Factors Influencing The Number Of Patients In Child
At the 0, 3, and 6 months, the number of patients with excessive drinking in Child-Pugh C class was highest among the three groups . Similarly, the number of non-drinking patients in Child-Pugh A class was the highest among the three groups . After 3â6 months of treatment, the number of patients in Child-Pugh C was still high .
Table 6Figure 4
What Is The Prognosis For Patients Who Have Alcoholic Hepatitis
If the patient who has alcoholic hepatitis gives up drinking alcohol completely, the liver may improve, and the long-term prognosis is good if there is no underlying scar in the liver. However, if the patient continues to drink excessively, the liver will continue to get worse and possibly develop cirrhosis, a serious condition that may ultimately lead to liver failure over time. Other health problems may also develop, including infections and malnutrition.
Last reviewed by a Cleveland Clinic medical professional on 06/21/2018.
References
Also Check: Hepatitis C Viral Rna Genotype Lipa
How Can Prevent Alcoholic Hepatitis
The best treatment is to stop drinking.
Treatment also may include:
- Hereditary defects in iron or copper metabolism
- Prolonged exposure to toxins
In children, the most frequent causes are biliary atresia â a disease that damages the bile ducts â and neonatal hepatitis. Children with these diseases often receive liver transplants.
Many adult patients who require liver transplants suffer from primary biliary cirrhosis. We do not yet know what causes this illness, but it is not in any way related to alcohol consumption.
Dont Miss: What Is Hepatic Steatosis Of The Liver
Don’t Miss: Ok Google What Is Hepatitis C
What Factors Increase Your Risk For Alcohol
The amount of alcohol you consume is the most important risk factor for developing alcohol-related liver disease. The risk increases with the length of time and amount of alcohol you drink. However, because many people who drink heavily or binge drink do not develop alcohol-related liver disease, we know there are other factors that affect a persons susceptibility. Additional risk factors that play a role in someone developing alcohol-related liver disease include:
Obesity: Obesity is a contributing factor to fatty liver disease. The combined effect of obesity and alcohol together is worse than the effect of either one of them alone.
Malnutrition: Many people who drink heavily are malnourished, either because they eat poorly due to loss of appetite and nausea or because alcohol and its toxic byproducts prevent the body from breaking down and absorbing nutrients. In both cases, the lack of nutrients contributes to liver cell damage.
Genetic factors: Genetics can influence how the body processes alcohol and may predispose someone to alcoholism and alcohol-related liver disease.
Race and ethnicity: A higher risk of liver injury appears to be associated with ones racial and ethnic heritage. For example, rates of alcoholic cirrhosis are higher in African-American and Hispanic males compared with Caucasian males.
What happens if you are an alcoholic and you contract hepatitis C?
Significant liver damage can be expected, even leading to cirrhosis.
When To Speak With A Doctor
Anyone who suspects they may have a liver condition should speak with a doctor as soon as possible. The sooner a healthcare professional diagnoses liver conditions, such as HCV and alcoholic hepatitis, the earlier treatment can begin. This may reduce the risk of permanent liver damage and complications.
Individuals can also speak with a doctor or a support organization if they find it difficult to reduce their alcohol consumption.
Seeking help for addiction may seem daunting or even scary, but several organizations can provide support. If you believe that you or someone close to you is struggling with addiction, you can contact the following organizations for immediate help and advice:
You May Like: Blood Test For Hepatitis C Virus
Demographic And Biochemical Data
There was no difference in the age of all male patients in the alcohol and alcohol-free groups . The median alcohol intake for Groups A and D was similar and was considered indicative of heavy alcohol consumption. The median alcohol intake for Group C was 65 g/day and this was considered as a group of moderate alcohol consumption. The AST/ALT ratio was > 1 for Group A, but was < 1 for the other groups. We did not find any significant difference in the serum levels of other biochemical parameters in these four groups except gamma-glutamyl transpeptidase and leucine aminopeptidase , which showed a higher value in Group A compared to the other groups .
Recommended Reading: What Does Hepatitis B Come From
Alcohol And The Liver
With the exception of the brain, the liver is the most complex organ in the body. Its functions include:
- filtering toxins from the blood
- aiding digestion of food
- regulating blood sugar and cholesterol levels
- helping fight infection and disease
The liver is very resilient and capable of regenerating itself. Each time your liver filters alcohol, some of the liver cells die.
The liver can develop new cells, but prolonged alcohol misuse over many years can reduce its ability to regenerate. This can result in serious and permanent damage to your liver.
ARLD is very common in the UK the number of people with the condition has been increasing over the last few decades as a result of increasing levels of alcohol misuse.
Read more about the causes of ARLD.
Recommended Reading: How Do You Treat Hepatic Encephalopathy
Causes And Risk Factors For Alcoholic Hepatitis
The main cause of alcoholic hepatitis is heavy drinking over an extended period of time. The process of breaking down alcohol in the liver causes inflammation that can destroy liver cells.
Over time, scars begin to replace functional liver tissue in the body. This interferes with how the liver works. Irreversible scarring, or cirrhosis, is the final stage of alcoholic liver disease.
Cirrhosis can quickly progress to liver failure once it develops. A damaged liver can also interfere with blood flow to the kidneys. This can result in damage and kidney failure.
Other factors can contribute to alcoholic hepatitis. For example, people with other types of hepatitis have a higher risk. As a result, it is not advisable for them to drink alcohol.
A person with alcoholic hepatitis may also experience malnourishment. Drinking significant amounts of alcohol can suppress the appetite. Alcohol may become the main source of calories for an individual. Malnutrition can also contribute to liver disease.
Other possible risk factors may include:
- sex assigned at birth, as females may have a
- electrolyte tests
- tests for other chemicals in the body
An ultrasound, CT scan, or MRI scan can show a more detailed view of the liver and any physical damage.
If other tests do not provide a clear answer, the doctor may conduct a liver biopsy. This involves taking a small tissue sample from the liver using a needle or through surgery for testing in a laboratory.
Toxic Effects On Cell Membranes
Ethanol and its metabolite, acetaldehyde, have been shown to damage liver cell membranes. Ethanol can alter the fluidity of cell membranes, thereby altering the activity of membrane-bound enzymes and transport proteins. Ethanol damage to mitochondrial membranes may be responsible for the giant mitochondria observed in patients with alcoholic hepatitis. Acetaldehyde-modified proteins and lipids on the cell surface may behave as neoantigens and trigger immunologic injury.
Read Also: What Is Hepatitis Panel Acute With Reflex To Confirmation
Clinical Supervisor Primary Therapist
Vanessa is certified in addictions counseling by Marylands Board of Professional Counselors and Therapists, with credentials as a clinical supervisor. She comes to The Freedom Center with over 14 years of direct experience in residential and outpatient treatment between the private and federal sectors.
In addition to helping those suffering from addiction, Vanessa has dedicated part of her career to helping the helper. In 2015, she began working in a Training and Career Development Center coordinating substance abuse trainings for other clinicians. Her experience in behavioral health training, program development, and organizational leadership lead her to pursue a certification as a Project Management Professional in 2018. Vanessa also holds a Bachelors of Arts in Behavioral and Social Sciences from the University of Maryland, College Park and a Masters of Business Administration-Human Resource Management from Columbia Southern University.
Vanessa is a Montgomery County native who spends her free time traveling with her daughter and volunteering in the community.
Diagnosis Of Hcv Infection
HCV liver disease was confirmed in each patient by the detection of anti-HCV antibody in serum tested by second generation radioimmunoblot assay or serum HCV RNA by the the polymerase chain reaction. All patients with hepatitis B surface antigen positivity and immunological disorders of chronic liver disease were excluded from our study. Patients who had not received interferon therapy before liver biopsy were included in this study. HCV RNA was measured in serum by the signal amplification technique employing branched deoxyribonucleic acid in a sandwich hybridization assay . Serum HCV RNA titres were expressed as mega equivalent copies of viral genome per millilitre of serum .
Recommended Reading: What Hepatitis Vaccines Are There
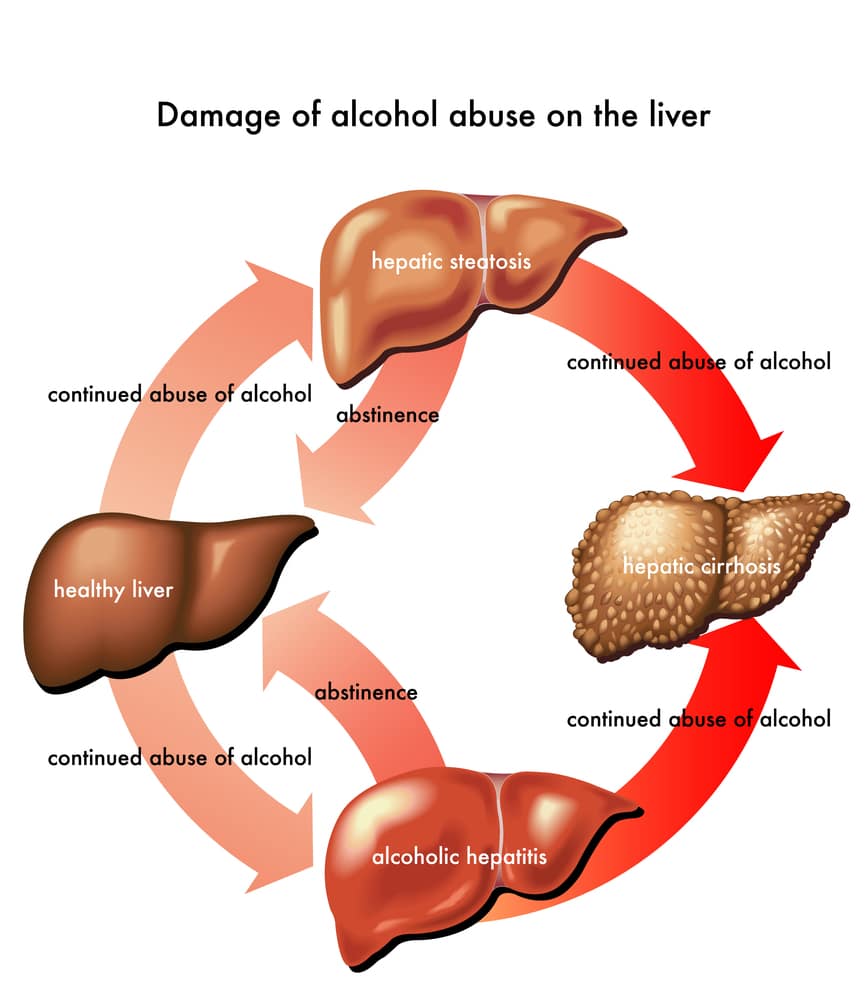
Types Of Alcohol Related Liver Disease
- Alcholol Related Steatohepatitis : Fat accumulates inside liver cells, making it hard for the liver to work properly. This early stage of liver disease occurs fairly soon after repeated heavy drinking. Usually it is symptom free but upper abdominal pain on the right side from an enlarged liver may occur. Steatosis goes away with alcohol abstinence.
- Alcoholic Hepatitis: This condition is marked by inflammation, swelling and the killing of liver cells. This scars the liver, which is known as fibrosis. Symptoms may occur over time or suddenly after binge drinking. They include fever, jaundice, nausea, vomiting, abdominal pain and tenderness. Up to 35 percent of heavy drinkers develop alcohol hepatitis, which can be mild or severe. If it is a mild case, stopping the drinking can reverse it.
- Alcohol Related Cirrhosis: The most serious form of ALD, it occurs when the entire liver is scarred, causing the liver to shrink and harden. This can lead to liver failure. Usually the damage cannot be reversed. Between 10 to 20 percent of heavy drinkers develop cirrhosis typically after 10 or more years of drinking.
Alcohol hepatitis and alcohol cirrhosis previously were called alcohol steatohepatitis , a term that still arises among some circles.
International Travel And Hepatitis A
If you are planning to travel to countries where hepatitis A is common, talk to your doctor about getting vaccinated before you travel. Travelers to urban areas, resorts, and luxury hotels in countries where hepatitis A is common are still at risk. International travelers have been infected, even though they regularly washed their hands and were careful about what they drank and ate.
Read Also: Where Can I Get Hepatitis B Vaccine For Free
How Is It Diagnosed
- Medical history. Your doctor may ask about your medical past to see if thereâs reason to believe you may have alcohol-related liver problems.
- Questionnaire. Theyâll ask you questions to determine if your drinking has become a problem.
- Blood tests. These will check your liver enzymes. Abnormally high levels are a sign of liver damage.
- Liver biopsy. Your doctor may request one in addition to blood tests.
How Can Alcohol Use Cause Hepatitis
Every food and drink you consume passes through your liver for processing. Your liver helps metabolize nutrients and filters out toxins. When alcohol goes to your liver for processing, it acts as a toxin. It offers no nutritional value and instead breaks down into poisonous chemicals.
Chronic heavy alcohol use can overload your liver with fat and toxins to process. When your liver can no longer keep up, these toxins and fat build up and begin to injure your liver. The injury produces an inflammatory response. This is your bodys way of attempting to heal and ward off further injury.
Like a fever, inflammation is supposed to be a temporary intervention. But when the assault is constant, the inflammation becomes constant. In your liver, this means swelling with fluid. If the swelling is severe and persistent, over time it will damage the tissues, causing cell death.
Read Also: Hepatitis B Is More Infectious Than Hiv True Or False
Don’t Miss: Hepatitis C Treatment Center Louisville Ky
Increased Risk Of Hepatocellular Carcinoma
Hepatocellular carcinoma is the most common form of liver cancer in the U.S., and one of the more common complications of chronic hepatitis C infection. Even more so than liver cirrhosis, the association between alcoholism and HCC is strong, with 80% of HCC cases being identified as heavy alcohol users.
The risk appears to increase with the amount a person drinks. One Italian study showed that the likelihood of HCC doubled when a person drank between 3.4 and 6.7 drinks per day. Similarly, studies have shown that heavy drinking can accelerate the development of HCC by as much as five years, resulting in not only larger tumors but far shorter survival times.
Can Alcoholic Hepatitis Be Fatal
Yes, it is estimated that 1 in 3 with this condition will die from it. Often, it isnt until the majority of the liver has been critically damaged that there is any outward indication that there is a problem. By the time pain or some other symptom makes itself known, the liver damage is extensive and the organ is likely in critical condition.
Don’t Miss: Food To Cure Hepatitis B
How Is Hepatitis Diagnosed
To diagnose hepatitis, your health care provider:
- Will ask about your symptoms and medical history
- Will do a physical exam
- Will likely do blood tests, including tests for viral hepatitis
- Might do imaging tests, such as an ultrasound, CT scan, or MRI
- May need to do a liver biopsy to get a clear diagnosis and check for liver damage
Formation Of Acetaldehyde Adducts
Acetaldehyde may be the principal mediator of alcoholic liver injury. The deleterious effects of acetaldehyde include impairment of the mitochondrial beta-oxidation of fatty acids, formation of oxygen-derived free radicals, and depletion of mitochondrial glutathione. In addition, acetaldehyde may bind covalently with several hepatic macromolecules, such as amines and thiols, in cell membranes, enzymes, and microtubules to form acetaldehyde adducts. This binding may trigger an immune response through the formation of neoantigens, impair the function of intracellular transport through precipitation of intermediate filaments and other cytoskeletal elements, and stimulate hepatic stellate cells to produce collagen.
The levels of acetaldehyde in the liver represent a balance between its rate of formation and its rate of degradation by ALDH. ALDH is downregulated by long-term ethanol abuse, with resultant acetaldehyde accumulation.
Recommended Reading: What Causes Hepatitis C Symptoms
What Causes Alcoholic Hepatitis
When alcohol gets processed in the liver, it produces highly toxic chemicals. These chemicals can injure the liver cells. This injury can lead to inflammation and, eventually, alcoholic hepatitis.
Although heavy alcohol use can lead to alcoholic hepatitis, experts arent entirely sure why the condition develops in some people but not in others.
Alcoholic hepatitis develops in a minority of people who heavily use alcohol no more than 35 percent, according to the American Liver Foundation. It can also develop in people who use alcohol only moderately.
Because alcoholic hepatitis doesnt occur in all people who heavily use alcohol, other factors may influence the development of this condition.
Risk factors include:
- having genetic factors that affect how the body processes alcohol
- living with liver infections or other liver disorders, such as hepatitis B, hepatitis C, and hemochromatosis
- abdominal CT scan
- ultrasound of the liver
Your doctor may order a liver biopsy to confirm a diagnosis of alcoholic hepatitis. A liver biopsy requires your doctor to remove a tissue sample from the liver. Its an invasive procedure with certain inherent risks, but biopsy results can show the severity and type of liver condition.
Common Symptoms Of Hepatitis
If you are living with a chronic form of hepatitis, like hepatitis B and C, you may not show symptoms until the damage affects liver function. By contrast, people with acute hepatitis may present with symptoms shortly after contracting a hepatitis virus.
Common symptoms of infectious hepatitis include:
It is crucial to understand what is causing hepatitis in order to treat it correctly. Doctors will progress through a series of tests to accurately diagnose your condition.
Don’t Miss: How To Know If I Have Hepatitis
Alcoholic Hepatitis Vs Cirrhosis
Cirrhosis is a permanent scarring of the liver.10 It is not the same condition as hepatitis, but it often develops as a result of it.
While liver damage from hepatitis is sometimes reversible, cirrhosis is not. And the more scar tissue you have in your liver, the harder it becomes for this vital organ to function. This can have many serious consequences for your overall health, and can eventually cause liver failure, which can be fatal. While some milder cases of cirrhosis are manageable, the only treatment for advanced cirrhosis is a liver transplant.
Unfortunately, cirrhosis is on the rise, making it more important than ever to raise awareness of this condition. And since alcoholic hepatitis can lead to cirrhosis, the sooner you catch liver damageand reduce your alcohol consumptionthe better.
Also Check: How Is Hepatitis C Test Done
Its Not Too Late To Get Help
The good news is that if acted upon early enough, alcohol hepatitis can be reversed. The liver has an incredible ability to repair itself, in fact, after part of it has been surgically removed the liver can regenerate itself in only a matter of months. However, continued alcohol damage can destroy this capability so it is imperative that those with this condition immediately cease alcohol consumption. Time is of the essence to get your drinking habit under control but quitting cold turkey is never recommended. Alcohol rehab facilities like the Freedom Center can help safely mitigate alcohol withdrawal symptoms and ultimately, help you achieve life-saving abstinence.
by The Freedom Center | Last updated Aug 16, 2022 | Published on Aug 25, 2022 | Alcohol, Mental Health
If youre taking an antidepressant, its important to understand the risks of combining alcohol with this medication. Alcohol is a depressant, so mixing it with antidepressants can make you feel worse. You may have more side effects from your antidepressants when
by The Freedom Center | Last updated Aug 16, 2022 | Published on Aug 16, 2022 | Addiction Treatment, Alcohol
If youre struggling with alcoholism or just want to cut back on alcohol consumption, there are two main options: cold turkey and tapering off. Both involve quitting drinking, but tapering off involves slowly reducing the alcohol consumed over time until youre no
Recommended Reading: Can You Get Hepatitis C Sexually