Signs Of Worsening Hep C Or Liver Disease
When chronic hep C remains untreated, it can cause liver scarring , liver cancer, or failure. The symptoms of cirrhosis include jaundice, weight loss, itchy skin, vomiting of blood, darkened urine or bowel movements, confusion, drowsiness and slurred speech , and build-up of fluid in the legs or abdomen.2
Who Should Be Tested For Hepatitis C
- All people born between 1945 and 1965
- Anyone who has ever injected drugs, even if once or many years ago
- People with HIV infection
- People who had a blood transfusion organ transplantation before 1992
- People who have been exposed to blood on the job through a needle stick or other injury
- People receiving hemodialysis
- People who have abnormal liver tests or liver disease
What Are The Complications Of Undiagnosed Hepatitis C
- Hepatitis C is known to be associated with two skin conditions, lichen planus and porphyria cutanea tarda.
- Diabetes, heart disease, and arterial blockage are more common among patients with chronic hepatitis C infection than in the general population. It may be that liver damage and chronic inflammation caused by hepatitis C may affect the levels of blood fats and blood sugar.
- Low platelet counts may occur as a result of the destruction of platelets by antibodies.
Don’t Miss: Can Hepatitis B Cause Meningitis
Contaminated Needles And Infected Blood
You can get hepatitis C from sharing contaminated needles, syringes and other injecting equipment during recreational drug use. Banknotes and straws used for snorting may also pass the virus on.
Being exposed to unsterilised tattoo and body piercing equipment can also pass hepatitis C on. Occasionally, you can get it from sharing a towel, razor blades or a toothbrush if there is infected blood on them.
Hepatitis C infection is also passed on in healthcare settings, from needle stick injuries or from medical and dental equipment that has not been properly sterilised. In countries where blood products are not routinely screened, you can also get hepatitis C by receiving a transfusion of unscreened blood and blood products.
You can prevent hepatitis C by:
- never sharing needles and syringes or other items that may be contaminated with infected blood
- only having tattoos, body piercings or acupuncture in a professional setting, where new, sterile needles are used
- following the standard infection control precautions, if youre working in a healthcare setting.
Alcohol And Other Toxins
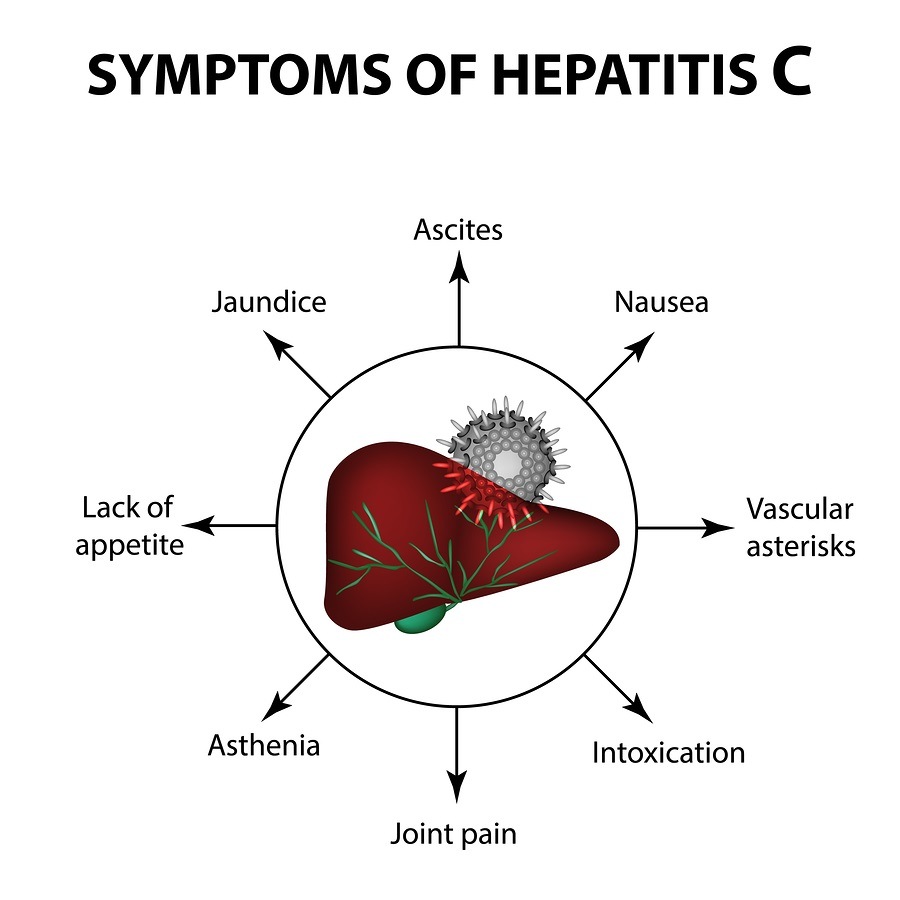
Excessive alcohol consumption can cause liver damage and inflammation. This is sometimes referred to as alcoholic hepatitis. The alcohol directly injures the cells of your liver. Over time, it can cause permanent damage and lead to liver failure and cirrhosis, a thickening and scarring of the liver.
Other toxic causes of hepatitis include overuse or overdose of medications and exposure to poisons.
Don’t Miss: Hepatitis C Symptoms Mayo Clinic
Who Is Most At Risk Of Contracting Hepatitis C
You have a high risk of contracting hepatitis C if you:
- use or have used injection drugs even if it was just once or many years ago
- have received blood or blood products or an organ transplant before July 1990 in Canada
- have been in jail or
- have been injected or scratched during vaccination, surgery, blood transfusion or a religious/ceremonial ritual in regions where hepatitis C is common.
You have a high moderate risk of contracting hepatitis C if you:
- have tattoos or body piercing
- have multiple sexual partners
- have a sexually transmitted infection , including HIV or lymphogranuloma venereum
- have experienced traumatic sex or rough sex or have used sex toys or fisting that can tear body tissue
- have vaginal sex during menstruation
- have received a kidney treatment
- have received an accidental injury from a needle or syringe
- have another infectious disease
- were born to a hepatitis C infected mother or
- have a sexual partner infected with hepatitis C.
Hepatitis C is NOT passed from person to person by:
- coughing, sneezing
- breastfeeding unless your nipples are cracked and bleeding or
- oral sex, unless blood is present.
The Acute Phase Of Hepatitis C
The term Acute Phase can be confusing. This is because it only refers to the 6 month period of time after the virus has first entered your body. It bears no relation to the acuteness of the symptoms or the severity of the disease.Antibodies to the virus are produced by your immune system when it reacts to the presence of the virus and are detectable in the blood from between 3 to 12 weeks after initial infection. Depending on how long it takes for the virus to take hold in the body, different immune systems will take different amounts of time to create antibodies. This is called the window period. Because it can take up to 3 months for the antibodies to show up in a blood test, if you suspect you have recently been infected, it is important to wait this long before having a test. If the antibody test is positive you will be offered a PCR or RNA test.
Symptoms during the Acute Phase
During the acute phase most people do not seem to experience any noticeable symptoms. For the 25-35% of people who do, the symptoms are normally vague and non-specific. They can include low-grade fever, fatigue, appetite loss, abdominal pain, nausea and vomiting. About 20% of the people who develop symptoms contract jaundice. This can be seen in the yellowing of the skin and eyes. This is a sign of the livers functions being affected as bilirubin begins to build up in the body. Jaundice is a recognised sign of liver problems and may lead to a test for hepatitis C being suggested.
You May Like: How Can You Pass Hepatitis C
What Are The Treatments For Hepatitis C
Treatment for hepatitis C is with antiviral medicines. They can cure the disease in most cases.
If you have acute hepatitis C, your health care provider may wait to see if your infection becomes chronic before starting treatment.
If your hepatitis C causes cirrhosis, you should see a doctor who specializes in liver diseases. Treatments for health problems related to cirrhosis include medicines, surgery, and other medical procedures. If your hepatitis C leads to liver failure or liver cancer, you may need a liver transplant.
What Occupations Have Increased Risk Of Hepatitis C
The risk of acquiring hepatitis C from the workplace depends on the amount of exposure to human blood or blood products and needlestick injuries. In general, occupational groups with increased risk include workers such as healthcare workers, dentists, and laboratory personnel who are repeatedly exposed to human blood and who are at risk of needlestick injuries.
You May Like: Causes And Symptoms Of Hepatitis
What The Cdc Recommends
Were you born between 1945 and 1965? If so, then youre a member of the Hepatitis C generation. The CDC recently recommended that all people born between during this time have a 1-time screening test for Hepatitis C. We now have new drugs that can treat and cure Hepatitis C so you should go get tested today.
The life you save may be your own! Please contact your local healthcare provider.
How Is Hepatitis C Treated
There are some very effective options for the treatment of hepatitis C infection. They are listed on the Medicare PBS , which makes them available at a much lower cost.
Newer treatments differ from those available previously:
- they cure more than 95% of people
- their side effects are minimal
- treatments last just 8 to 12 weeks
- they involve just a few pills each day, with no injections required
Curing hepatitis C means clearing the virus from the body. It helps reduce liver inflammation and can also help reverse scarring and cirrhosis. You can be re-treated if your treatment doesnt work the first time.
You should check with your doctor before taking any other medication or supplements, and whether you need vaccinations against hepatitis A and hepatitis B. You should also avoid alcohol if you have hepatitis. If you have liver damage, you may also need to see a liver specialist
For more information on how to get treatment, contact the National Hepatitis Info Line on 1800 437 222.
Also Check: What Does Hepatitis C Cause
How Long Does Hepatitis C Appear Symptom
Patients with hepatitis C virus infection will have recurrent urticaria skin symptoms, which means that the virus in vivo, human replication, disease instability, or HCV infection.
If the anti HCV antibody is positive, the skin symptoms of patients infected with HCV are pruritus, which means that the disease is stubborn and the treatment is difficult.
The skin symptoms of patients infected with hepatitis C virus were flat polygon papules, dark red or purplish red, glossy surface, or large papules scattered on the tip of the needle, linear or reticular arrangement, most likely lichen planus. About 37% of hepatitis C patients were in the unstable stage, and the improvement of hepatitis C subsided, and the aggravation of hepatitis C worsened.
Can Hepatitis C Be Treated

Yes, since 2010 enormous progress has been made in the treatment of chronic hepatitis C. New therapies called direct-acting antivirals are pills that act on the virus itself to eradicate it from the body, unlike older medicines like interferon injections which work by stimulating an immune response. These new treatments are very effective and can achieve cure rates of over 90%. In most situations now, there is no need for interferon, which was responsible for many of the side effects previously associated with HCV treatment. The new treatment combinations require shorter treatment durations , have reduced side effects and appear to be effective at all stages of the disease.
Because these new therapies are very new, they remain very expensive. As such, drug coverage from both government and private companies may require that your liver disease has progressed to a certain stage before they are willing to cover the cost of these drugs.
Your primary care physician may refer you to a specialist to determine whether you are eligible for treatment. A specialist will help you decide which drug therapy is best for you based on the severity of your liver disease, your virus genotype and whether or not you have been treated in the past.
Read Also: How Do You Get Hepatitis Ab And C
How Is Monitoring Done After Treatment For Hepatitis C
Once patients successfully complete treatment, the viral load after treatment determines if there is an SVR or cure. If cure is achieved , no further additional testing is recommended unless the patient has cirrhosis. Those who are not cured will need continued monitoring for progression of liver disease and its complications.
While cure eliminates worsening of fibrosis by hepatitis C, complications may still affect those with cirrhosis. These individuals still need regular screening for liver cancer as well as monitoring for esophageal varices that may bleed.
Because hepatitis B co-infection may reactivate or worsen even after treatment for HCV, monitoring for hepatitis symptoms may be needed after the end of therapy.
Hepatitis C And Liver Transplantation
Some people with advanced hepatitis C infection and severe liver damage undergo a liver transplant, but that doesn’t eradicate the infection. Patients with active infection at the time of the transplant will develop hepatitis C in the new liver. Sometimes the infection recurs even when patients are on antiviral treatment. Those who have achieved sustained virologic response – meaning no detectable virus in the blood 6 months after treatment – have a very low risk of developing hepatitis C infection in the new liver.
Recommended Reading: Hepatitis B Surface Ab Ql Reactive
Symptoms Of Hepatitis C Virus
Symptoms for HCV may not appear for 20 to 30 years, and that is why it is so important to get tested. The U.S. Centers for Disease Control now recommends that all adults 18 years and older are tested at least once for HCV. Some high risk groups may need more frequent testing, and all pregnant women should be tested during every pregnancy.
HCV can actually clear itself from the body in about 15% of people, but most people become infected with the virus chronically.
Early symptoms of acute HCV occur within 1 to 3 months and may last several weeks. These may include:
- yellow-colored skin or eye sclera
- weakness
- nausea and stomach pain
- joint or muscle pain
Chronic, long-term symptoms of HCV can include weight loss, fluid build-up and swelling, poor appetite, fatigue, easy bruising and bleeding, itchy skin, jaundice, dark-colored urine, confusion, drowsiness and slurred speech , and spider-like blood vessels on the skin .
When Should I Get Hepatitis C Testing
When used for early detection in patients without symptoms of hepatitis C, screening is recommended at least once for all adults aged 18 years or older, except in locations with very low prevalence of HCV. Screening is also recommended during pregnancy and for patients of any age with risk factors for HCV infection. In patients with risk factors, periodic screening is recommended for as long as risk factors persist.
Risk factors for HCV include:
- Current or past injectable drug use
- Having a blood transfusion or organ transplant before July 1992
- Receiving kidney dialysis
- Pain in the abdomen or joints
- Nausea, vomiting, or loss of appetite
- Jaundice or yellowish skin and eyes
Hepatitis C testing may also be performed when liver tests are abnormal or when diagnosing the cause of existing liver damage.
You May Like: Does The Hpv Vaccine Protect Against Hepatitis B
How Do Doctors Treat Hepatitis C
Doctors treat hepatitis C with antiviral medicines that attack the virus and can cure the disease in most cases.
Several newer medicines, called direct-acting antiviral medicines, have been approved to treat hepatitis C since 2013. Studies show that these medicines can cure chronic hepatitis C in most people with this disease. These medicines can also cure acute hepatitis C. In some cases, doctors recommend waiting to see if an acute infection becomes chronic before starting treatment.
Your doctor may prescribe one or more of these newer, direct-acting antiviral medicines to treat hepatitis C:
You may need to take medicines for 8 to 24 weeks to cure hepatitis C. Your doctor will prescribe medicines and recommend a length of treatment based on
- which hepatitis C genotype you have
- how much liver damage you have
- whether you have been treated for hepatitis C in the past
Your doctor may order blood tests during and after your treatment. Blood tests can show whether the treatment is working. Hepatitis C medicines cure the infection in most people who complete treatment.
Hepatitis C medicines may cause side effects. Talk with your doctor about the side effects of treatment. Check with your doctor before taking any other prescription or over-the-counter medicines.
For safety reasons, talk with your doctor before using dietary supplements, such as vitamins, or any complementary or alternative medicines or medical practices.
Who Is At Risk For Hepatitis C
You are more likely to get hepatitis C if you
- Have injected drugs
If you have chronic hepatitis C, you probably will not have symptoms until it causes complications. This can happen decades after you were infected. For this reason, hepatitis C screening is important, even if you have no symptoms.
Also Check: Hepatitis B And Rheumatoid Arthritis Treatment
Easy Bleeding And Bruising
Your liver makes the things that help your blood clot. When itâs damaged, it canât make enough. You might start to bleed easily and have trouble stopping it. Or you might bruise easily.
Tell your dentist or other doctors before you have any medical procedure. Treat cuts with pressure bandages and get to the doctor right away. In an emergency, youâll get platelets to replace what you lost and Vitamin K to help your blood clot. View a slideshow on the basics of bruises.
How Do People Get Hepatitis C
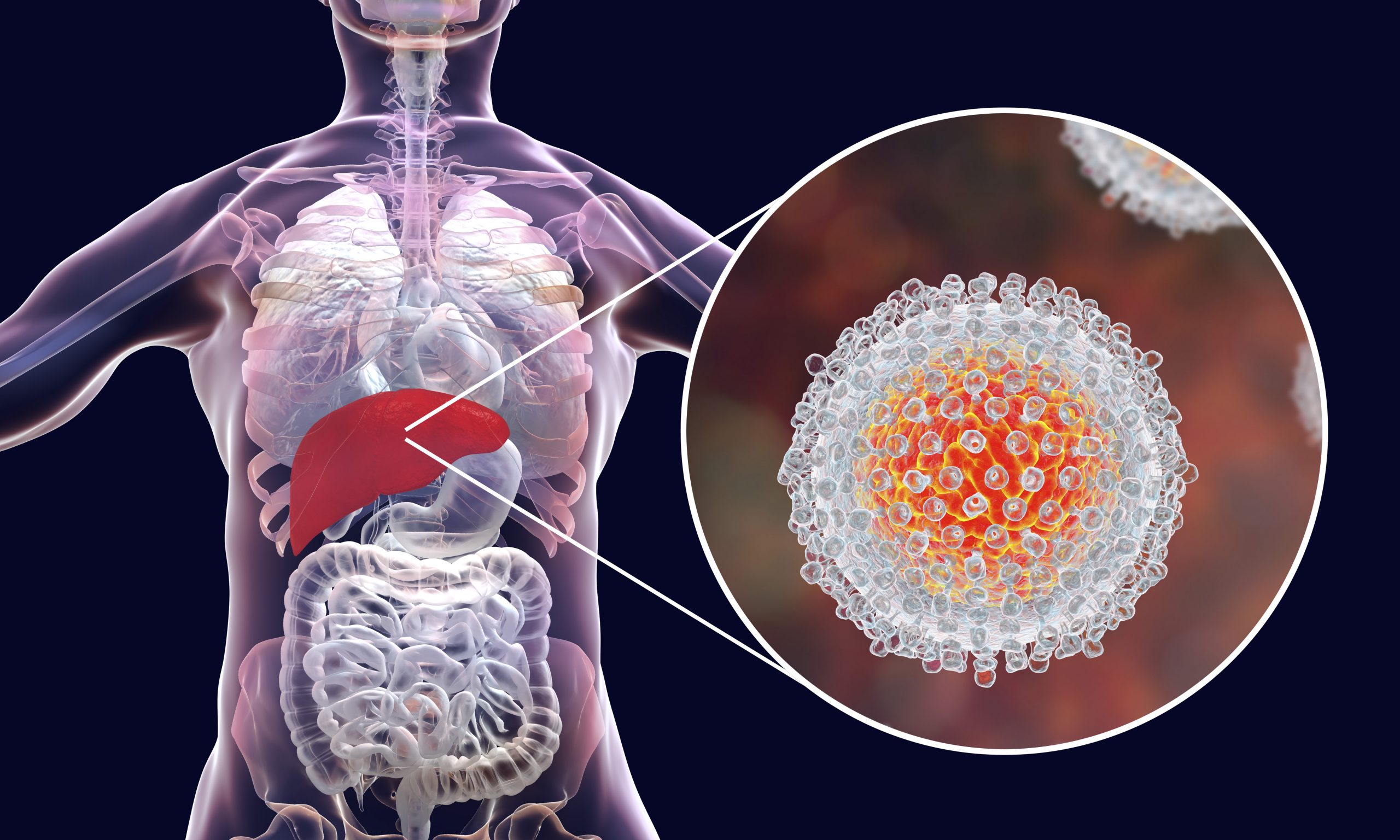
Hepatitis C virus is found in the blood of people with HCV infection. It enters the body through blood-to-blood contact.
Until reliable blood tests for HCV were developed , people usually got hepatitis C from blood products and blood transfusions. Now that blood and blood products are tested for HCV, this is no longer the typical means of infection.
Currently, people usually get hepatitis C by sharing needles for injection drug use. An HCV-infected woman can pass the infection to her baby during birth. It is also possible to get hepatitis C from an infected person through sexual contact, an accidental needlestick with a contaminated needle, or improperly sterilized medical, acupuncture, piercing, or tattooing equipment.
Also Check: Is There A Pill That Cures Hepatitis C
What Drugs Treat And Cure Hepatitis C
The treatment of chronic hepatitis C has gone through several generations of medications. Not long ago, treatment was limited to interferon alpha-2b or pegylated interferon alpha-2b , and ribavirin . Interferon and pegylated interferon need to be injected under the skin , while ribavirin is taken by mouth. This combination therapy is infrequently used today, being recommended for only the least common genotypes of hepatitis C virus .
Since 2010, direct-acting antiviral drugs have been in use. The second generation of antivirals for HCV was the protease inhibitors telaprevir and boceprevir , both taken by mouth. These were used in combination with the earlier drugs to increase effectiveness . These drugs are also no longer in common use, and have been replaced by better options.
As more has been learned about how hepatitis C virus multiplies within the liver cells, new drugs continue to be developed to interfere with this multiplication at different stages. As such, we no longer think in terms of generations of drugs, but rather categories of action. Research and development of these direct-acting antivirals continue, with new agents coming to market every few months. Each category is improved and expanded by the addition of new drugs, which are safer and more effective.
Currently available and commonly used direct-acting antiviral drugs include:
- simeprevir
- Muscle aches