Diagnosing Autoimmune Hepatitis In Children
The liver is a large organ in the abdomen that performs many important tasks: It removes toxins from the blood, makes substances that aid in digestion and blood clotting, and stores vitamins and minerals needed throughout the body.
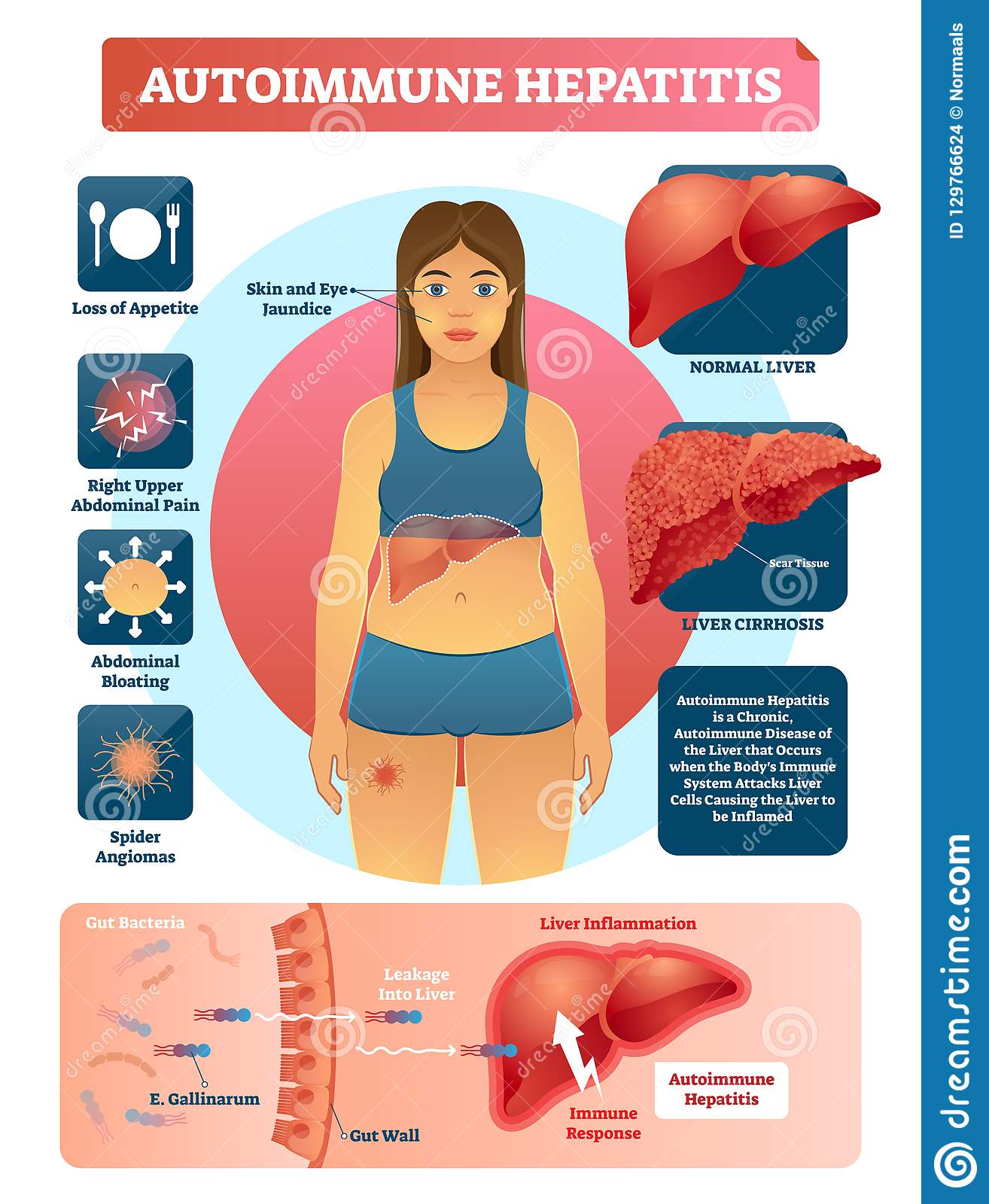
Hepatitis refers to any inflammation of the liver. Autoimmune hepatitis occurs when the immune system, which normally protects the body from infection, attacks healthy cells in the liver, causing chronic inflammation. Without treatment, this inflammation can cause scarring in the liver, known as cirrhosis, and ultimately, liver failure.
Doctors at Hassenfeld Childrens Hospital at NYU Langone have extensive experience in diagnosing and treating autoimmune hepatitis in children.
Signs & Symptoms Of Autoimmune Hepatitis
Most cases of early autoimmune hepatitis have no symptoms and can only be detected by routine blood tests . The symptoms of autoimmune hepatitis differ depending on its severity and may include:
- Itchy skin, dark urine, pale stools, disorientation, abdominal swelling, and leg swelling if the disease gets worse
Can An Autoimmune Hepatitis Diagnosis Be Something Else
Some symptoms and lab findings found in autoimmune hepatitis are also common in other chronic conditions. Your medical team will work to rule out any other possible causes for your symptoms. Some diseases to rule out include other types of hepatitis, certain viral infections, and other liver conditions such as cirrhosis and fatty liver disease.
You May Like: Hepatitis B Surface Antigen Antibody
Don’t Miss: What Kills The Hepatitis C Virus
Less Common Symptoms Of Ms
Less common symptoms may include tremors, hearing loss, difficulties with swallowing, speech problems, seizures, itching, and periods of uncontrollable laughter or crying, says Dr. Croll.
Its also important to note that MS is more common in women than in men.
Women may notice that their symptom severity varies with hormonal changes, pregnancy, and menopause. Men are more likely to be diagnosed with a more progressive form of MS called primary progressive MS, Dr. Croll explains.
Causes And Risk Factors
Hepatitis in children has many different origins or causes. A child may contract hepatitis from exposure to a viral source. The following is a list of some of the viruses associated with hepatitis:
- Hepatitis viruses. Five main types of the hepatitis virus have been identified, including hepatitis A, B, C, D, and E.
- Cytomegalovirus . This virus is a part of the herpes virus family that can be transmitted from person to person.
- Epstein-Barr virus . The virus most commonly associated with infectious mononucleosis.
- Herpes simplex virus . Herpes can involve the face and skin above the waist, or the genitalia.
- Varicella zoster virus . Also known as chickenpox, a complication of VZV is hepatitis, although these very rarely cause hepatitis in children or infants.
- Enteroviruses. A group of viruses commonly seen in children such as coxsackie viruses and echoviruses.
- Rubella. Caused by the Rubivirus, rubella is a mild disease that causes a rash. It can cause problems for the fetus if contracted during pregnancy.
- Adenovirus. A group of viruses that commonly cause colds, tonsillitis, and ear infections in children. They can also cause diarrhea.
- Parvovirus. A virus referred to as fifth disease, which is characterized by a facial rash that is described as having a slapped-cheek appearance.
The following is a list of some of the diseases that may cause acute or chronic hepatitis in children:
Don’t Miss: Can Hepatitis Cause Mental Illness
How Can Autoimmune Hepatitis Be Prevented
There is no commercial testing to delineate which individual would be at risk for acquiring AIH. Immunization with hepatitis A vaccine is encouraged by the American Academy of Pediatrics for all children older than 12 months of age and with three doses of hepatitis B vaccine from birth. This may help prevent the development of AIH in genetically predisposed individuals. More studies are needed to understand the role of viral infection in AIH. Perhaps individuals who have a strong family history of autoimmune disease should be aware of certain medications that can cause AIH-DILI.
Are You Sure Your Patient Has Autoimmune Hepatitis What Are The Typical Findings For This Disease
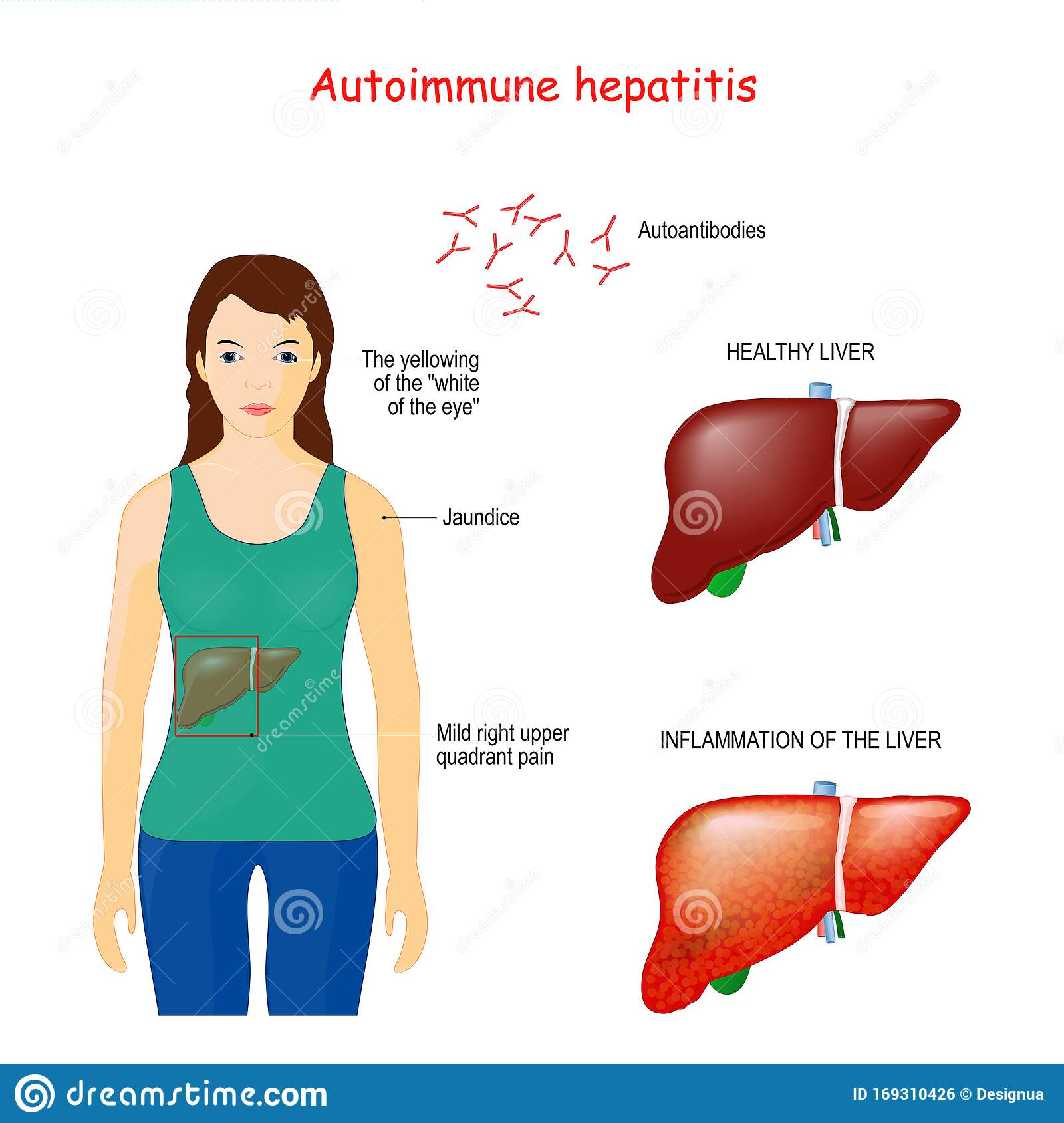
Autoimmune hepatitis often presents with nonspecific symptoms of fatigue, anorexia, and nausea. The next most common symptoms are abdominal pain, jaundice, arthralgia, and epistaxis.
AIH is a chronic progressive inflammatory disease that mainly affects the liver and is characterized by autoimmune injury to hepatocytes, resulting in liver fibrosis and cirrhosis. AIH is described biochemically by an elevation of alanine aminotransferase and aspartate aminotransferase levels, serologically by elevated immunoglobulin G levels and the presence of autoantibodies, and histologically by the presence of interface hepatitis and lymphoplasmacytic infiltrates in the liver in the absence of other known conditions.
Classifications of Autoimmune Hepatitis
Clinical Manifestations of Autoimmune Hepatitis
The majority of patients with AIH present with insidious and nonspecific symptoms. Seventy-five percent of patients with AIH are girls/women. AIH-1 affects all age groups with a bimodal presentation: one peak occurs in children and adolescents and the other in occurs adults older than 40 years of age. AIH-2 predominantly affects children and young adults.
Physicians must have a high index of suspicion for AIH. An early clue to the diagnosis of AIH is female sex, negative serologic test results for the various causes of viral hepatitis, and high serum globulin or IgG.
Interestingly one third of pediatric patients with AIH have cirrhosis at diagnosis, as reported by Gregorio et al.
Don’t Miss: Hepatitis B What Is It
Graft Dysfunction After Liver Transplantation
Autoimmune hepatitis can recur or develop de novo after liver transplantation, and it should be considered in all transplanted patients with graft dysfunction .108113 The frequency of recurrence ranges from 8% to 68%, depending in part on the performance of liver tissue examinations by protocol or by clinical indication.113118 Autoimmune hepatitis recurs in 8% to 12% after 1 year and 36% to 68% after 5 years .113,119122De novo autoimmune hepatitis occurs in 1% to 7% of patients 1 month to 9 years after transplantation for nonautoimmune liver disease.108,120,123125
Diagnostic criteria for recurrent or de novo autoimmune hepatitis after liver transplantation have not been codified.113 Most patients have hypergammaglobulinemia, increased serum levels of IgG, conventional autoantibodies, and interface hepatitis with or without portal plasma cell infiltration.119,126,127 Adults with de novo autoimmune hepatitis may develop antibodies against glutathione-S-transferase T1 .128 Recurrent and de novo autoimmune hepatitis are variably responsive to conventional corticosteroid therapy cirrhosis develops in as many as 60% graft loss is possible and retransplantation is required in 8% to 50%.113
What Are The Adverse Effects Associated With Each Treatment Option
The common adverse effects of prednisone are gastrointestinal disturbances, mood changes, increased appetite, acne, salt retention, osteopenia, frequent infection, and hypertension. Uncommon side effects include diabetes mellitus, pancreatitis, steroid psychosis, and avascular necrosis of the hip joints. Azathioprine is known to cause nausea, vomiting, rash, pancreatitis, bone marrow suppression, liver dysfunction, cholestatic hepatitis, and frequent infection. Individuals with extremely low TPMT enzyme activity or elevated 6-TG metabolites are at risk for bone marrow suppression. An elevation of the 6-MMP metabolite is associated with liver dysfunction. In an individual who has extremely high TPMT enzymes or has low 6-TG metabolites and very high 6-MMP metabolites, hepatotoxicity often occurs. To avoid hepatotoxicity, Al-Shamma et al. used allopurinol, which is a xanthine oxidase inhibitor in an AIH patient who went into remission rapidly. Xanthine oxidase inhibitors promote the metabolism of azathioprine to 6-TU and 6-TG metabolites, therefore resulting in less substrate for the TPMT enzyme to metabolize azathioprine into 6-MMP metabolites, therefore resulting in less hepatotoxicity.
Don’t Miss: Life Expectancy For Hepatitis B
What Complications Might You Expect From The Disease Or Treatment Of The Disease
AIH is a chronic inflammatory disease of the liver. A significant degree of hepatic necrosis can lead to marked fibrosis, even with appropriate treatment. Despite normal serum aminotransferase levels, it is possible that the liver still has low-grade inflammation . Eventually, some patients with this type of inflammation will experience cirrhosis and manifest signs and symptoms of portal hypertension.
It is almost an art to titrate immunosuppressive drugs to achieve an early complete remission. Patient education is essential to the success and safety of the treatment in AIH. Susceptibility to frequent viral and bacterial infections may require discontinuation or a decrease in immunosuppressant drug doses as treatment, with an appropriate antibiotic.
The use of high-dose prednisone and azathioprine at the beginning of therapy requires vigilant monitoring with biochemistry panels. Persistent hyperglycemia or the development of diabetes mellitus from high-dose prednisone should be avoided, as this may lead to severe opportunistic infections such as fungal diseases.
What Is The Treatment For Autoimmune Hepatitis
Treatment is almost always needed. Early treatment can improve symptoms, reduce the risk of complications, and also greatly improve your outlook . Treatment aims to reduce inflammation and suppress the immune system with immunosuppressant medicines:
- Steroid medication is the usual first treatment. Steroids are good at reducing inflammation. A high dose is usually needed at first. The dose is then gradually reduced over a few weeks. The aim is to find the lowest dose needed to control the inflammation. The dose needed varies from person to person. See the separate leaflet called Oral Steroids for more detail.
- Azathioprine is an immunosuppressant medicine that works in a different way to steroids. It is usually used in addition to the steroid. A steroid plus azathioprine tends to work better than either alone. Also, the dose of steroid needed is usually less if you also take azathioprine. This means that any side-effects from steroids may be less severe.
Treatment works well in most cases. Usually, the inflammation settles and symptoms improve within a few months of starting treatment. However, it may take a year or more to get the disease totally under control. Azathioprine is usually taken for at least two years.
For some people a liver transplant may be an option for example:
- In the few people who do not respond to treatment with the medicines mentioned above or
- In people diagnosed in the late stage of the disease with severe scarring of the liver or liver failure.
Don’t Miss: What Is Hepatitis C Contagious
Potential Outcomes Of Immunosuppressant Therapy
The goal of treatment is disease remission. In remission, patients experience the improvement of symptoms, the normalization of abnormal liver chemistries and gamma globulin levels, and the reduction or elimination of inflammatory activity on liver biopsy.
Most patients who embark on a course of immunosuppressant therapy respond well initially. More than 90% of adults started on corticosteroid treatment experience improvements in liver chemistries and gamma globulin levels within 2 weeks.
Remission, if it is to be achieved, typically requires 18-24 months of immunosuppressant therapy. Remission can be achieved in about 65% of patients within 18 months and 80% of patients within 3 years. Once a drug-induced remission is achieved, an attempt should be made to withdraw immunosuppression. However, a sustained remission after total drug withdrawal is seen in 13% of patients at 5 years. Patients who relapse need to restart long-term immunosuppressant therapy in an effort to normalize their biochemical abnormalities and to delay the progression of liver disease. Many such patients are maintained on chronic maintenance therapy with azathioprine.
About 13% of patients experience an incomplete response to treatment, without worsening of their condition. Most incomplete responders need long-term immunosuppression in an attempt to stabilize levels of aspartate transaminase and alanine aminotransferase andby extensionprevent disease progression.
References
Symptoms Of Hepatitis B
Some people who are infected with the hepatitis B virus have mild, flu-like symptoms and some do not become sick at all. Children who are infected are less likely to have an illness or get sick after getting hepatitis B than adults.
In more severe cases, hepatitis B can cause:
- Loss of appetite.
- Pain in the joints.
Normally, these health problems disappear in a few weeks, but even when the person feels much better, they may still be infectious.
Most adults who become infected with the hepatitis B virus recover completely and do not become infected again. A few people become very ill in the time just after infection and need to go to hospital some may even die.
Dont Miss: Hepatitis C Ab Test Results
Recommended Reading: What Is The Treatment For Hepatitis B Virus
Signs And Symptoms Of Autoimmune Hepatitis
Autoimmune hepatitis is a rare, serious condition in which the bodys immune system attacks the liver and causes inflammation. It can lead to cirrhosis and liver failure if it isnt treated. There are two forms of autoimmune hepatitis disease.
Early Hepatitis C Symptoms
Hepatitis C is typically transmitted through exposure to infected blood, which usually occurs through sharing needles. Many people with a new hepatitis C viral infection do not have any symptoms. When symptoms do occur, they can include:
These symptoms usually begin about two to 12 weeks after exposure to the virus.
You May Like: What To Do If I Have Hepatitis B
What Causes This Disease And How Frequent Is It
In general AIH-1 is the most common form. The prevalence is 1/200,000 in the US population however this could have been underreported, since AIH is an insidious disease and some cases could be asymptomatic. The prevalence of AIH-2 is unknown.
Previous hepatitis A virus infection has been proposed as a factor that results in molecular mimicry between the infectious particle and the liver parenchyma in AIH-1. Hepatitis C infection is frequently associated with AIH-2.
Individuals who are susceptible to AIH likely have allelic variants of DRB1 on their human leucocyte antigen region, suggesting a pathogenic role for HLA class II antigen presentation and T-cell activation. HLA DRB1*0301 and DRB1*0401 increase susceptibility for AIH-1 in North American and European populations, and DRB1*0405 and DRB1*0404 play that role in Japanese, Argentinean, and Mexican populations. In South America, individuals with DRB1*1301 likely have frequent exposure to HAV and are predisposed to AIH-1. Possession of HLA DRB1*701 and DRB1*0301 increases susceptibility to AIH-2, with the former carrying a more severe form of AIH.
Complications Of Autoimmune Conditions
Autoimmune diseases can potentially put you at risk for serious complications. These vary by condition, but some of the more common ones include:
- Heart disease: Conditions that cause inflammation, such as lupus and rheumatoid arthritis, can affect the heart.
- Mood disorders: Long-term pain and fatigue, which are symptoms of many autoimmune diseases, are often associated with depression and anxiety.
- Neuropathy: Nerve damage or neuropathy can develop with many autoimmune disorders, including rheumatoid arthritis and Sjögren’s syndrome. This can lead to feeling numb and weak in the arms or legs.
- Deep vein thrombosis: Ulcerative colitis and Crohn’s disease lead to an increased risk of developing blood clots. These clots may travel to the lungs and cause a blockage, known as a pulmonary embolism.
- Organ damage: Autoimmune diseases that cause harm to specific organs can lead to significant damage if not properly treated. For example, type 1 diabetes can cause kidney failure.
Talk to your healthcare provider about what you can do to minimize the risk of complications that are associated with your condition.
Don’t Miss: How To Check For Hepatitis C
What You Can Do
- Be aware of any pre-appointment restrictions. At the time you make the appointment, be sure to ask if there’s anything you need to do in advance, such as restrict your diet.
- Write down any symptoms you’re experiencing, including any that may seem unrelated to the reason for which you scheduled the appointment.
- Write down key personal information, including any major stresses or recent life changes.
- Make a list of all medications, vitamins or supplements that you’re taking.
- Take a family member or friend along to help you remember everything that was discussed.
- Write down questions to ask your doctor.
For autoimmune hepatitis, some basic questions to ask your doctor include:
What Is Viral Hepatitis
Hepatitis means inflammation of the liver. The liver is a vital organ that processes nutrients, filters the blood, and fights infections. When the liver is inflamed or damaged, its function can be affected. Heavy alcohol use, toxins, some medications, and certain medical conditions can cause hepatitis. However, hepatitis is often caused by a virus. In the United States, the most common types of viral hepatitis are hepatitis A, hepatitis B, and hepatitis C.
Read Also: What Does Hepatitis Feel Like
How Is It Spread
Hepatitis A is spread when a person ingests fecal mattereven in microscopic amountsfrom contact with objects, food, or drinks contaminated by feces or stool from an infected person.
- Birth to an infected mother
- Sex with an infected person
- Sharing equipment that has been contaminated with blood from an infected person, such as needles, syringes, and even medical equipment, such as glucose monitors
- Sharing personal items such as toothbrushes or razors
- Poor infection control has resulted in outbreaks in health care facilities
Hepatitis C is spread when blood from a person infected with the Hepatitis C virus even in microscopic amounts enters the body of someone who is not infected. The hepatitis C virus can also be transmitted from:
- Sharing equipment that has been contaminated with blood from an infected person, such as needles and syringes
- Receiving a blood transfusion or organ transplant before 1992
- Poor infection control has resulted in outbreaks in health care facilities
- Birth to an infected mother
Recommended Reading: Can You Give Plasma If You Have Hepatitis C
What Is The Evidence

The evidence for treatment presented above is expert opinion only. There are no randomized controlled treatment trials in children with AIH.
McFarlane, IG. Definition and classification of autoimmune hepatitis. Semin Liver Dis. vol. 22. 2002. pp. 317-24.
Krawitt, EL. Autoimmune hepatitis. N Engl J Med. vol. 354. 2006. pp. 54-66.
Mieli-Vergani, G, Vergani, D. Autoimmune hepatitis. Nat Rev Gastroenterol Hepatol. vol. 8. 2011. pp. 320-9.
Ferrari, R, Pappas, G, Agostinelli, D. Type 1 autoimmune hepatitis: patterns of clinical presentation and differential diagnosis of the ‘acute’ type. QJM. vol. 97. 2004. pp. 407-12.
Al-Chalabi, T, Underhill, JA, Portmann, BC. Impact of gender on the long-term outcome and survival of patietns with autoimmune hepatitis. J Hepatol. vol. 48. 2008. pp. 140-7.
Czaja, AJ, Davis, GL, Ludwig, J. Autoimmune features as determinants of prognosis in steroid-treated chronic active hepatitis of uncertain etiology. Gastroenterology. vol. 85. 1983. pp. 713-7.
Gregorio, GV, Mieli-Vergani, G. Autoimmune liver disease in childhood. Indian J Gastroenterol. vol. 16. 1997. pp. 60-3.
Castiella, A, Lucena, MI, Zapata, EM. Drug-induced autoimmune-like hepatitis: a diagnostic challenge. Dig Dis Sci. vol. 56. 2011. pp. 2501-3.
Mieli-Vergani, G, Heller, S, Jara, P. Autoimmune hepatitis. J Pediatr Gastroenterol Nutr. vol. 49. 2009. pp. 158-64.
Donaldson, PT. Genetics in autoimmune hepatitis. Semin Liver Dis. vol. 22. 2002. pp. 353-64.
Also Check: Hepatitis A And B Shots