Treatment Of Hepatitis C
Unlike hepatitis A and B, there is no vaccine available for hepatitis C. Fortunately, both acute and chronic hepatitis C infections are curable.
Current hepatitis C treatments involve taking two or more medications known as direct antiviral agents, or DAAs. This combination of medications prevents HCV from replicating until the virus is no longer present in the body. Treatment usually takes 6 to 24 weeks but can take longer.
However, people who have both HIV and HCV need individualized treatments because the medications used to treat HCV infections can interact with HIV treatments.
A doctor will recommend a treatment plan based on the individualâs:
- hepatitis C genotype
Epidemiology And Pathogenesis Of Hcp
Question: What factors contribute to the pathogenesis and risk for transmission of HIV, HCV, and HBV from HCP to patients?
Answer: Virtually no new information has surfaced about the healthcare-associated epidemiology, pathogenesis, or transmission of HBV, HCV, and HIV since the publication of the 2010 SHEA guideline. As noted in the introduction, with the exception of cases linked to HCP substance use,Reference Hellinger, Bacalis and Kay19–Reference Williams, Perz and Bell27 literature reports documented no new cases of HIV, 3 cases of HCV,Reference Bourigault, Nael and Garnier28–Reference Roy, Galmes-Truyols and Gimenez-Duran30 and 2 cases of HBV transmission from HCP to patients.Reference Enfield, Sharapov and Hall14,Reference Sugimoto, Nagakubo and Ito15 The contribution of HCP substance use to HCP-to-patient HCV and HBV cases should not be overlooked. When transmission is documented, HCP substance use must be considered and excluded. In addition, staff should be made aware of institution-based HCP substance use detection programs.Reference Berge, Dillon, Sikkink, Taylor and Lanier36 Nonetheless, with perhaps the exception of the relatively new issue of the opioid epidemic involving HCP, the few instances of transmission provided limited new insights about the factors that influence transmission.
The 5 factors identified by the 2010 SHEA guideline as contributors to the pathogenesis and transmission risk for HBV, HCV, and HIV remain:
Is There A Cure
Though there is no vaccine for Hepatitis C, treatments can reduce the viral load to undetectable levels which is considered cured or in remission.
The virus is considered cured when it is not detected in your blood 12 weeks after treatment is completed. This is otherwise known as a sustained virologic response .
Hepatitis C is one of the most serious hepatitis viruses. However, with newer treatments developed over the past few years, the virus is much more manageable than it was in the past.
Current antiviral drugs that help cure hepatitis C may also help prevent the health complications of chronic liver disease.
The reports less than half of people who contract the hepatitis C virus may clear it from their bodies without treatment. For this group of people, the virus will be a short-term acute condition that goes away without treatment.
But for most people, acute hepatitis C will likely develop into a chronic condition that requires treatment.
Since the virus often doesnt produce symptoms until after more significant liver damage occurs, its important to get tested for hepatitis C if you think you might have been exposed.
approved the antiviral drug Mavyret for an 8-week treatment period for people with all genotypes of hepatitis C.
This treatment is now being used for many people instead of the 12-week treatment that was previously required.
Noninvasive ways to test for liver damage caused by hepatitis C are also now available to aid in diagnosis.
Don’t Miss: Can Drinking Cause Hepatitis C
Transmission Hbv Hcv And Hiv In Healthcare Settings
HIV, HBV and HCV are spread by contact with the blood of an infected person. The spread of these viruses from one person to another in healthcare settings is rare, but can occur. This contact is primarily through contaminated needles, syringes, or other sharp instruments. Medical experts emphasize that the careful practice of infection control procedures, including standard precautions , protects patients as well as healthcare providers from possible transmission in medical and dental settings.
Cleaning and Disinfection
See table of approved disinfectants in the PDF link below.
What does OSHA currently accept as “appropriate” disinfectants to prevent the spread of HIV and HBV?*
It is important to emphasize the EPA-approved label section titled “SPECIAL INSTRUCTIONS FOR CLEANING AND DECONTAMINATION AGAINST HIV-1 AND HBV Of SURFACES\ OBJECTS SOILED WITH BLOOD\BODY FLUIDS.” On the labels that OSHA has seen, these instructions require:
*Source:
What is the best way to clean up a blood spill?
Infectious Diseases In Saliva

Infectious diseases can be spread through several routes of transmission. Oral transmission refers to the spreading of microbes through saliva or shared foods and drinks.
When a person accidentally consumes microbe-contaminated items, such as saliva during kissing, the swallowing action of the tongue wipes the microbes against the back of the throat, allowing the microbe to enter the body.
Infections, such as mononucleosis caused by Epstein-Barr virus , and cytomegalovirus , are examples of infections spread via oral transmission from virus-containing saliva.
Other infectious microbes that spread through saliva do so by sticking to the inner surface of the cheeks and mouth, the tongue, or teeth. An example is the bacterium Streptococcus, which can cause an array of infections, including gum disease and strep throat.
The surfaces of the respiratory tract are continuous and made up of similar tissues. Microbes that are found in the saliva can generally be found in other parts of the respiratory tract, including the nose and throat. Therefore, even colds and flu can be spread through the saliva.
Don’t Miss: Can You Get Rid Of Hepatitis
Vaccines And Other Biomedical Interventions
Safe and highly effective vaccines are available for 2 STIs: hepatitis B and HPV. These vaccines have represented major advances in STI prevention. The vaccine against hepatitis B is included in infant immunization programmes in 95% of countries and prevents millions of deaths from chronic liver disease and cancer annually.
As of October 2018, the HPV vaccine is available as part of routine immunization programmes in 85 countries, most of them high- and middle-income. HPV vaccination could prevent the deaths of millions of women over the next decade in low- and middle-income countries, where most cases of cervical cancer occur, if high vaccination coverage of young women can be achieved.
Research to develop vaccines against herpes and HIV is advanced, with several vaccine candidates in early clinical development. Research into vaccines for chlamydia, gonorrhoea, syphilis and trichomoniasis is in earlier stages of development.
Other biomedical interventions to prevent some STIs include adult male circumcision and microbicides.
- Male circumcision reduces the risk of heterosexually acquired HIV infection in men by approximately 60% and provides some protection against other STIs, such as herpes and HPV.
- Tenofovir gel, when used as a vaginal microbicide, has had mixed results in terms of the ability to prevent HIV acquisition, but has shown some effectiveness against HSV-2.
What’s The Relationship Between Drug Use And Viral Infections
People who engage in drug use or high-risk behaviors associated with drug use put themselves at risk for contracting or transmitting viral infections such as human immunodeficiency virus , acquired immune deficiency syndrome , or hepatitis. This is because viruses spread through blood or other body fluids. It happens primarily in two ways: when people inject drugs and share needles or other drug equipment and when drugs impair judgment and people have unprotected sex with an infected partner. This can happen with both men and women.
Drug use and addiction have been inseparably linked with HIV/AIDS since AIDS was first identified as a disease. According to the CDC, one in 10 HIV diagnoses occur among people who inject drugs.1 In 2016, injection drug use contributed to nearly 20 percent of recorded HIV cases among menmore than 150,000 patients. Among females, 21 percent of HIV cases were attributed to IDU.2 Additionally, women who become infected with a virus can pass it to their baby during pregnancy, regardless of their drug use. They can also pass HIV to the baby through breastmilk.
Recommended Reading: Hepatic Steatosis Treatment Step By Step
Presentation On Theme: Originally Presented At World Aids Day Observance November 29 2006 Presentation Transcript:
1 HIV/AIDS AND SIMILARLY TRANSMITTED DISEASES: A MATTER OF PERSONAL RESPONSIBILITYOriginally presented atWORLD AIDS DAY OBSERVANCE NOVEMBER 29, 2006San Bernardino Valley College, CaliforniaRonald P. Hattis, MD, MPHBeyond AIDS Foundation
2 Warning!X-rated photos of genital infections with sexually transmitted diseases are included toward the end of this presentation!Viewer discretion advised
3 The AIDS Memorial Quilt In 1987, the Names Project Foundation began a tradition of honoring persons who died of AIDS with hand-made quilts about their lives. Thousands of quilts are shown on display in 1992 in Washington.Beyond AIDS works to control transmission, so that further quilts will be unnecessary
4 How can HIV transmission be controlled?HIV/AIDS does not have:a vaccinea curean environmental fixOnce infected, a person is infectious to others lifelongInfection is symptom-free for years
5 How can HIV transmission be controlled? Transmission routinely occurs before the transmitter is even aware of having been exposed, let alone infectedPrevention therefore depends on reduction of high-risk behavior:by those at risk before they become infectedby those known to already be infected before they transmit the virus
6 How can HIV transmission be controlled? Prevention of HIV/AIDS and similarly transmitted diseases is a matter of personal responsibilityIdentification of infection requires early testing of persons with no symptoms, and intervening rapidly with those testing positive
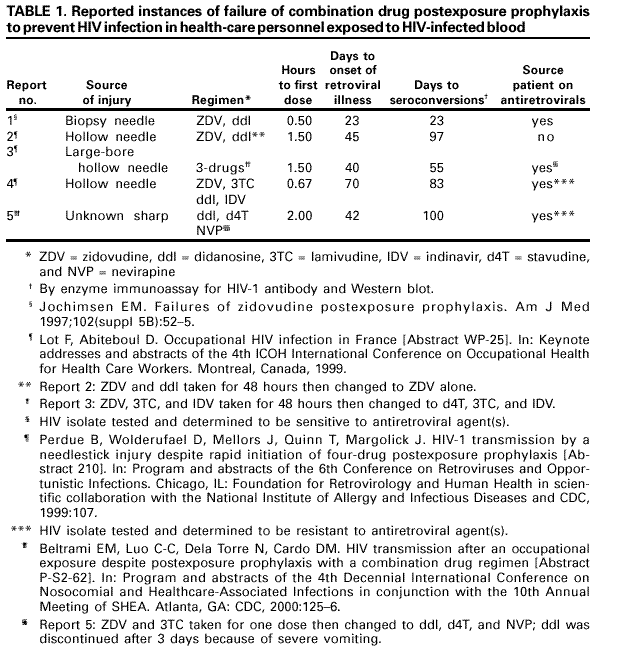
Zidovudine Alone Is Not Recommended Prophylaxis
EDITORGamester et al found that only 34% of students visiting a country with a high prevalence of HIV purchased zidovudine, probably because of the cost . They recommended that medical schools should consider paying for the drug.1
However, zidovudine alone is no longer the standard postexposure prophylaxis. United Kingdom guidelines now state that healthcare workers with high risk exposure to HIV should be advised to take a combination
Also Check: Can You Transmit Hepatitis C
A New Jersey Hospital Could Have Exposed Thousands Of Patients To Hiv And Hepatitis
Thousands of people got a particularly crummy gift this Christmas: A warning that they could have been exposed to dangerous bloodborne diseases like HIV and viral hepatitis while receiving care at the hospital.
On Tuesday, NBC Newsreported that the HealthPlus Surgery Center in Saddle Brook, New Jersey sent letters to more than 3,700 patients who had visited it between January 1st to September 7th. According to the letter, obtained by NBC News, an investigation by the New Jersey Department found that HealthPlus staff often failed to properly sterilize surgical tools between uses or otherwise neglected infection control procedures, raising the risk that patients could have gotten bloodborne infections.
To date, there have not been reports of any infections or illness related to the investigation, the letter says. However, HealthPlus and the New Jersey Department of Health recommend that you get blood tests for hepatitis B, hepatitis C, and HIV.
The need for a test is especially important because allthreediseases often cause no symptoms at first, and acute symptoms can resemble a flu or cold if they appear. But both hepatitis B and C can become chronic silent infections, while HIV infection is currently incurable and only manageable with lifelong antiviral therapy. Untreated chronic hepatitis B and C infection can lead to permanent liver damage, liver failure, and cancer.
How Often Are Major Blood
-
Contributed equally to this work with: Fang Duan, Qiang Huang
Affiliation State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University, Guangzhou, China
-
Contributed equally to this work with: Fang Duan, Qiang Huang
Affiliation State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University, Guangzhou, China
-
Affiliation State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University, Guangzhou, China
-
Affiliation State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University, Guangzhou, China
-
Affiliation State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University, Guangzhou, China
You May Like: How Do You Get Hepatitis B And C
Preventing Hepatitis And Hiv Infections In The Hospital
Isolation precautions create barriers between people and germs. They help prevent the spread of germs in the hospital.
Follow standard precautions with all people.
When you are near or are handling blood, bodily fluids, body tissues, mucous membranes, or areas of open skin, you must use personal protective equipment . Depending on the exposure, you may need:
Oversight In The United States
In the United States, working with primary human tissues requires compliance with Occupational Safety and Health Administrations Bloodborne Pathogens Standard.15 Bloodborne pathogens are defined as infectious microorganisms present in blood that can cause disease in humans and other potentially infectious materials . These pathogens include, but are not limited to, hepatitis B virus, hepatitis C virus, and human immunodeficiency virus. Workers exposed to bloodborne pathogens are at risk for serious or life-threatening illnesses . An overview of the regulatory requirements is outlined in Fig. 1.2 and detailed in the following discussion.
Figure 1.2. Regulatory oversight of research specimens in the United States. This figure outlines the major regulatory oversight involved in the use of the research specimens. In the initial in vitro evaluation stage, the oversight involves the use of biohazardous agents in the laboratory and is regulated by OSHAs Bloodborne Pathogens Standard and biosafety requirements regulated by an organizations biosafety committee. If the specimen is then going to be used in vivo in an animal model, there is additional oversight of the biohazard as ABSL2 and the requirements that the animal procedure be evaluated by the IACUC as defined by the regulatory and oversight bodies listed.
The Bloodborne Pathogens Standard require several actions on the part of the employer. These include:
Catherine M. Keebler, Michael Facik, in, 2008
You May Like: Treatment For Liver Cirrhosis Hepatitis B
Management Of Hcp Living With Hbv
Question: How should institutions provide guidance for HCP living with HBV?
Answer:
1. HCP living with HBV should seek an initial evaluation from a physician who has expertise in HBV management to characterize the serologic and virologic aspects of infection.
2. HCP living with HBV should seek optimal medical management, including, when appropriate, treatment with effective antiviral agents.
3. HCP living with HBV who do not perform category III/exposure-prone procedures should not be prohibited from participating in patient-care activities solely on the basis of their HBV infection.
4. Consonant with the most recent set of guidelines from CDC concerning the management of HCP living with HBV,5 there is no justification for, nor benefit gained from, routine notification of patients with regard to HCP living with HBV who are being managed through the institutions oversight panel.
5. For HCP living with HBV who perform category III/exposure-prone procedures:
a. HCP living with HBV and who, despite appropriate treatment, have circulating viral loads 1,000 IUs should not perform category III/exposure-prone procedures.
b. HCP living with HBV whose circulating viral loads can be consistently suppressed to < 1,000 IUs can perform category III/exposure-prone procedures, as long as the individual
i. Has not been previously identified as having transmitted infection to patients while on appropriate suppressive therapy
Oversight Of Hcp Living With Bloodborne Pathogen
Question: Have expert review panels been effective in providing oversight for HCP living with HBV, HCV, and/or HIV? How should oversight panels be assembled and how should they function?
Answer: The concept of expert review panels assisting in the management of HCP living with bloodborne pathogens was initially described in the now retired 1991 CDC guidelines.2 These guidelines noted the following:
The review panel should include experts who represent a balanced perspective. Such experts might include all of the following: a) the HCWs personal physician, b) an infectious disease specialist with expertise in the epidemiology of HIV and HBV transmission, c) a health professional with expertise in the procedures performed by the HCW, and d) a state or local public health official. If the HCWs practice is institutionally based, the Expert Review Panel might also include a member of the infection control committee, preferably a healthcare epidemiologist. HCWs who perform exposure-prone procedures outside the hospital/institutional setting should seek advice from appropriate state and local public health officials regarding the review process. Panels must recognize the importance of confidentiality and the privacy rights of infected HCWs.2
The 2010 SHEA guidance extended these recommendations as follows:
Recommended Reading: What Is Hepatitis B Virus
Counselling And Behavioural Approaches
Counselling and behavioural interventions offer primary prevention against STIs , as well as against unintended pregnancies. These include:
- comprehensive sexuality education, STI and HIV pre- and post-test counselling
- safer sex/risk-reduction counselling, condom promotion
- STI interventions targeted to key populations, such as sex workers, men who have sex with men and people who inject drugs and
- STI prevention education and counselling tailored to the needs of adolescents.
In addition, counselling can improve peoples ability to recognize the symptoms of STIs and increase the likelihood they will seek care or encourage a sexual partner to do so. Unfortunately, lack of public awareness, lack of training of health workers, and long-standing, widespread stigma around STIs remain barriers to greater and more effective use of these interventions.
What Is The Risk Of Coinfection
A coinfection is when someone has two or more infections at the same time. People living with HIV are at risk of developing coinfections such as hepatitis C because HIV weakens the immune system, which leaves the body more vulnerable to other infections and illnesses.
HIV and HCV are also transmitted in similar ways, which means that people who have HIV may be at higher risk of exposure to HCV. In the United States, over a third of people living with HIV also have hepatitis C.
Coinfection of HCV and HIV is higher among those who use injected drugs. According to the Centers for Disease Control and Prevention , HCV coinfection occurs in between 62 and 80 percent of people with HIV who use injected drugs.
A systematic review of 783 studies concluded that people living with HIV were six times more likely to have hepatitis C than people without HIV.
Hepatitis C infections are more serious in people with HIV and can lead to more severe damage of the liver. HIV and HCV coinfections can increase the risk of:
- liver fibrosis and cirrhosis, which is a buildup of scar tissue in the liver
- end-stage liver disease
A person can contract HCV through direct contact with blood or other body fluids that contain the virus. Possible modes of transmission include:
Ways to prevent hepatitis C include:
- not sharing needles
You May Like: Can You Get Rid Of Hepatitis C