Hbv Chronic Infection And New Biomarkers
The HBV is a DNA virus that belongs to the Hepadnaviridae family.3 The virus replicates and assembles in the hosts hepatocytes, and the virions are released through the cell secretory pathways. After the virus enters the hepatocytes, the HBV is transported to the nucleus to release the relaxed circular DNA genome. In the nucleoplasm, the rcDNA becomes a covalently closed circular DNA that can use the host-cell DNA repair mechanism and can serve as a transcription template for all viral transcripts that are translated into the different viral proteins.4 In addition to complete infectious virions, infected cells produce free, non-infectious sub-viral spherical or filamentous particles.5 Integration of the viral genome into the host genome may occur randomly it is not necessary for viral replication, but it is one of the mechanisms involved in the hepatocyte transformation and carcinogenesis.6 Phylogenetic analyses of isolated HBV strains have identified 10 major genotypes that have a different distribution worldwide.7
An important aspect to consider is the correlation between ethnicity and HBV genotype. The HBV genotypes B and C are endemic in South East Asia, and genotype D is most prevalent in countries bordering the Mediterranean basin.10 This genotype distribution is important for the interpretation of studies on the influence of HBV genotype and other factors in determining the probability of response to treatment strategies.
Is Hepatitis B Curable
Theres no cure for hepatitis B. The good news is it usually goes away by itself in 4 to 8 weeks. More than 9 out of 10 adults who get hepatitis B totally recover.
However, about 1 in 20 people who get hepatitis B as adults become carriers, which means they have a chronic hepatitis B infection. Carriers are more likely to pass hepatitis B to other people. Most carriers are contagious meaning they can spread hepatitis B for the rest of their lives.
Hepatitis B infections that last a long time may lead to serious liver diseases like cirrhosis and liver cancer. About 1 in 5 people with chronic hepatitis B die from it. There are medicines that can help treat chronic hepatitis B infections.
Most babies who get hepatitis B during birth develop chronic infection, unless they get treated right away. But treatments are almost always effective if your baby gets them quickly. Thats why its important for pregnant people to get tested for hepatitis B.
Durability And Related Factors After Hbsag Clearance
When patients with HBeAg-positive CHB achieve a satisfactory antiviral treatment endpoint , the clinical recurrence is 2040%, and the virological recurrence can be as high as 8090% after drug withdrawal . Because the safety of drug withdrawal is uncertain, HBsAg clearance is recommended as the ideal treatment endpoint for CHB patients. The accessibility and rate of HBsAg clearance was mentioned above, but the durability of HBsAg clearance after treatment cessation remains controversial.
HBeAg status should also receive attention in the pursuit of HBsAg clearance. The clearance of HBsAg in most patients is based on HBV DNA suppression and HBeAg seroconversion, but a few patients exhibit different HBsAg response patterns, such as HBsAg clearance without HBeAg seroconversion. Only HBsAg clearance based on HBV DNA suppression and HBeAg seroconversion is safe for drug withdrawal .
You May Like: Hepatitis B Surface Ab Immunity
Hbsag Clearance After Na Treatment
There are few large or conclusive studies on the clearance of HBsAg after NA treatment, and some of these studies are single-centre retrospective studies. Kim et al. reported a clearance rate of 1% or less in 110 CHB patients who were treated with ETV/LAM for approximately 1 year. A retrospective study by Yip et al. reported an HBsAg clearance rate of 2.1% after an average follow-up of 4.8 years in 20,263 CHB patients treated with ETV/TDF for longer than 6 months. Wong et al. retrospectively evaluated 1072 CHB patients on antiviral therapy for approximately 6 years and found an HBsAg clearance rate of 4.58%. This study found no significant difference in the clearance rate between HBeAg-positive and HBeAg-negative patients, but the rate in patients with cirrhosis was significantly lower than patients without cirrhosis . These results suggested that the clearance rate of non-cirrhosis patients was higher after NA treatment, which is not consistent with the results of patients who experienced spontaneous clearance. Compared to patients with normal baseline ALT, patients with higher ALT levels had significantly higher rates of achieving HBsAg clearance. In general, the clearance rate may increase with the extension of treatment in CHB patients, but the overall rate with currently available NA treatment is low. The HBsAg clearance rates were 1.45.1% after an average follow-up of 27 years after NA treatment .
What Is Chronic Hepatitis
Hepatitis is an inflammation of the liver. In chronic hepatitis, liver inflammation continues for at least six months. This condition may be mild, causing relatively little damage, or more serious, causing many liver cells to be destroyed. Some cases lead to cirrhosis and liver failure.
Chronic hepatitis from infection is most often caused by these viruses:
- Hepatitis B and C. Often the person infected is unaware of any initial symptoms. Or the symptoms were so mild that the person did not seek medical attention. This is especially true for chronic hepatitis C. Over time, perhaps a decade or more, both types may lead to the serious complication of cirrhosis due to ongoing destruction of liver cells and resultant scarring. A minority of patients with cirrhosis develop liver cancer over time.
- Hepatitis D. Hepatitis D infects only patients already infected with hepatitis B, and it generally results in a flare of active hepatitis.
This information helps to determine the best treatment and to assess your risk of developing cirrhosis and liver failure. A liver biopsy also can help to check for other disorders, such as alcoholic liver injury or fatty liver.
You May Like: Hepatitis B Virus Surface Ab
Specific Therapy For Acute Hepatitis Delta Virus Infection
Since the start of vaccination against HBV, a decline in the incidence of acute hepatitis delta virus infection has been observed in many regions . HDV requires ongoing expression of HBV surface genes to be able to infect a host, but it does not require HBV replication. Simultaneous coinfection with both HBV and HDV is associated with more severe disease and higher risk for fulminant hepatitis than acute HBV alone however, HDV superinfection may also present as acute hepatitis . In general, coinfection is more likely to lead to severe acute presentation, but rarely leads to chronicity, while superinfection of HDV usually leads to chronicity . For example, 2 of 218 HDV coinfected patients but none of 128 HDV superinfected patients died from consequences of acute hepatitis .
Dont Miss: How Do You Get Hepatitis B
Safety Of Na Withdrawal
Safety of this strategy is a major concern as NA is a well-tolerated treatment with few side effects. An important issue to evaluate after NA interruption is the risk of developing HCC. In the study of Jeng82 that included patients without cirrhosis and with cirrhosis , the HCC incidence at 1-, and 3-years after withdrawal was 0.15% and 1% for non-cirrhotic patients and 1.3% and 4% for those with cirrhosis. However, the incidence during therapy was similar . Therefore, treatment cessation did not increase the HCC development. In the RETRACT-B study,95 the HCC incidence at 48 months after NA withdrawal was 2.2% in patients with cirrhosis and only 0.7% in those without cirrhosis.
Recommended Reading: Tenofovir Disoproxil Fumarate For Hepatitis B
Treatment For Antiviral Resistance In Children
The 2015 APASL guidelines recommend that tenofovir or IFN should be used for the treatment of children who develop lamivudine resistance. When adefovir resistance develops, the guidelines recommend that entecavir or tenofovir should be used if the child has no history of NA treatment before receiving adefovir .
Natural History Of Hepatitis B Virus
In contrast to many known pathogens, hepatitis B virus is not directly cytopathic to hepatocytes. Although not completely understood, the injury to the liver cells is in part through a host immune mechanism. Replicating HBV in hepatocytes produces HBsAg particles and virions which are taken up by the antigen presenting cells. The viral proteins are degraded to peptides, which are presented on the cell surface bound to MHC class I or II molecules. MHC class I molecules are recognized by CD8 T cells and MHC II by CD4 T cells. Virusspecific CD8+ cytotoxic T cells, with help from CD4+ T cells, recognize viral antigens presented on MHC class I chains on infected hepatocytes. This recognition reaction can lead to either direct lysis of the infected hepatocyte or the release of interferon a , which can downregulate viral replication in surrounding hepatocytes without direct cell killing .
In order to further discuss advancements in the understanding and treatment of HBV, it is important first to review the natural history of the disease. The cycle of chronic HBV infection primarily consists of five phases as shown in Figure 1 .
Figure 1.
Five phases of chronic hepatitis B *. * Adapted from Tong et al. and modified by HalegouaDeMarzio and Hann .
It is important to remember that once patients are infected, they remain positive for antiHBc IgG throughout even after they lose HBsAg and after they acquire antiHBs. Also, antiHBe may often remain detectable.
Recommended Reading: Can You Live A Normal Life With Hepatitis C
Special Considerations During Immunosuppressive Therapy
With immunosuppressive therapy, both in the context of malignancy and rheumatologic/autoimmune diseases, reactivation of HBV infection can occur. HBV reactivation in HIV-negative people with HBsAg-positive/anti HBc-positive disease receiving immunomodulatory therapy is well described.147,148 Even among people with HBsAg-negative/anti-HBc-positive disease, HBV reactivation occurs in 8% to 18% of people receiving anti-cancer drugs149 and 1.7% of people receiving rheumatologic disease drugs.150
Management Of Chronic Hbv Carriers And Inactive Hbsag Carriers
Because chronic HBV carriers are in the immune tolerance phase, they do not have or only have mild inflammatory activity in the liver, patients in this phase respond poorly to antiviral treatment. Therefore, antiviral therapy is not recommended. However, it is emphasized that some patients in the immune tolerance phase might enter the immune clearance phase and develop hepatitis flares. Inactive HBsAg carriers are in the immune control phase, but they might progress to HBeAg-negative CHB and are at risk of developing HCC in long-term follow-up.
Therefore, for chronic HBV carriers and inactive HBsAg carriers, it is recommended that they should undergo routine blood tests, biochemical tests, virological tests, AFP tests, abdominal ultrasound, and noninvasive tests for liver fibrosis every 612 months. A liver biopsy is recommended if necessary. Antiviral therapy should start if they meet the indications for such treatment.
Recommended Reading: How Do You Hepatitis B
How Is Hepatitis B Treated
Your healthcare provider will treat you based on what type of hepatitis B you have, acute or chronic.
Acute hepatitis B infections
If you develop an acute form of the condition, you probably wont need medical treatment. Instead, your doctor will likely suggest that you get plenty of rest, drink lots of fluids and maintain a healthy diet to support your body as it fights off the infection.
Chronic hepatitis B infections
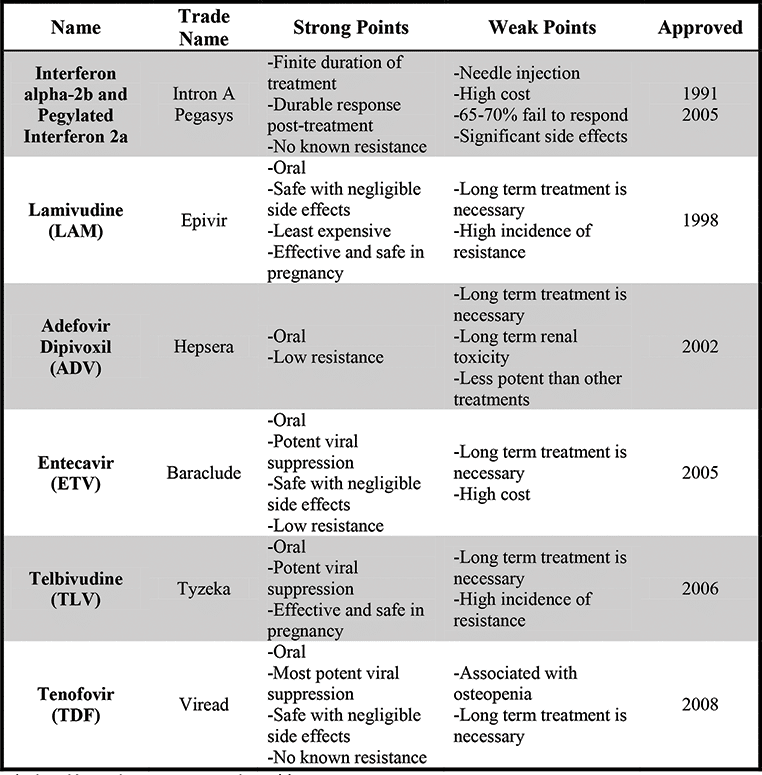
If you have chronic hepatitis B, you might be a candidate for drug therapy. Usually, drug therapy is used only if you have active liver disease. There are seven drugs that are approved by the U.S. Food and Drug Administration to treat hepatitis B. Two are injectable forms of interferon, while the five other antivirals are tablets.
You will need to take these medications every day. They help by slowing the viruss ability to multiply in your system. This helps reduce swelling and liver damage. Youll need to be regularly monitored for early signs of liver damage and liver cancer. Your healthcare provider will want to see you once or twice a year.
Nucleoside Analogues Or Oral Antivirals
Antivirals, or NAs, slow down or stop the hepatitis B virus from reproducing, decreasing the risk of liver damage. Less liver damage occurs when there is less virus present.
People take NAs orally as a pill and experience very few side effects.
First-line treatments, such as Tenofovir disoproxil and entecavir, are potent and effective in suppressing the virus, but they only work for as long as a person takes them. Discontinuing treatment
Also Check: What Is The Hepatitis C Antibody Test
Treatment Of Chronic Hepatitis B Guidelines
Detection of the following relevant indicators at baseline before treatment
major biochemical markers, such as ALT, AST, bilirubin, and albumin major virological and serological markers, such as HBV DNA quantification, HBsAg, HBeAg, and anti-HBe blood routine serum creatinine levels, blood phosphorus levels, and renal tubular function should be tested if required noninvasive tests for liver fibrosis, such as liver stiffness measurement and when ETV and TDF are used in patients with creatinine clearance < 50 mL/min, the doses of both drugs should be adjusted. There is no recommended dose for TAF when it is used in patients with creatinine clearance < 15 mL/min who are not receiving hemodialysis. In other cases, no dose adjustment is required.
Patient compliance
It should be closely monitored, which includes dosage, method of use, missed medication or self-discontinuation, to ensure that patients understand the risks that might result from unwarranted discontinuation and improve their compliance.
Prevention and management of rare adverse events
Monitoring and management of drug resistance
The use of potent antiviral drugs with minimal resistance has resulted in significantly reduced rates of resistance that could arise from long-term treatment of NAs. If HBV DNA levels increased > 2 lg IU/mL from nadir during treatment and the potential of poor compliance has been ruled out, salvage therapy should be initiated promptly, and drug resistance should be tested for.
Who Should Get The Hepatitis B Vaccine
All newborn babies should get vaccinated. You should also get the shot if you:
- Come in contact with infected blood or body fluids of friends or family members
- Use needles to take recreational drugs
- Have sex with more than one person
- Are a health care worker
- Work in a day-care center, school, or jail
Also Check: Drugs Used For Hepatitis C
What Is Involved In A Liver Transplant
A liver transplant is considered necessary when the liver is damaged and cannot function or in some cases of liver cancer. Your liver is very important. It is responsible for many functions related to making sure that your body stays healthy and is able to digest foods.
You may be eligible for a transplant if you have chronic hepatitis B infection or some of the diseases that may result from it, including liver cancer and cirrhosis. You will have to complete testing and be evaluated before being approved for a transplant. It is likely that you will be placed on a waiting list while an appropriate organ is found.
Donated livers come from two types of donors: living and deceased. Because the liver can regenerate, it is possible to use part of a liver for transplant. The remaining sections in both the donor and the receiver will grow into livers of adequate size.
People who get liver transplants must take anti-rejection drugs for the rest of their lives. These drugs make you more susceptible to infection. However, liver transplants have become more successful over time and continue to improve.
Candidates In The General Population
Antiviral treatment is an effective therapeutic strategy for CHB patients that efficiently suppresses HBV replication, decreases inflammatory necrosis in the liver, reduces the incidence of liver cirrhosis and related complications, and reduces the fatality rate associated with hepatocellular carcinoma and other liver diseases. In the 2019 China guidelines , HBV infection is divided into four phases: immune tolerance, immune clearance, immune control, and immune reactivity, and it is different from the 2015 version . Additionally, the 2019 China guidelines eased the restrictions on indications for antiviral therapy, and reducing the demand for HBV-DNA load. Conversely, the HBV-DNA load is considered for the performance of antiviral therapy in the 2018 guidelines updated by the 2018 AASLD guideline and the 2017 EASL guidelines . For the treatment of HBV infection with normal ALT , antiviral therapy is recommended in patients > 30-years-old with a family history of liver cirrhosis or cancer in the 2019 China guidelines. In another case > 30-years-old without a family history of liver cirrhosis or cancer, a hepatic biopsy was recommended. Although we can refer to many guidelines, there are many patients failed to fulfill the criteria for treatment at follow-up and eventually developed liver fibrosis, cirrhosis, and cancer .
Table 1. Comparison between 2015 and 2019 guidelines.
Table 2. Indications for chronic hepatitis B treatment in 2017 and 2018 guidelines.
Don’t Miss: Medicine To Treat Hepatitis C
Hepatitis B Causes And Risk Factors
Itâs caused by the hepatitis B virus, and it can spread from person to person in certain ways. You can spread the hepatitis B virus even if you donât feel sick.
The most common ways to get hepatitis B include:
- Sex. You can get it if you have unprotected sex with someone who has it and your partnerâs blood, saliva, , or vaginal secretions enter your body.
- Sharing needles. The virus spreads easily via needles and syringes contaminated with infected blood.
- Accidental needle sticks.Health care workers and anyone else who comes in contact with human blood can get it this way.
- Mother to child.Pregnant women with hepatitis B can pass it to their babies during childbirth. But thereâs a vaccine to prevent newborns from becoming infected.
Hepatitis B doesnât spread through kissing, food or water, shared utensils, coughing or sneezing, or through touch.
How Do I Get Hepatitis B Treatment
Usually for adults, hepatitis B goes away on its own and you wont need treatment. Your doctor might tell you to rest, eat well, and get plenty of fluids. You may also get medicines to help with any symptoms you might have but be sure to talk with your doctor or nurse before taking anything.
If you have chronic hepatitis, there are medicines you can take to treat it. Your doctor will tell you about your options and help you get whatever treatment you need.
Read Also: Hepatitis C Antigens And Antibodies