What Occupations Have Increased Risk Of Hepatitis B
In general, occupational groups with increased risk include:
- Health-care workers repeatedly exposed to blood or blood products or those who are at risk of needlestick injury.
- Pathologists, laboratory personnel, or embalmers.
- Dentists, dental assistants, and dental hygienists.
- Certain staff members of institutions for the developmentally handicapped.
- Staff of institutions where workers may be exposed to aggressive, biting residents.
Travellers to regions with intermediate or high rates of endemic HBV infection may also consider being vaccinated.
Blood Transfusion/receipt Of Blood Products
Early case-control studies of patients with newly acquired, symptomatic non-A, non-B hepatitis found a significant association between disease acquisition and a history six months prior to illness of blood transfusions, injection drug use, health care employment with frequent exposure to blood, personal contact with others who had hepatitis, multiple sexual partners or low socioeconomic status. Today, HCV is rarely transmitted by blood transfusion or transplantation of organs due to thorough screening of the blood supply for the presence of the virus and inactivation procedures that destroy bloodborne viruses. In the last several years, blood banks have instituted techniques that utilize nucleic acid amplification of the hepatitis C virus, which will detect the presence of virus even in newly-infected patients who are still hepatitis C antibody-negative. These techniques are estimated to have prevented 56 transfusion-associated HCV infections per year in the U.S. since 1999, and have lowered the current risk of acquiring HCV via transfused blood products to 1 in 2 million.
How Is Hepatitis B Transmitted
Hepatitis B is spread in several distinct ways: sexual contact sharing needles, syringes, or other drug-injection equipment or from mother-to-child at birth.
In the United States, in 2018, injection drug use was the most common risk factor reported among people with an acute HBV infection, followed by having multiple sex partners. Less commonly reported risk factors included accidental needle sticks, surgery, transfusions, and household contact with a person with HBV infection. In the United States, healthcare-related transmission of HBV is rare.
Mother-to-child transmission of HBV is especially concerning, because it is preventable. An estimated 25,000 infants are born to mothers diagnosed with HBV each year in the United States, and approximately 1,000 mothers transmit HBV to their infants. Without appropriate medical care and vaccinations, 90% of HBV-infected newborns will develop chronic infection, remaining infected throughout their lives. Up to 25% of people infected at birth will die prematurely of HBV-related causes. For this reason, the standard of care for pregnant women includes an HBV test during each pregnancy so that the appropriate steps can be taken to prevent HBV-positive mothers from transmitting the disease to her infant.
Also Check: What Is Hepatitis C From
Alcoholic Or Toxic Hepatitis
As the name suggests, alcoholic hepatitis is caused by excessive consumption of alcohol. One of the primary jobs of the liver is to filter toxins and waste from your body, and one of those substances it filters and breaks down is alcohol. If someone drinks more alcohol than their liver can process, they could develop alcoholic hepatitis, which can eventually lead to liver failure. Although the development of alcoholic hepatitis usually occurs over the course of years of over-drinking, it is possible to develop a case of acute alcoholic hepatitis.
Similarly, toxic hepatitis is caused by exposure to chemicals or drugs that overwhelms the liver. A person who is frequently exposed to toxic chemicals due to their line of work either by ingesting, breathing, or coming into direct contact with chemicals may be at greater risk of developing toxic hepatitis.
Toxic hepatitis can also be an extreme side effect of some prescription or over-the-counter medications. For this reason, its important to stick to the recommended or prescribed doses for any medications and to communicate any alarming symptoms like nausea, vomiting, jaundice, pain, or fever with your primary care physician right away.
No Identifiable Source Of Infection
According to the Centers for Disease Control and Prevention, injection drug use accounts for approximately 60% of all HCV infections in the United States, while other known exposures account for 20-30%. Approximately 10% of patients in most epidemiological studies, however, have no identifiable source of infection. HCV exposure in these patients may be from a number of uncommon modes of transmission, including vertical transmission, and parenteral transmission from medical or dental procedures prior to the availability of HCV testing. There are no conclusive data to show that persons with a history of exposures such as intranasal cocaine use, tattooing or body piercing are at an increased risk for HCV infection based on these exposures solely. It is believed, however, that these are potential modes of HCV acquisition in the absence of adequate sterilization techniques.
Don’t Miss: How Is Hepatitis C Spread
Hiv And Hepatitis B And Hepatitis C Coinfection
Hepatitis B and hepatitis C are liver infections caused by a virus. Because these infections can be spread in the same ways as HIV, people with HIV in the United States are often also affected by chronic viral hepatitis.
Viral hepatitis progresses faster and causes more liver-related health problems among people with HIV than among those who do not have HIV. Liver disease, much of which is related to HBV or HCV, is a major cause of non-AIDS-related deaths among people with HIV.
Given the risks of hepatitis B or hepatitis C coinfection to the health of people living with HIV, it is important to understand these risks, take steps to prevent infection, know your status, and, if necessary, get medical care from someone who is experienced in treating people who are coinfected with HIV and HBV, or HIV and HCV.
Is Hepatitis B Contagious
The disease, hepatitis B, is contagious. HBV, the viral cause of hepatitis B, is transmitted person-to-person by
- blood,
- semen, or
- any other body fluid from the infected person.
Moreover, hepatitis B can be transferred through sexual contact, sharing needles, or from mother to baby at the time of birth.
Also Check: What Happens When You Get Hepatitis C
Treatment: Chronic Hepatitis C
The latest drug to be approved by the FDA is glecaprevir and pibrentasvir . This medication offers a shorter treatment cycle of 8 weeks for adult patients with all types of HCV who donât have cirrhosis and who have not been previously treated. The length of treatment is longer for those who are in a different disease stage. The prescribed dosage for this medicine is 3 tablets daily.
There are several other combination drugs available, as well as some single drugs that may be used in combination. Your doctor will choose the right one for you depending on the type of hepatitis C you have, how well your liver is functioning and any other medical problems you may have. Also be sure to discuss your insurance coverage since these medications are expensive.
Hbv Serotypes And Genotypes
Based on some of the antigenic determinants of HBsAg, nine serological types -referred to as subtypesadw2, adw4,adrq+, adrq, ayw1,ayw2, ayw3, ayw4 andayr – have been identified . Ten genotypes of HBV have been identified, and thesecorrespond to specific geographic distributions . Genotype A is more frequently found in North America,northwestern Europe, India, and Africa. Genotypes B and C are endemic to Asia,and genotype D predominates in eastern Europe and the Mediterranean . Type E is found in western Africa typeF, in South America and type G, in France, Germany, Central America, Mexico,and the United States. Type H is prevalent in Central America type I, in Vietnam and type J, in Japan .
HIV-seropositive MSM populations predominantly coinfected with HBV genotype Ahave been reported in European countries and Japan ,,. The prevalence of HBV genotype A issignificantly higher in the MSM population than in the rest of the population. In addition, Araujo etal. speculated in their review that HBV subgenotypes A2 and C arelikely to predominate in populations at high risk of infection via sexualtransmission . Additionally, HBVgenotype A develops into a persistent infection more often than genotype C ,.
Don’t Miss: Treatment To Cure Hepatitis C
How To Prevent Transmission
Between 2% and 6% of adults infected with hepatitis B virus will develop chronic hepatitis B. Chronic hepatitis B can lead to liver failure and liver cancer, so protecting yourself is important.
The hepatitis B vaccine is safe for almost everyone and about 95% effective for providing long-term protection against hepatitis B infection.
While anyone can benefit from the vaccine, people who are at a greater risk of being exposed to the virus because of their work, lifestyle or medical history are strongly encouraged to be immunized. In many countries, babies born to infected mothers get vaccinated at birth. All babies born in the United States are routinely vaccinated.
Hepatitis B immune globulin , is another way to prevent hepatitis B infection in babies born to infected mothers or after exposure to the virus. This uses concentrated antibodies to provide immediate protection. According to the Centers for Disease Control and Prevention, it is given as a shot and can provide short-term protection against hepatitis B.
Because the hepatitis B vaccine does not protect against HIV, hepatitis C or other diseases spread through sex and contact with blood, it’s still important to keep using basic protective strategies. Practicing safer sex and not sharing needles are recommended even if you’re immune to hepatitis B.
Is Hepatitis A Sexually Transmitted Infection
Viral hepatitis can be transmitted through blood and other bodily fluids, including sexual fluids. Each viral strain has a different risk of being transmitted through sex.
Hepatitis B is most commonly linked with sexual transmission. The hepatitis B virus is present in semen and bodily fluids shared between two partners during unprotected sex.
You can also contract hepatitis A through sexual contact, though it is far more common to get hepatitis A by consuming food or water that has been contaminated by the feces of people infected with hepatitis A.
The hepatitis C virus is present in blood. While it can be transmitted sexually, the rate of sexual transmission is low. Hepatitis C is more likely to be transmitted through the use of shared needles or razors.
To protect yourself from sexual transmission of hepatitis, you can get vaccinated against hepatitis A and B . Using condoms or other barrier methods during vaginal, oral, or anal sex can also reduce your risk of contracting viral hepatitis as well as other sexually transmitted diseases and infections.
Also Check: What Is The Definition Of Hepatitis B
How Are Hepatitis B And C Diagnosed
Hepatitis B is diagnosed by a series of blood tests. The test may show an ongoing infection or antibodies that indicate that the patient is protected against hepatitis B. In patients who have a positive screening test that suggests the possibility of ongoing infection, further testing is done to determine the levels of the virus in the bloodstream.
Hepatitis C is diagnosed via a blood test called a Hepatitis C Antibody Test. A positive result means that hepatitis C antibodies are present in the blood. But a positive antibody test doesnt necessarily mean a person has hepatitis C. A further blood test is needed to confirm the diagnosis. This second blood test quantifies the amount of the virus or the viral load in the liver and the bloodstream.
Hepatitis B: What Happens
Many adults who get hepatitis B have mild symptoms for a short time and then get better on their own. But some people are not able to clear the virus from the body, which causes a long-term infection. Nearly 90% of infants who get the virus will carry it for life. Over time, hepatitis B can lead to serious problems, such as liver damage, liver failure, and liver cancer.
Also Check: Can You Cure Hepatitis A
Hiv And Hbv Coinfection
About 2% of people with HIV in the United States are coinfected with HBV both infections have similar routes of transmission. People with HIV are at greater risk for complications and death from HBV infection. All people with HIV are recommended to be tested for HBV, and if susceptible, are further recommended to receive the hepatitis B vaccination or, if chronically infected, evaluated for treatment to prevent liver disease and liver cancer. For more information about HIV and HBV coinfection, visit HIV.govâs pages about hepatitis B and HIV coinfection.
What Is The Outlook
Most people with hepatitis A recover without any complications. Once youve had hepatitis A, you cant get it again. Antibodies to the virus will protect you for life.
Some people may be at an increased risk for serious illness from hepatitis A. These include:
- older adults
acute hepatitis B infections in the United States in 2018.
Don’t Miss: Hepatitis B How Do You Catch It
How Do You Get Hepatitis B
Hepatitis B is really contagious. Its transmitted through contact with semen , vaginal fluids, and blood. You can get it from:
-
having vaginal, anal, or oral sex
-
sharing toothbrushes and razors
-
sharing needles for shooting drugs, piercings, tattoos, etc.
-
getting stuck with a needle that has the Hep B virus on it.
Hepatitis B can also be passed to babies during birth if their mother has it.
Hepatitis B isnt spread through saliva , so you CANT get hepatitis B from sharing food or drinks or using the same fork or spoon. Hepatitis B is also not spread through kissing, hugging, holding hands, coughing, sneezing, or breastfeeding.
Treatment Options For Hepatitis B
Acute hepatitis B usually doesnt require treatment. Most people will overcome an acute infection on their own. However, rest and hydration will help you recover.
Antiviral medications are used to treat chronic hepatitis B. These help you fight the virus. They may also reduce the risk of future liver complications.
You may need a liver transplant if hepatitis B has severely damaged your liver. A liver transplant means a surgeon will remove your liver and replace it with a donor liver. Most donor livers come from deceased donors.
Also Check: Hepatitis C Transmission Routes Cdc
How Is It Treated
Hepatitis A is treated using supportive methods. These can include things like rest, fluids, and healthy foods. Medications can also help to ease some symptoms like fever, aches, and pains.
Theres a vaccine available to protect against infection with HAV. This is typically recommended for children as well as for people at an increased risk for contracting the virus.
Also, receiving a single dose of the hepatitis A vaccine may prevent you from becoming ill if youve been exposed to HAV. For it to be effective, the vaccine needs to be given of exposure.
How Is Hepatitis Diagnosed
Chronic hepatitis can quietly attack the liver for years without causing any symptoms. Unless the infection is diagnosed, monitored, and treated, many of these people will eventually have serious liver damage. Fortunately, blood tests can determine whether you have viral hepatitis, and if so, which kind.
You May Like: Is There A Cure For Hepatitis B Virus
Hepatitis C: What Happens
About 25% of people who get hepatitis C defeat the virus after a short-term infection. The rest will carry the virus in their body for the long term. Chronic hepatitis C can cause very serious complications, including liver failure and liver cancer. There are effective treatments for the virus, though.
Who Should Be Tested For Hepatitis
Testing is important for anyone with the risk factors we’ve mentioned, particularly injected drug users and people who have had multiple sex partners. Health advocates are also urging people of Asian heritage to get tested. Stanford University’s Asian Liver Center estimates that 1 in 10 Asians living in the U.S. has chronic hepatitis B. Many of them have probably had the virus since birth.
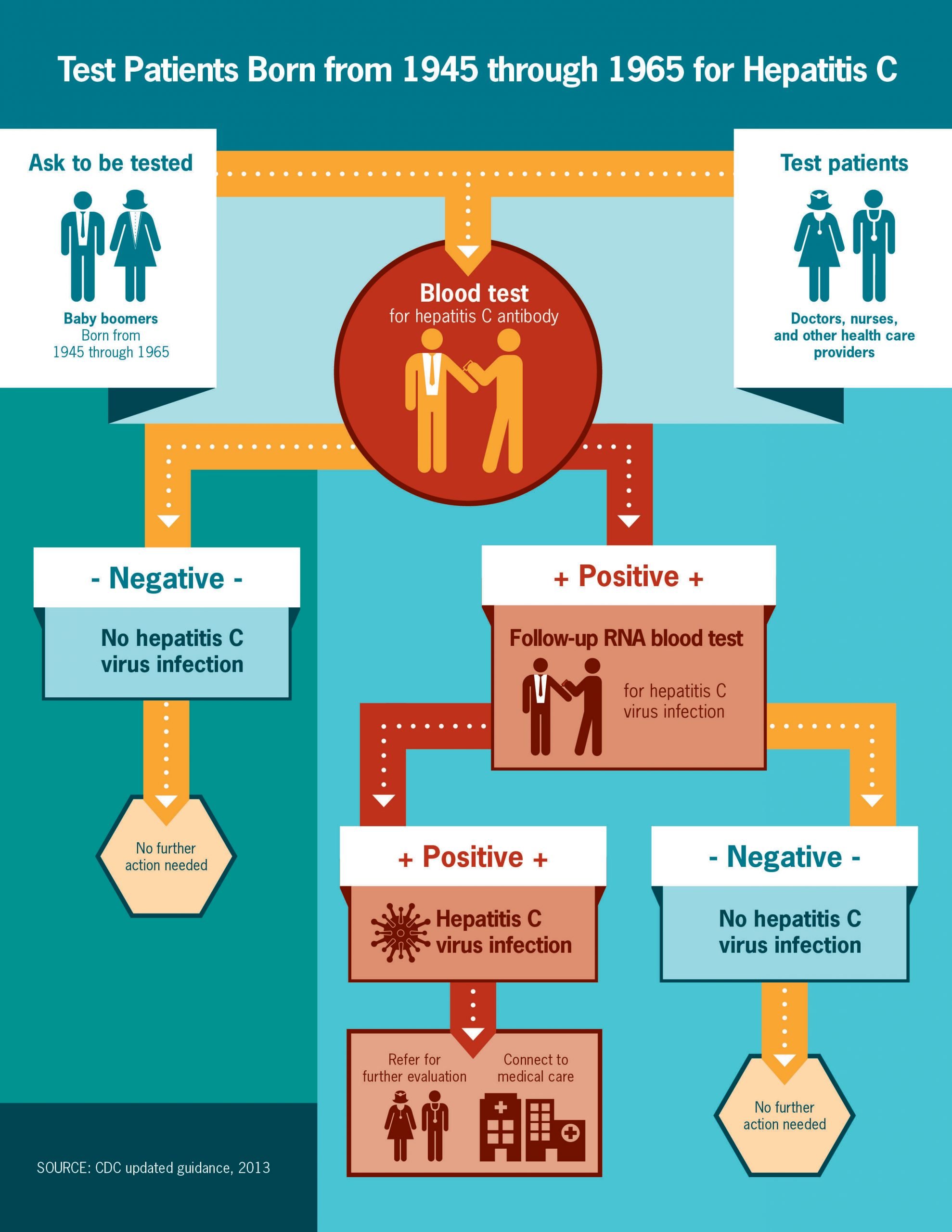
Also, the U.S. Preventive Services Task Force recommends that health care providers offer a one-time hepatitis C screening for anyone born between 1945 and 1965.
Don’t Miss: Hepatitis A Vaccine At Cvs
How Can You Prevent Hepatitis B And Hepatitis C
Hepatitis B: Vaccination is the best way to prevent all of the ways that hepatitis B is transmitted. People with HIV who do not have active HBV infection should be vaccinated against it. In addition to the 3-dose series of hepatitis B vaccine given over 6 months, as of 2017, there is a 2-dose series given over 1 month.
Hepatitis C: No vaccine exists for HCV and no effective pre- or postexposure prophylaxis is available. The best way to prevent hepatitis C infection is to never inject drugs or to stop injecting drugs by getting into and staying in drug treatment. If you continue injecting drugs, always use new, sterile needles or syringes, and never reuse or share needles or syringes, water, or other drug preparation equipment.
Acute Hepatitis B Infection
There is no specific treatment for acute hepatitis B, and most people recover within one to two months. Usually, you can manage symptoms at home with painkillers if necessary. Your healthcare professional should advise you to have regular blood tests and physical check-ups. Most people make a full recovery from acute hepatitis B.
Recommended Reading: How Does Hepatitis C Affect The Liver
Sexual Transmission And Hepatitis A
Transmission of hepatitis A virus can occur from any sexual activity with an infected person and is not limited to fecal-oral contact. People who are sexually active are considered at risk for hepatitis A if they are MSM, live with or are having sex with an infected person, or inject drugs. Vaccination is the most effective means of preventing hepatitis A transmission among people at risk for infection. CDC has published recommendations for prevention of hepatitis A that identify all groups recommended for vaccination, including hepatitis A vaccination for MSM.
Are Hepatitis B And C Preventable
Hepatitis B is a vaccine-preventable disease.
There is a three-shot vaccination series that is very effective in protecting people against the virus if theyre exposed. In the United States, all newborns are vaccinated for hepatitis B and all pregnant women are screened for hepatitis B during pregnancy. This way, mothers infected with hepatitis B can take protective steps to decrease the risk of transmission of the virus to the child.
There is no vaccine for hepatitis C.
Also Check: Where To Get Hepatitis B Test