Accepting Hepatitis C Risk
This group accepted the risks that accompanied their behaviour as they viewed behaviour change as requiring considerable effort, whereas they perceived medical treatment as an easier option. Thus, they accepted and even expected multiple rounds of treatment or possibly living with a chronic hepatitis C infection. However, they were concerned about disclosure and the possibility of sexual rejection.
“This group accepted and even expected multiple rounds of treatment or possibly living with a chronic hepatitis C infection.”
Its hard to change much. Because in the moment you dont want to talk about it. Because thats when you want to party, have sex, you want to enjoy and you dont want to say, Hey stop! Hepatitis C! Then everything would be over.
They had lived with hepatitis C for a similar time to the second group but went on an intensive search for information to better understand the infection and prevent re-infection. Two had been previously treated with older interferon-based therapy. While some men in this group had opted for some risk-reduction strategies, there was frustration at not knowing exactly how they became infected or re-infected. This occasionally led to abandonment of risk-reduction strategies.
One couple spoke of how much easier it was having a partner with both infections:
anxiety
Can Hcv Infection Be Prevented
The best protection against HCV is to never inject drugs. If you do inject drugs, always use new, sterile needles, and do not reuse or share needles, syringes, or other injection drug equipment.
People, including people with HIV, can also take the following steps to reduce their risk of HCV infection:
- Do not share toothbrushes, razors, or other personal items that may come in contact with another personâs blood.
- If you get a tattoo or body piercing, make sure the instruments used are sterile.
- Use condoms during sex. The risk of HCV infection through sexual contact is low, but the risk increases in people with HIV. Condoms also reduce the risk of HIV transmission and infection with other sexually transmitted diseases, such as gonorrhea and syphilis.
The Link Between Hepatitis C And Hiv
Both hepatitis C and HIV are transmitted the same way, says Dr. Sherman: through unprotected sexual contact with an infected person or by sharing injection drug needles with someone who is infected.
Engaging in high-risk behaviors , such as using injection drugs or not using a condom during sex, can increase your risk of contracting one or both viruses. Infection can happen either from the same person or different people, at the same time or different times.
Both hepatitis C and HIV are transmitted by blood exposure through needle sharing, says Sherman. However, hepatitis C is more transmissible, so many patients get that first, followed later by HIV. Occasionally, both viruses are transmitted at the same time.
The risk of being infected with HIV and hepatitis Cis higher among Black Americans. According to the CDC and the U.S. Department of Health and Human Services, Black Americans account for about 13 percent of the population but 42 percent of new HIV diagnoses and 25 percent of chronic hepatitis C diagnoses. Black Americans have also historically been almost twice as likely to die of hepatitis C compared with white Americans.
Socioeconomic factors due to poverty limited access to healthcare, housing, and education increase the risk for infection, according to the CDC. Stigma, fear, and discrimination may also prevent Black Americans from seeking or having access to prevention and care services, the CDC adds.
You May Like: How To Test For Hepatitis
How Are Hepatitis B And Hepatitis C Spread From Person To Person
Like HIV, the hepatitis B and hepatitis C viruses spread:
- From mother to child: Pregnant women can pass these infections to their infants. HIV-HCV coinfection increases the risk of passing on hepatitis C to the baby.
- Sexually: Both viruses can also be transmitted sexually, but HBV is much more likely than HCV to be transmitted sexually. Sexual transmission of HCV is most likely to happen among gay and bisexual men who are living with HIV.
Prevention Is The Best Medicine

Even though hepatitis C rarely spreads within a household, if you or a family member have the disease, it’s wise to take precautions to prevent its spread especially if anyone in your home is immune compromised, or has cuts or open sores that increase the risk of infection.
In general, use these common sense preventive tips:
- Unless you are in a long-term, monogamous relationship, practice safe sex.
- Clean up spilled or dried blood with a bleach-based cleaning solution and wear rubber gloves.
- Do not share razors.
- Do not share toothbrushes. “Though hepatitis C is not transmitted through saliva, there might be blood on the toothbrush,” Reau says.
Note that hepatitis C is not transmitted by sharing eating utensils, hugging, kissing, coughing or sneezing.
Don’t Miss: New Treatment For Hepatitis B
How Do People Become Infected With Hiv
HIV is in the blood, semen, vaginal fluid and breast milk of an infected person. It can be spread by exposure to these body fluids by:
- unprotected anal or vaginal sex without a condom
- sharing drug injecting equipment
- tattooing, piercing and other procedures with unsterile needles or equipment
- transmission from mother to baby during pregnancy, childbirth or breastfeeding
- oral sex, although this is rare
- sharps injuries
It is important to remember that HIV is not spread through activities such as kissing, sharing cups and cutlery, normal social contact, toilet seats or mosquitoes.
You are at higher risk of HIV infection if:
- you are a man, a transgender woman or a person who identifies as gender diverse who has sex with men
- you have sex or share needles with someone else at risk of HIV
- you share sex toys
- you have sex with people from countries with a high rate of HIV infection
- you inject drugs
- you have had tattoos or other piercings overseas using unsterile equipment
- you have a sexually transmitted infection . People can be infected with several different STIs at the same time. Having an STI can make it easier to become infected with HIV and pass it on to sexual partners
- you have had a blood transfusion in a country where the blood supply is not safe
Some people are at a higher risk of HIV infection because they are exposed to more people with HIV infection and/or engage in more high-risk behaviour. These include:
How Is The Health Of Your Liver Monitored
Everyone living with HIV should have regular tests to monitor the health of their liver as part of the routine check-ups carried out by their HIV clinic. These tests are especially important if you have hepatitis C.
These include liver function tests that monitor levels of liver enzymes. Ultrasounds and scans are also important monitoring tools which may be used if more information is needed.
Sometimes its necessary to have a liver biopsy. This involves the removal of a small amount of the liver, under a local anaesthetic, for further tests on the health of your liver.
Don’t Miss: Is There Now A Cure For Hepatitis C
Resources For Drug Interaction
Most persons with HIV infection are taking multidrug antiretroviral therapy, which may pose a problem with drug interactions when initiating HCV treatment. For resources on drug interactions that may occur with HIV antiretroviral medications and HCV treatment medications, access the following sites:
- AASLD-IDSA HCV Guidance: Patients with HIV/HCV Coinfection
Sharing Toothbrushes Scissors And Razors
There’s a potential risk that hepatitis C may be passed on through sharing items such as toothbrushes, razors and scissors, as they can become contaminated with infected blood.
Equipment used by hairdressers, such as scissors and clippers, can pose a risk if it has been contaminated with infected blood and not sterilised or cleaned between customers. However, most salons operate to high standards, so this risk is low.
Read Also: Natural Treatment For Hepatitis C
A Rise In Injection Drug Use Is Fueling A Spike In Hepatitis C Among Young Opioid And Heroin Users
An Indiana nurse holds one of the syringes provided to intravenous drug users taking part in Fayette Countys state-approved needle exchange program. Hepatitis C infections have nearly tripled since 2010 an increase mainly due to the heroin epidemic.
In an unrelenting opioid epidemic, hepatitis C is infecting tens of thousands of mostly young, white injection drug users, with the highest prevalence in the same Appalachian, Midwestern and New England states that are seeing the steepest overdose death rates.
Like the opioid epidemic that is driving it, the rate of new hepatitis C cases has spiked in the last five years. After declining for two decades, new hepatitis C cases shot to an estimated 34,000 in 2015, nearly triple the number in 2010, according to a recent report from the U.S. Centers for Disease Control and Prevention .
With better screening for the bloodborne disease and more treatment using costly but highly effective new drugs, hepatitis C could be eradicated, according to a new study from the National Academies of Sciences, Engineering, and Medicine.
We have two public health problems that are related its called a syndemic and we cant address one without addressing the other, said James Galbraith, an emergency room physician at the University of Alabama at Birmingham Hospital.
A Quiet Disease
More Testing
Hepatitis C primarily affects injection drug users and members of the baby boomer generation born between 1945 and 1965.
What Is Hepatitis C
Hepatitis C is a liver infection caused by the hepatitis C virus . The abbreviation HCV can stand for either the virus or the infection it causes.
HCV can be either a short-term or a long-term illness:
- Acute HCV occurs within 6 months after exposure. In most people, acute HCV becomes chronic HCV.
- Chronic HCV can last a lifetime. Without treatment, chronic HCV can cause liver cancer or severe liver damage that can lead to liver failure.
- HCV is a contagious infection that can spread from person to person.
Read Also: Is Hepatitis C An Autoimmune Disease
Risks Of Hepatitis C And Hiv Coinfection
The CDC reports that HIV coinfection can accelerate the course of hepatitis C, including the rapid progression of chronic liver disease from hepatitis C to cirrhosis, a form of permanent liver damage. This is particularly true in people with advanced immunodeficiency .
In addition, coinfected individuals with cirrhosis progress more rapidly to end-stage liver disease and hepatocellular carcinoma than those with hepatitis C alone. Both of these liver conditions can be life threatening. In fact, according to the CDC, liver disease much of which is caused by hepatitis B or hepatitis C is a leading non-AIDS cause of death in people with HIV.
Hepatitis C has also been associated with an increased risk for conditions such as vasculitis , kidney disease, and the skin condition porphyria cutanea tarda.
Untreated, patients with HIV and hepatitis C coinfection have a worse prognosis in terms of liver disease progression and outcomes, Sherman says.
Hepatitis C Treatment Programmes
An important first step to providing treatment for people with hepatitis C and HIV co-infection is to diagnose infections. HIV services should routinely screen all patients for hepatitis C.
However, guidelines recommending screening are often poorly implemented, especially in low and middle-income countries. Hepatitis C testing may not be systematically provided to groups which have elevated rates of hepatitis C, such as people who inject drugs, prisoners, sex workers, and men who have sex with men.43
Recommended Reading: What Kind Of Disease Is Hepatitis C
Managing Hepatitis C And Hiv
Having both hepatitis C and HIV, called a coinfection, can increase your risk for liver damage if not properly diagnosed and managed.
A diagnosis of hepatitis C alone can be daunting, but people who have the virus are also at increased risk for HIV and vice versa.
According to the Centers for Disease Control and Prevention , 21 percent of HIV-positive people across the country have also tested positive for a past or current hepatitis C infection, although the danger varies greatly depending on your personal risk factors. If you have both conditions, that alone places you at increased risk for liver damage compared with those who have hepatitis C only.
Coinfection with hepatitis C and HIV usually represents an intersection of risk factors for each virus, says Kenneth E. Sherman, MD, PhD, a hepatologist who is the director of the division of digestive diseases and Gould Professor of Medicine at the University of Cincinnati College of Medicine.
How Can Infection With Hiv Be Prevented
There is no vaccine to prevent HIV. Development of one is proving to be very difficult, as the HIV virus is constantly mutating and changing. Therefore, the main way to prevent infection by HIV is to avoid activities that put you at risk, such as sharing needles and having sex without a condom. See the separate leaflet called Safer Sex for more information.
Some cases of HIV can be prevented in other ways – for example:
You May Like: How Is Hepatitis B And C Transmitted
Hiv In The Gay And Bisexual Population
In the now historic document, which recently reached its 30th anniversary, the CDC reported five cases of Pneumocystis carinii pneumonia in young gay men who otherwise should have been healthy. I first became aware of this phenomenon as I sat on the beach reading The New York Times the summer before my freshman year at Columbia University. With bewilderment and fear, I read Robert Altmans account of doctors in New York and California have diagnosed among homosexual men 41 cases of a rare and often rapidly fatal form of cancer. In the following years, I witnessed the eruption of the disease, which in its early years was given the name GRID because of its omnipresence in the gay population .
Hiv Vs Aids: Whats The Difference
Overview
It can be easy to confuse HIV and AIDS. They are different diagnoses, but they do go hand-in-hand: HIV is a virus that can lead to a condition called AIDS, also known as stage 3 HIV.
At one time, a diagnosis of HIV or AIDS was considered a death sentence. Thanks to research and the development of new treatments, people with HIV at any stage today are living long, productive lives. An HIV-positive person who adheres to regular antiretroviral treatment can expect to live a near-normal life span.
Don’t Miss: Can Hepatitis C Be Treated
Awareness Prevention And Early Diagnosis Are Essential
There’s a good reason why hepatitis C is known as a “silent killer.”
According to the U.S. Centers for Disease Control and Prevention, an estimated 3.2 million Americans live with chronic hepatitis C infection, which is transmitted through infected bodily fluids like blood and semen, and causes inflammation of the liver. Yet up to 75% of people who have hepatitis C aren’t aware they have it.
Most of those living with the virus experience only mild symptoms or don’t have any symptoms at all until they develop serious liver damage or another life-threatening liver disease. Unfortunately, that means they aren’t getting diagnosed and treatment is delayed until the later stages when irreversible liver damage has occurred.
Here, hepatologistNancy Reau, MD, associate director of the Solid Organ Transplant Program at Rush University Medical Center, explains who is at risk for hepatitis C and offers advice to help you protect yourself.
Diagnosing Hepatitis C In People Living With Hiv
Everyone with HIV should be tested to see if they also have hepatitis C. A blood test for antibodies to hepatitis C is used to see whether you have been exposed to the virus. You might be given a PCR test to confirm infection.
In people living with HIV, the diagnosis of hepatitis C can be more difficult, as the infection may not show up on their antibody tests.
If you think you may be at risk of hepatitis C infection, you should have regular tests to see if you have been infected with the virus.
Don’t Miss: What Is Hepatitis C And How Do You Get It
How Do You Get Hiv
HIV is carried in semen , vaginal fluids, anal mucus, blood, and breast milk. The virus gets in your body through cuts or sores in your skin, and through mucous membranes . You can get HIV from:
-
having vaginal or anal sex
-
sharing needles or syringes for shooting drugs, piercings, tattoos, etc.
-
getting stuck with a needle that has HIV-infected blood on it
-
getting HIV-infected blood, semen , or vaginal fluids into open cuts or sores on your body
HIV is usually spread through having unprotected sex. Using condoms and/or dental dams every time you have sex and not sharing needles can help protect you and your partners from HIV. If you do have HIV, treatment can lower or even stop the chances of spreading the virus to other people during sex. If you dont have HIV, theres also a daily medicine called PrEP that can protect you from HIV.
HIV can also be passed to babies during pregnancy, birth, or breastfeeding. A pregnant woman with HIV can take medicine to greatly reduce the chance that her baby will get HIV.
HIV isnt spread through saliva , so you CANT get HIV from kissing, sharing food or drinks, or using the same fork or spoon. HIV is also not spread through hugging, holding hands, coughing, or sneezing. And you cant get HIV from a toilet seat.
Tests To Diagnose Hepatitis C
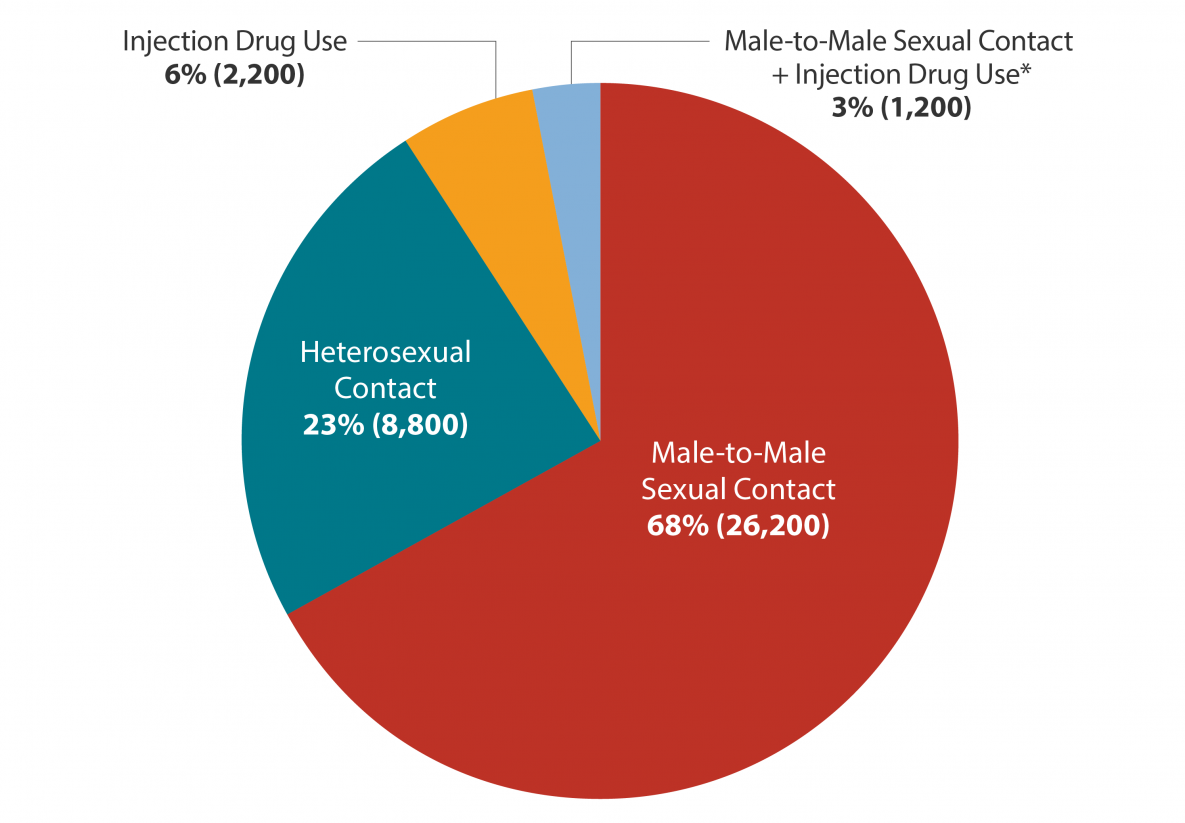
How is Hepatitis C diagnosed?
There are two main blood tests typically used to diagnose Hepatitis C. First, youll have a screening test that shows if youve ever had Hepatitis C at some point in your life. If this test is positive, youll have a second test to see if you have Hepatitis C now. These blood tests are described below:
Hepatitis C antibody test
This is the screening test used by doctors to show whether or not you have ever been exposed to Hepatitis C at some time in your life, by detecting antibodies in your blood. Antibodies are substances your body makes to fight off all kinds of infections. If you were ever infected with Hepatitis C, your body would have made antibodies to fight the virus.
If the test result is:
- Negative, it means you have not been exposed to Hepatitis C and further testing is usually not needed.
- Positive, you have had Hepatitis C at some point. However, it does not tell you whether you have it now. Youll need to see your doctor for another test the Hepatitis C RNA test to determine if the virus is still active and present in your blood.
Hepatitis C RNA Qualitative Test
This test will determine whether or not you are currently infected with Hepatitis C. It is often called the PCR test because of the process used . It looks for the genetic material of the Hepatitis C virus in your blood.
If the test result is:
Hepatitis C RNA Quantitative Test
You May Like: Does The Hpv Vaccine Protect Against Hepatitis B