What Is The Treatment Of An Acute Porphyria
The pain of acute attacks can be severe, requiring hospitalisation for pain management and a work-up for other possible causes of pain. Severe electrolyte imbalance, respiratory distress, or seizures should prompt admission to intensive care.
Recommended treatments to suppress ALAS1 include :
- Glucose , providing sodium is normal and stable
- Intravenous haematin given through a central line line or an implanted Portacath®
- Recent evidence has suggested that haematin may promote inflammation and increase the risk of recurrent attacks so it should only be used in confirmed attacks .
Drugs that are potential triggers of acute attacks must be avoided. The drugs below are considered safe at the time of writing .
How Do Porphyrias Affect Eating Diet And Nutrition
If you have acute porphyria, your doctor may recommend a balanced diet in which 60 to 70 percent of your calories come from carbohydrates.8 Lowering your intake of carbohydrates and calories, even for a short time, can cause an acute porphyria attack. Talk with your doctor or a dietitian before changing your diet to try to lose weight. They can help you plan a safe diet to lose weight gradually.
People with cutaneous porphyrias who need to avoid sunlight may have lower levels of vitamin D. Doctors may recommend vitamin D supplements to treat low vitamin D levels.
Most Common Symptoms Of Acute Hepatic Porphyria
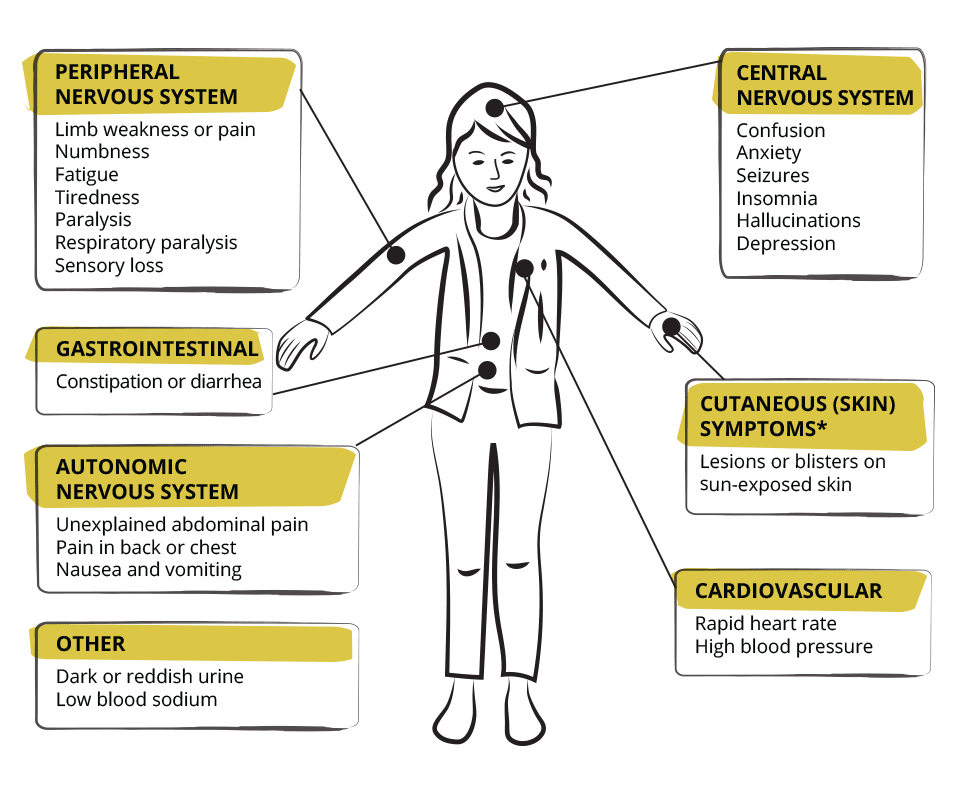
People with AHP can experience gastrointestinal, neurologic, psychiatric, cardiovascular, or skin symptoms. The most common symptom is abdominal pain which can be severe and last several hours.
Those with AHP can also experience chronic symptoms. These are symptoms that last a long time and may include:
- anxiety
- depression
- fatique- feeling overly tired or having low energy
- nausea- feeling of sickness in the abdomen, stomach, chest, or head with feeling an urge to vomit
- pain- physical discomfort and/or suffering in the body
Recommended Reading: Hepatitis B Vaccine Dose For Newborns
When Is The Best Time To Be Tested For Acute Prophyria
The best time to be tested for porphyria is at the earliest opportunity. In practice, this means that families should be offered screening for acute porphyria as soon as possible after a relative has been found to have the condition. When one or other parent is already known to have an acute porphyria, their children should be tested as soon as possible, and in some countries babies can be tested at or soon after birth. It may be necessary to wait until your child is older, but it is recommended that testing takes place before onset of puberty. It is extremely rare for children to have a porphyria attack but there are two main advantages of early diagnosis. First, those who are found to have inherited one of the acute porphyrias can be advised about how to reduce their risk of an acute attack. Second, if an acute attack does develop, your doctor will be able to confirm the diagnosis and start treatment early.
What Causes Acute Hepatic Porphyria
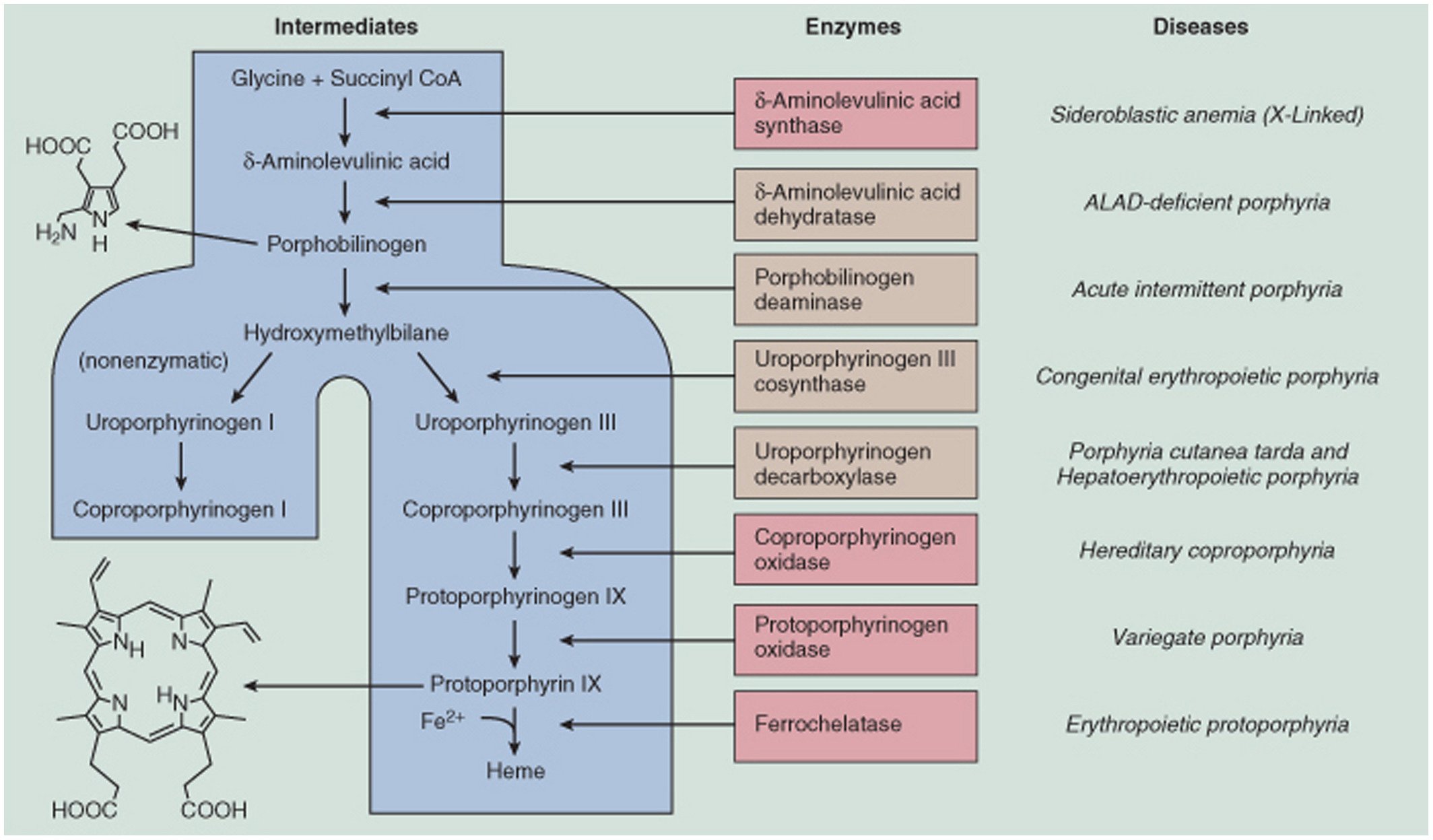
Porphyrins are natural chemicals in your body. They are made by your body when it creates something called heme.
Heme is part of hemoglobin — the protein in red blood cells that carries oxygen from your lungs to the rest of your body. It’s critical for many body functions, like in the liver and muscles. It’s also found in bone marrow.
When heme is made in your bone marrow and liver, eight enzymes are needed for the process to work properly. If there’s a shortage in one of those enzymes, your levels of porphyrins could go up. Which of the eight enzymes is low and where the porphyrins are in your body determine which type of porphyria you have. With acute hepatic porphyria, there is a buildup of porphyrins in your liver.
That can cause problems, usually in your skin or with your nerves. You could also have:
- Dark urine
- Nausea
- Seizures
An attack usually starts with severe stomach pain and can last for days. You’ll usually need to go to the hospital for treatment.
Read Also: What Is The Test For Hepatitis B
The Acute Attack Clinical Manifestations
The symptoms individually are nonspecific but in aggregate may suggest the diagnosis . Attacks occur mainly in females age 15 to 45. They are rare prior to menarche and become less likely after menopause. The most common symptom is abdominal pain, which is usually diffuse. In some patients, it is localized to the back or an extremity. By the time the patient is seen, pain has increased relentlessly for several days, not hours, often accompanied by nausea, vomiting, and constipation. Fever and leukocytosis are not present in the absence of an accompanying infectious process. Mild elevation of the transaminases is common. Hyponatremia may be seen and occasionally is severe. Because patients tend to present dehydrated after several days of nausea and inadequate oral intake, hyponatremia may be masked initially by hemoconcentration but can develop rapidly after rehydration with dextrose in water. The pathophysiology is debated. In some cases it appears to be a form of inappropriate ADH secretion ) due to pituitary central nervous system dysfunction urine osmolarity can be high, consistent with SIADH. In others, hypovolemia may be the underlying problem.
The Acute Porphyric Attack
The symptoms and signs of attacks are nonspecific and can mimic many other disease processes. Constipation, fatigue, mental status changes , and insomnia typically precede an acute attack. The most common symptoms of an attack are abdominal pain and vomiting. The pain may be excruciating and is disproportionate to abdominal tenderness or other physical signs. Abdominal manifestations may result from effects on visceral nerves. Usually, there is no inflammation, the abdomen is not tender, and there are no peritoneal signs. However, a minority of patients with acute hepatic porphyrias also develop acute pancreatitis Acute Pancreatitis Acute pancreatitis is acute inflammation of the pancreas . The most common triggers are gallstones and alcohol intake. The severity of acute pancreatitis is… read more , for which alternative potential causes, such as gallstones, excess alcohol use, and severe hypertriglyceridemia, are not found. Temperature and white blood cell count are usually normal or only slightly increased. Bowel distention may develop as a result of paralytic ileus. The urine is red or reddish brown and positive for porphobilinogen during an attack.
Also Check: How To Check For Hepatitis
Missed Diagnosis And Misdiagnosis
In the urgent care setting, porphyria is often overlooked as a diagnostic possibility, because the symptoms are those of far more common conditions. When the initial screening tests for the common conditions are negative, patients usually are discharged with a diagnosis of viral gastroenteritis, irritable bowel syndrome, addiction withdrawal, or psychosomatic pain. A recent study of U.S. patients with genetically confirmed acute porphyria found that the diagnosis was delayed by an average of 15 years from the onset of symptoms . The case presented above is unusual, in that a perceptive resident physician thought of the diagnosis and ordered the correct test, a urine PBG.
The number of people who have been misdiagnosed and believe, erroneously, that they have acute porphyria far exceeds those with a confirmed diagnosis. When they come to an ED, very few will have documentation of their diagnosis. In this situation, a rapid PBG would be definitive but, as discussed above, is not available. Although neurological complications are not a concern in this group, a test that excludes acute porphyria would redirect attention to other possible causes of the patient’s complaints and potentially avoid an expensive and unproductive hospitalization.
Recurrent Attacks Of Porphyria
A few patients, mostly those with AIP, develop a pattern of recurrent attacks, usually defined as four or more attacks requiring admission to hospital for treatment in one or more years. In women these attacks may be related to the normal hormone changes of the menstrual cycle with symptoms typically starting in the week or so before menstruation, but in many patients, there is no clear trigger for their attacks. Patients with recurrent porphyria attacks should be referred to a specialist porphyria centre if possible so they can get the best possible care. The main treatment is to give regular infusions of hemin to try to prevent attacks. In very severe cases, liver transplantation may be considered. A new treatment for recurrent attacks of porphyria gave very promising results in clinical trials but is not yet available to patients in all countries.
Also Check: Hepatitis C Causes Symptoms And Treatment
Also Check: How Is Hepatitis B Transmitted
Biochemical Diagnosis Of Acute Porphyria
In all three autosomal dominant acute porphyrias, attacks are accompanied by a clear increase in PBG , which, for convenience, is generally assessed in urine rather than blood. In active AIP, the type most commonly associated with acute attacks, the PBG is at least 10-fold the upper limit of normal, more typically 20- to 100-fold. A urine PBG of > 50 mg/g creatinine in a patient with pain symptoms of unknown cause is highly specific for the diagnosis occasional genetic carriers have PBG levels in this range even when feeling well and thus represent false-positive cases. While this is unusual, it highlights the importance of having baseline information from urine samples that are collected when the patient is feeling well. ALA should be evaluated at the same time to identify cases of lead poisoning, which can mimic acute porphyria. It would also identify the rare individual with ALA dehydratase deficiency.
The Neuromuscular Manifestations Of Acute Hepatic Porphyria And Their Pathophysiological Mechanisms
Neurological manifestations in AHP can be related to dysfunction of the central, peripheral, or autonomic nervous system. AHP should be always remembered as an important differential diagnosis for acquired and inherited neuromuscular disorders . In this section, we describe in detail the most common neuromuscular manifestations of AHP and the pathophysiological mechanisms involved with them.
Read Also: Hepatitis B Vaccine Cost Walgreens
How Is An Acute Porphyria Diagnosed
Porphyria may be suspected clinically, but must be confirmed by laboratory tests .
The most important immediate test is a measurement of light-protected urinary porphobilinogen.
- A normal porphobilinogen in an unwell patient excludes acute porphyria.
- A false positive can occur in dehydrated patients with concentrated urine a quantitative urinary porphobilinogen corrects for creatinine and can overcome this problem.
Urinary porphyrins may also rise in an acute attack, but are less specific as urinary porphyrins may occur in infections, hepatobiliary disease, haematological disorders, heavy metal exposure, and lead poisoning.
Once an acute attack is confirmed, blood and faecal samples are tested to determine the subtype of porphyria. Samples should be sent to an accredited laboratory or one familiar with porphyria testing .
A skin biopsy of cutaneous lesions in variegate porphyria and hereditary coproporphyria has similar findings to porphyria cutanea tarda.
Screening of relatives is essential as the majority of people with the geneticmutation will have clinically latent disease but are at risk of developing acute attacks and should heed the same advice regarding triggers.
Heme Biosynthesis And Regulation
Heme is required for a variety of hemoproteins, including hemoglobin, myoglobin, respiratory cytochromes, and the cytochrome P450 enzymes. Hemoglobin synthesis in erythroid precursor cells accounts for 85% of daily heme synthesis in humans. Hepatocytes account for most of the rest, primarily for synthesis of cytochrome P450 enzymes, which are especially abundant in the liver endoplasmic reticulum, and turn over more rapidly than many other hemoproteins, such as the mitochondrial respiratory cytochromes.
Read Also: How Serious Is Hepatitis C
Recommended Reading: Hepatitis A Curable Or Not
What Are The Complications Of Acute Hepatic Porphyria
Complications of porphyria can include :
- Seizures, neuropathies, and rarely, posterior reversible encephalopathy
- Hyponatraemia due to secretion of inappropriate antidiuretic hormone
- Tachyarrhythmias
- A variety of psychiatric features.
Longer-term complications include:
- Hypertension
- Scarring and thickened skin in those with skin lesions.
Given the severity and recurrent nature of the pain, porphyria patients may be at increased risk of opioid misuse and dependence .
Treatment Of Recurrent Attacks:
In recurrent attacks that appear linked to the menstrual cycle, ovulatory suppression with gonadotropin-releasing hormone agonists may be helpful . GnRH agonists are peptides that have no demonstrable porphyria-inducing activity . The main adverse effect is menopausal symptoms, which are not tolerated by some patients. Supplemental low-dose estrogen may be helpful for those whose porphyria symptoms are improving on treatment.
Patients who experience more than 34 attacks per year should consider prophylactic hematin therapy . Monitoring of ALA and PBG between attacks is helpful for optimizing the timing of prophylactic hematin therapy. Regular, long-term administration of hematin typically requires the placement of an indwelling venous catheter for access. Patients should be monitored for complications related to chronic hematin administration such as iron overload.
Read Also: How Do You Prevent Hepatitis C
Liver And Kidney Transplantation
Orthotopic liver transplantation has been successful and indeed curative in patients with severe, disabling, intractable attacks that are refractory to hemin therapy. Because orthotopic liver transplantation is associated with morbidity and mortality, it is considered a treatment of last resort. In addition, patients who already have advanced neuropathy with quadriplegia and respiratory paralysis are considered poor candidates for transplantation.-
AIP patients with advanced renal disease tolerate and benefit from renal transplantation, and exacerbations of porphyria do not occur with exposure to commonly used immunosuppressive agents. Rarely, AIP patients with end-stage renal disease develop elevations in plasma porphyrins and blistering skin lesions, resembling those seen in porphyria cutanea tarda, and respond well to renal transplantation. Some patients with both repeated attacks and end-stage renal disease have benefited from combined liver and kidney transplantation.
No Recurrent Aip Attacks With Givlaari Small Real
I co-parent two sweet, insightful, hilarious, and clever kiddos. I love being a bonus in their lives, and their places in my heart certainly fill what was once a gaping void. However, quelling the primal, biological pull of motherhood took real intention.
In the last two years, more people in my close circle were expecting children than werent. All of a sudden, girlfriends whod never grown a human were doing just that. While I was genuinely happy for the new and expecting moms in my life, Ive been in a place where another persons good fortune angered me, particularly as it related to the limitations imposed on my life with acute hepatic porphyria . Its an ugly hole I never wish to fall into again.
I grieved for a traditional version of motherhood, either through pregnancy or adoption. My decision was less about passing along a genetic mutation for AHP and more about ensuring I had the ability to parent full time, with the energy and stability to provide for a baby while managing AHPs chronic symptoms.
On Mothers Day weekend, I experienced mixed emotions as I celebrated the moms in my life. I noticed my inner critic had a lot to say. First came thoughts about somehow being less of a woman because I wasnt going to have a baby. Then, judgment emerged about once again going against the collective social grain, and defining a separate set of life milestones on my own path.
It becomes overwhelming, and theres nothing like Mothers Day to dredge it all up again.
Recommended Reading: Is Hepatitis C Transferred Sexually
How Can I Prevent An Acute Porphyria Attack
- Do not smoke cigarettes or drink alcohol: Cigarettes and alcohol can make your acute porphyria worse. They may also damage the liver and further worsen your problems. Talk to your healthcare provider if you have trouble quitting smoking or drinking.
- Eat enough food: You can trigger an attack if you do not eat enough, especially if you cut out carbohydrates. Ask your healthcare provider how much you should eat each day. You may need to work with a dietitian to create a food plan.
- Reduce stress: Try to decrease or avoid stress. Ask healthcare providers how you can learn to relax.
- Be careful with medicines: Certain medicines can trigger an acute porphyria attack, so ask your healthcare provider about the medicines you take.
High Blood Pressure And Kidney Problems
If you have acute porphyria, your doctor may check for complications such as high blood pressure and chronic kidney disease, which may lead to kidney failure. Your doctor may prescribe medicines to lower blood pressure and recommend steps to manage chronic kidney disease or treatments for kidney failure.
Read Also: How Long Does Hepatitis A Vaccine Last
Treating Acute Hepatic Porphyria
When someone with AHP is experiencing an acute attack, treatment with intravenous hemin in the hospital can help with symptoms. At that time, it is also important to try to identify what may have caused the attack so that they can be avoided in the future.
A drug called Givosiran was approved by the U.S. Food and Drug Administration in 2019 for the treatment of adults with AHP. It is a medicine that is injected under the skin once a month. In clinical trials, patients on givosiran had fewer acute attacks from AHP when compared to those given a placebo. A placebo is a pill or treatment with no active ingredients. While taking givosiran, patients should have their liver and kidney tests monitored by their healthcare team. For patients with AHP who suffer from repeated severe attacks, do not respond to IV hemin or givosiran, or have a very poor quality of life, liver transplantation can be considered as a last resort.
Adapted from IFFGDs publication #581 Understanding Acute Hepatic Porphyria by Christopher V. Almario, MD, MSHPM Cedars-Sinai Medical Center, Karsh Division of Gastroenterology and Hepatology
Pathophysiology Of Neurovisceral Pain In Acute Porphyria

The metabolic changes underlying acute porphyria have been well-delineated for more than 40 years, yet for most of that time their role in the pathogenesis of neurovisceral attacks has been unclear. Research has focused on two hypotheses that are not mutually exclusive. The first is heme deficiency, which could directly affect neuronal function in that these cells, like hepatocytes, require heme for synthesis of essential heme proteins. One such protein is tryptophan pyrrolase, which has a relatively low affinity for heme but requires it for enzymatic activity. When heme is scarce, the activity drops, potentially shifting tryptophan metabolism from the kynurenine pathway to 5-hydroxytryptamine , a neurotransmitter. Although certain aspects of acute porphyria suggest a serotonergic state, human data to confirm this postulate are lacking.
Also Check: Can Hepatitis B Virus Be Cured