Taking A Hepatitis C Test
Hepatitis C testing is conducted on a sample of blood. Blood samples can be collected by a doctor, nurse, technician, or other health care provider from an adult patients vein using a small needle or a skin prick on a childs heel.
For an at-home hepatitis C test, patients collect a blood sample according to the manufacturers directions. Instructions provided in the test kit detail the steps to obtain a small sample of blood and mail it for testing.
When Should I Get Tested For Hepatitis C
You should get tested for hepatitis C if you have any of the following symptoms:
- A high level of liver enzymes in your blood, such as alanine aminotransferase or aspartate aminotransferase
- A significant increase in liver enzymes
- A significant increase in liver size
You do not need to get tested for hepatitis C if you feel well. Your doctor will assess your risk of developing the condition and advise you if and when you should get tested.
You can get tested for hepatitis C at a number of locations, including:
- Your primary care doctor.
How Do Doctors Treat Hepatitis C
Doctors treat hepatitis C with antiviral medicines that attack the virus and can cure the disease in most cases.
Several newer medicines, called direct-acting antiviral medicines, have been approved to treat hepatitis C since 2013. Studies show that these medicines can cure chronic hepatitis C in most people with this disease. These medicines can also cure acute hepatitis C. In some cases, doctors recommend waiting to see if an acute infection becomes chronic before starting treatment.
Your doctor may prescribe one or more of these newer, direct-acting antiviral medicines to treat hepatitis C:
You may need to take medicines for 8 to 24 weeks to cure hepatitis C. Your doctor will prescribe medicines and recommend a length of treatment based on
- which hepatitis C genotype you have
- how much liver damage you have
- whether you have been treated for hepatitis C in the past
Your doctor may order blood tests during and after your treatment. Blood tests can show whether the treatment is working. Hepatitis C medicines cure the infection in most people who complete treatment.
Hepatitis C medicines may cause side effects. Talk with your doctor about the side effects of treatment. Check with your doctor before taking any other prescription or over-the-counter medicines.
For safety reasons, talk with your doctor before using dietary supplements, such as vitamins, or any complementary or alternative medicines or medical practices.
Don’t Miss: Is Hepatitis B And Hiv The Same Thing
Time For Processing Hcv Ab Test Results
The turnaround time for 3rd-generation EIAs is at least 1 day. Many labs do not perform the tests on site and must send specimens to another lab for processing, which may further increase the turnaround time.
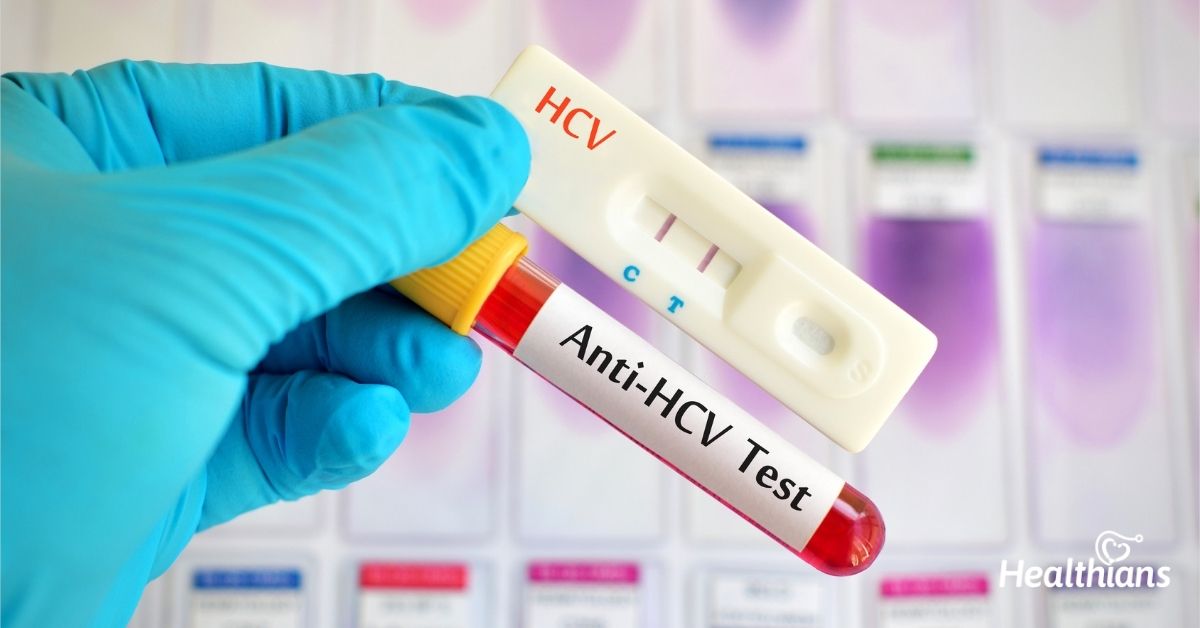
A point-of-care test is also available. The OraQuick® HCV Rapid Antibody Test is an FDA-approved test that can be performed with a fingerstick . It is also a CLIA-waived test and therefore can be used in clinic offices and outreach facilities. Results are reported as reactive or nonreactive within 20 minutes. Just as for the standard HCV Ab test done in the lab, a positive OraQuick® test must be confirmed by an HCV RNA test. The sensitivity and specificity of the test is similar to that of the laboratory-based assays.
Lifestyle And Home Remedies For Hepatitis C Infection
If you receive a diagnosis of hepatitis C, your doctor will likely recommend certain lifestyle changes. These measures will help keep you healthy longer and protect the health of others as well:
- Stop drinking alcohol. Alcohol speeds the progression of liver disease.
- Avoid medications that may cause liver damage. Review your medications with your doctor, including over-the-counter medications you take as well as herbal preparations and dietary supplements. Your doctor may recommend avoiding certain medications.
- Help prevent others from coming in contact with your blood. Cover any wounds you have and dont share razors or toothbrushes. Dont donate blood, body organs or semen, and advise health care workers that you have the virus. Also tell your partner about your infection before you have sex, and always use condoms during intercourse.
What should I eat and drink if I have hepatitis C?
If you have hepatitis C, you should eat a balanced, healthy diet. Talk with your doctor about healthy eating. You should also avoid alcohol because it can cause more liver damage.
Also Check: Difference Between Hepatitis B And C
Normally Where Are The Aminotransferases
AST is normally found in a diversity of tissues including liver, heart, muscle, kidney, and brain. It is released into serum when any one of these tissues is damaged. For example, its level in serum rises with heart attacks and with muscle disorders. It is therefore not a highly specific indicator of liver injury.
ALT is, by contrast, normally found largely in the liver. This is not to say that it is exclusively located in liver but that is where it is most concentrated. It is released into the bloodstream as the result of liver injury. It therefore serves as a fairly specific indicator of liver status.
Recommended Reading: How Do You Get Hepatitis A B C
Natural History Following Infection With Hcv
Hepatitis C can present as acute or chronic hepatitis. Most of the cases of acute hepatitis C are asymptomatic. Symptomatic acute hepatitis with jaundice is seen in 10-15% of patients only and can be severe, but fulminant liver failure is rare. Spontaneous clearance is observed in 25-50% of those with symptomatic infection and in 10-15% of those with asymptomatic infection. The natural history following exposure to HCV is summarized in .
Natural history following infection with hepatitis C virus
Chronic hepatitis C is marked by the persistence of HCV RNA in the blood for at least 6 months after the onset of acute infection. The risk of progression to chronic infection by HCV is influenced by various factors including:
-
Age at the time of infection
-
Gender
-
Ethnicity
-
Coinfection with human immunodeficiency virus , HBV
-
Concomitant alcohol consumption
-
Comorbid conditions like cancer, immunosuppression, insulin resistance, nonalcoholic steatohepatitis, obesity, etc.
You May Like: What Are The Effects Of Hepatitis C
Gap In Linkage To Care
Unfortunately, many individuals diagnosed with HCV infection do not get linked to appropriate care for their HCV infection. Multiple reasons for the gap in linkage to care have been cited, including failure of the medical provider to make the referral, lack of medical insurance, and substance use or mental health disorders that interfere with making or keeping the referral appointment. Linkage to care rates have been lower among racial and ethnic minorities. Failure to link to care negatively impacts health outcomes in persons living with HCV infection. With highly effective HCV treatment now available for all HCV genotypes, referral for evaluation and management of HCV has taken on even greater importance.
What Is The Risk That An Hepatitis C Virus
Approximately 6 of every 100 infants born to hepatitis C virus-infected mothers become infected with the virus. Transmission occurs at the time of birth, and no prophylaxis is available to prevent it. The risk is increased by the presence of maternal hepatitis C virus viremia at delivery and also is 23 times greater if the woman is coinfected with HIV. Most infants infected with hepatitis C virus at birth have no symptoms and do well during childhood. More research is needed to find out the long-term effects of perinatal hepatitis C virus infection.
Read Also: Hepatitis B Surface Antibody Titer Test
Besides Hcv Testing What Other Tests Might Be Done
Healthcare practitioners may also order a liver panel, which is a group of tests that help assess the health of your liver. Liver tests such as ALT and AST may be used to detect ongoing liver injury. You will likely be checked to see if you are immune to hepatitis A and hepatitis B, and if not, you will be offered vaccination, since infection with these other viruses can further damage your liver. Other tests such as albumin, prothrombin time, and bilirubin can also be used. They are typically normal unless you have developed cirrhosis. Sometimes a liver biopsy may be performed to determine the severity of liver damage. If you are going to be treated, you will be checked for exposure or infection with hepatitis B virus, as HCV treatment can cause a flare-up of hepatitis B.
Recommended Laboratory Evaluation Prior To Referral
All persons referred for further evaluation and management of HCV infection should have a confirmed positive HCV RNA level, preferably a quantitative HCV RNA level and not a qualitative HCV RNA level. It is ideal, but not imperative, that the clinician who makes the diagnosis of HCV infection can perform some preliminary tests to provide advanced information in anticipation of the initial referral visit. These initial preliminary tests include an HCV genotype, tests of synthetic liver function , hepatic inflammation , and assays to detect relevant coinfection . For primary care providers taking on a more comprehensive role for the initial evaluation and management, see Module 2, Lesson 1 for a detailed discussion in the Core Concept Initial Evaluation of Persons with Chronic Hepatitis C.
Read Also: Is Hepatitis B The Same As Hiv
Why Was This Test Discontinued
The HCV RIBA test was eventually phased out. This is because its been replaced by more sensitive tests that can give your doctor more details about your bodys response to the presence of HCV. Many tests can also detect HCV viremia, which is a much more accurate tool for confirming an infection than a simple positive/negative antibody result.
The Centers for Disease Control and Prevention discontinued the HCV RIBA test in 2013. As a result, companies that once made the test, such as the pharmaceutical company Novartis AG, largely dont sell the test to laboratories anymore.
This test isnt completely obsolete.
Some laboratory testing facilities still use the test as part of HCV screening procedures.
And some blood banks use the HCV RIBA test to confirm the presence of HCV antibodies before a donated blood sample can be used. If the blood gets a positive HCV RIBA test result, it may need further HCV testing before its considered safe to use.
Diagnosing Hepatitis A B & C
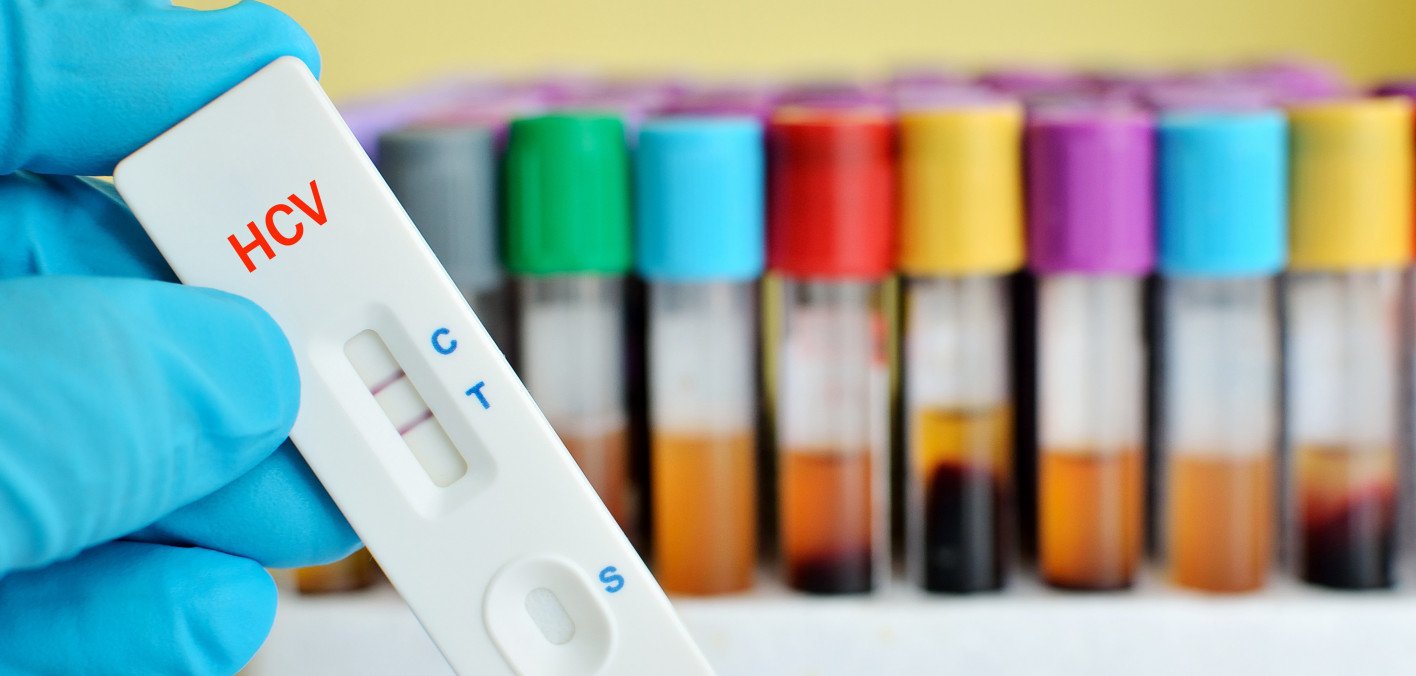
At NYU Langone, hepatologists, or liver specialists, and infectious disease specialists use blood tests to diagnose hepatitis A, B, and C. These viral infections cause inflammation of the liver.
If the results of a blood test confirm a diagnosis of viral hepatitis, your doctor may recommend imaging tests or a liver biopsy to determine the extent of liver disease.
Also Check: Hepatitis C And Liver Damage
What Is The Outlook For People With Hepatitis C
If you have hepatitis C, it is important to seek treatment as soon as possible.
As the disease progresses, your liver will become damaged. This will lead to liver inflammation.
Without treatment, the inflammation can become serious and lead to liver failure.
In the United States, there is an estimated 30,000 new cases of hepatitis C per year, according to the Centers for Disease Control and Prevention . However, it is impossible to accurately calculate the number of people with the disease worldwide.
Your doctor can give you a better estimate of your risk for developing the condition.
If you have hepatitis C, its important to check that you have tested regularly for the infection. This will help ensure that you receive the right treatment at the right time.
How Does Hepatitis C Spread
The most common way to contract Hepatitis C is through needles . Pregnant women infected with Hepatitis C can spread the virus to their children at the time of birth. Less common ways to spread Hepatitis C include sexual contact, sharing personal care items like razors, and getting body modification procedures, such as tattoos and piercings, in non-sterile environments.
Read Also: Is Hepatitis C Contagious By Touch
Who Is More Likely To Get Hepatitis C
People more likely to get hepatitis C are those who
- have injected drugs
- had a blood transfusion or organ transplant before July 1992
- have hemophilia and received clotting factor before 1987
- have been on kidney dialysis
- have been in contact with blood or infected needles at work
- have had tattoos or body piercings
- have worked or lived in a prison
- were born to a mother with hepatitis C
- are infected with HIV
- have had more than one sex partner in the last 6 months or have a history of sexually transmitted disease
- are men who have or had sex with men
In the United States, injecting drugs is the most common way that people get hepatitis C.13
Immunoassays For Hcv Core Antigen
As an HCV diagnostic marker, HCV core antigen has been studied, either alone or as an HCV antibody-HCV antigen combination assay. Some experts have proposed use of an HCV core antigen test as a less expensive option than HCV RNA testing, but there are no HCV antigen assays that are FDA-approved for use in the United States at this time.
Recommended Reading: How Many Types Of Hepatitis C Are There
Positive Hcv Antibody And Negative Hcv Rna
Individuals with a positive HCV antibody test and a negative HCV RNA should be informed they do not have evidence of current hepatitis C infection. It should be explained to the patient that most likely they were infected at some time with HCV, but cleared the infection on their own and they do not have current infection. They do not need further follow-up HCV testing, unless they had recent exposure to HCV. A single negative HCV RNA value does not prove that a patient is not infected, given the potential fluctuations of the viral level early in HCV infection a follow-up HCV RNA level would be indicated depending on the clinical case. Patients should be reevaluated if they have exposure to HCV in the future. In addition, they should receive counseling that prior infection does not make them immune to reinfection with HCV.
Positive Hcv Antibody And Positive Hcv Rna
Individuals with a positive HCV EIA and positive HCV RNA should be told they have evidence of active hepatitis C infection and they should clearly understand they need medical follow-up evaluation and potential treatment of liver disease. A single positive HCV RNA value indicates infection, but must be interpreted in the context of clinical history to determine whether the individual has acute or chronic infection. For persons with a positive HCV EIA and positive HCV RNA, the CDC has generated counseling messages that focus on four areas: contacting a health care provider for further evaluation and management of their HCV infection, protecting their liver from further harm, addressing weight management in overweight and obese persons, and minimizing transmission of their HCV to others . In addition, the CDC recommends performing alcohol screening and brief intervention, which consists of screening for excessive alcohol consumption, brief counseling for individuals who screen positive, and referral to a specialized alcohol treatment program for individuals with possible alcohol dependence.
Don’t Miss: When Do Hepatitis C Symptoms Appear
Relationship Of Symptoms And Spontaneous Clearance
Overall, when combining data from multiple historical studies, approximately 25 to 35% of person with acute HCV infection have spontaneous clearance of HCV. The rates of spontaneous clearance are significantly lower in persons who are Black and in those individuals who have HIV coinfection. In contrast, rates of spontaneous clear are higher in females and in persons who acquired HCV in childhood. It has also been demonstrated that patients who present with symptomatic acute HCV infection and jaundice have higher rates of spontaneous clearance of HCV, in the range of 35 to 50%. The presence of jaundice is believed to reflect hepatic inflammation caused by a more robust initial immune response against HCV.
Virological Tools For Diagnosis
Virological diagnosis of HCV infection is based on two categories of laboratory tests, namely serologic assays detecting specific antibody to HCV and assays that can detect, quantify, or characterize the components of HCV viral particles, such as HCV RNA and core antigen . Direct and indirect virological tests play a key role in the diagnosis of infection, therapeutic decision-making, and assessment of virological response to therapy.
Recommended Reading: How Do You Get Hepatitis A
When To Get Tested
For screening: at least once when you are age 18 years or older when you are pregnant when you have risk factors for HCV infection, regardless of age
For diagnosis: when you may have been exposed to the hepatitis C virus, such as through injection drug use, or when you have signs and symptoms associated with liver disease
For monitoring: before, during, and after hepatitis C treatment
Hcv Core Antigen Detection
During the past decade, several assays for the detection of the core antigen of HCV by ELISA or CLIA have been developed. These assays were envisioned as alternatives to NAT to be used in resource-limited settings, where molecular laboratory services are either not available or not widely utilized owing to cost issues. Since these assays are either ELISA or CLIA based, they are user friendly, require less technical expertise and are less expensive compared to molecular techniques. Evaluations in transfusion settings have shown that the HCVcore Ag assay detects HCV infection as effective as NAT, about 40-50 days earlier than the current third generation anti-HCV screening assays. HCV core antigen levels closely follow HCV RNA dynamics, and allow clinical monitoring of a patient’s therapy, independently of HCV genotype. The major limitation of the HCV core Ag assay is its lower sensitivity limiting its utility. A new generation CLIA based quantitative test with sensitivity comparable to that of end point PCR but less than that of real time RT-PCR has been reported.
You May Like: How Does A Person Contract Hepatitis C