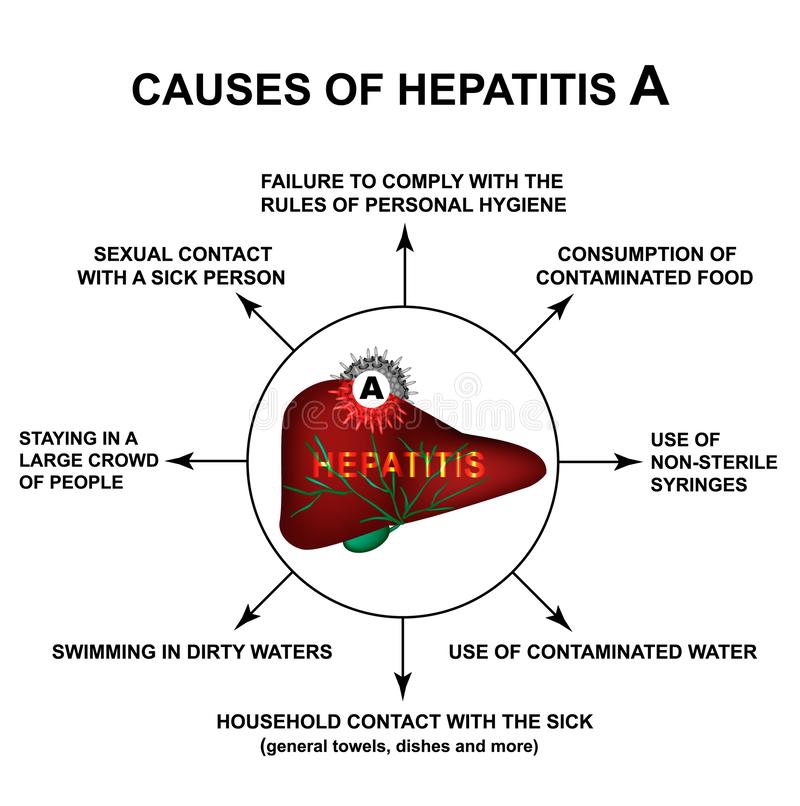
How Is Hepatitis A Spread
Hepatitis A virus is usually spread when a person ingests fecal matter – even in microscopic amounts – from contact with objects, food, or drinks contaminated by feces or stool from an infected person.
Hepatitis A can be spread when:
- An infected person does not wash his or her hands properly after going to the bathroom and then touches objects or food
- A caregiver does not properly wash his or her hands after changing diapers or cleaning up the stool of an infected person
- Someone engages in certain sexual activities, such as oral-anal contact with an infected person
Hepatitis A also can be spread through contaminated food or water. This most often occurs in countries where Hepatitis A is common, especially if personal hygiene or sanitary conditions are poor. Contamination of food can happen at any point: growing, harvesting, processing, handling, and even after cooking.
How Do Doctors Diagnose Hepatitis A
Doctors diagnose hepatitis A based on symptoms and a blood test. A health care professional will take a blood sample from you and send the sample to a lab. A blood test will detect antibodies to the hepatitis A virus called immunoglobulin M antibodies and show whether you have acute hepatitis A. If the blood test finds antibodies to the hepatitis A virus that are not IgM antibodies, then you are immune to hepatitis A, due to either past hepatitis A infection or hepatitis A vaccination.
Whats The Best Way To Stop The Spread Of Hepatitis A
Hepatitis A vaccination is the best way to prevent hepatitis A. The hepatitis A vaccine is given in 2 doses, usually about 6 months apart.
Other ways to stop the spread of HAV are:
- Always washing your hands with soap and warm water immediately after using the bathroom or changing a diaper
- Always washing your hands with soap and warm water before preparing or eating food
Also Check: Can Hepatitis C Come Back
What Is Viral Hepatitis
Hepatitis means inflammation of the liver. The liver is a vital organ that processes nutrients, filters the blood, and fights infections. When the liver is inflamed or damaged, its function can be affected. Heavy alcohol use, toxins, some medications, and certain medical conditions can cause hepatitis. However, hepatitis is often caused by a virus. In the United States, the most common types of viral hepatitis are hepatitis A, hepatitis B, and hepatitis C.
How Is Viral Hepatitis Diagnosed
Diagnosis of viral hepatitis is based on symptoms and physical findings as well as blood tests for liver enzymes, viral antibodies, and viral genetic materials.
Symptoms and physical findings
Diagnosis of acute viral hepatitis often is easy, but the diagnosis of chronic hepatitis can be difficult. When a patient reports symptoms of fatigue, nausea, abdominal pain, darkening of urine, and then develops jaundice, the diagnosis of acute viral hepatitis is likely and can be confirmed by blood tests. On the other hand, patients with chronic hepatitis due to HBV and HCV often have no symptoms or only mild nonspecific symptoms such as chronic fatigue. Typically, these patients do not have jaundice until the liver damage is far advanced. Therefore, these patients can remain undiagnosed for years to decades.
Blood tests
There are three types of blood tests for evaluating patients with hepatitis: liver enzymes, antibodies to the hepatitis viruses, and viral proteins or genetic material .
Liver enzymes: Among the most sensitive and widely used blood tests for evaluating patients with hepatitis are liver enzymes, called aminotransferases. They include aspartate aminotransferase and alanine aminotransferase . These enzymes normally are contained within liver cells. If the liver is injured , the liver cells spill the enzymes into the blood, raising the enzyme levels in the blood and signaling that the liver is damaged.
Examples of tests for viral antibodies are:
Don’t Miss: Chronic Hep C Without Hepatic Coma Icd 10
Treatment And Prevention Of Hepatitis A
Because hepatitis A virus infections can have serious health consequences, the Centers for Disease Control and Prevention recommends providing post-exposure prophylaxis for unvaccinated people who have consumed any contaminated food or water within two weeks of exposure.
PEP consists of:
- Hepatitis A vaccine for people between the ages of 1 and 40 years
- Hepatitis A virus-specific immunoglobulin for people outside of this age range, but the hepatitis A vaccine can be substituted if IG is not available.
- Those with evidence of previous vaccination or who can confirm previous hepatitis A illness do not require PEP.
If you are unsure if you have been vaccinated against hepatitis A, contact your health professional to check your immunization records. If you have been vaccinated, no further action is needed. If you have never received the hepatitis A vaccine, getting a single dose within two weeks of exposure can protect against illness. If you are unable to determine whether you have already been vaccinated, receiving an additional dose of vaccine is not harmful if you have already been vaccinated.
Multiple Cases Of Hepatitis Reported After Shots
The Journal of Hepatology paper noted that seven additional cases of suspected immune-mediated hepatitis have been reported following COVID-19 shots, including both Pfizers and Modernas.
They hope to raise awareness so that vaccination centers will routinely check for signs of immune-mediated hepatitis prior to administering second doses and state, Long-term follow up of identified individuals will be essential in determining the prognosis of this immune-mediated liver injury.5
In a separate letter to the editor, published in the Journal of Hepatology in June 2021, researchers again raised concerns that COVID-19 shots could cause hepatitis. In this case, a 56-year-old woman developed severe autoimmune hepatitis following her first dose of Modernas COVID-19 shot.6
Prior to this, in April 2021, researchers also described a case of autoimmune hepatitis that developed after a COVID-19 shot, this time in a 35-year-old woman who was three months postpartum. In autoimmune hepatitis, the bodys immune system mistakenly attacks the liver, causing inflammation and damage, and its possible the shot triggered the autoimmunity via spike-directed antibodies:7
To our knowledge, this is the first reported episode of autoimmune hepatitis developing post-COVID-19 vaccination, raising concern regarding the possibility of vaccine-induced autoimmunity. As causality cannot be proven, it is possible that this association is just coincidental.
You May Like: How Do You Know If You Get Hepatitis C
How Do Doctors Treat Hepatitis A
Treatment includes resting, drinking plenty of liquids, and eating healthy foods to help relieve symptoms. Your doctor may also suggest medicines to help relieve symptoms.
Talk with your doctor before taking any prescription or over-the-counter medicines, vitamins or other dietary supplements, or complementary or alternative medicinesany of these could damage your liver. You should avoid alcohol until your doctor tells you that you have completely recovered from hepatitis A.
See your doctor regularly to make sure your body has fully recovered. If you have symptoms for longer than 6 months, see your doctor again.
What Are The Symptoms Of Hepatitis A
Symptoms of hepatitis A may include:
- Stomach pain, vomiting, loss of appetite.
- Diarrhea, stools that are light in color .
- Jaundice, which means that skin and eyes are yellow. This happens primarily to older children and adults. Kids younger than 6 years old do not generally have jaundice.
- Urine that is dark yellow in color.
Read Also: Is Hepatitis B And C Curable
Undercooked And Raw Shellfish
Shellfish are animals that filter the water from their surroundings. Because of this, they can become contaminated with hepatitis A virus if they are grown in polluted waters. To be safe, cook shellfish thoroughly before eating it. Undercooked shellfish like oysters, mussels, and clams may harbor and transmit hepatitis A. You may prefer the taste of raw oysters, but cooked shellfish really is safer. Protect your health and skip the raw oyster bar.
What Does The Government Do To Protect Me
In Canada, several government organizations work together every day to keep your food safe:
- Health Canada makes food safety standards and policies to help minimize the risk of foodborne illnesses.
- The Canadian Food Inspection Agency enforces these policies and standards and carries out inspections to make sure the food industry meets its food safety responsibilities. The CFIA works with Health Canada to make sure that foodborne illness is detected early and warnings go out to the public quickly.
- The Public Health Agency of Canada studies the incidence and causes of diseases in Canada, conducts outbreak surveillance, and coordinates outbreak response.
The Government of Canada works very hard to protect your health and safety:
- We are carrying out a five-year Food and Consumer Safety Action Plan, to strengthen and modernize Canada’s safety system and make sure you can have confidence in the quality and safety of the food, health and consumer products you buy.
- We are investing $75 million more in Canada’s food safety system to hire more inspectors, update lab technology, and improve communication with Canadians.
- We support and participate in public awareness campaigns about safe food practices, like the Canadian Partnership for Consumer Food Safety Education’s Be Food Safe program, which encourages Canadian consumers to think of food safety at every step of the food handling process, from shopping for groceries to re-heating leftovers.
Recommended Reading: Can You Get Hepatitis C From Kissing
How Common Is Hepatitis A
In the United States, hepatitis A has become relatively uncommon. After the hepatitis A vaccine became available in 1995, the rate of hepatitis A infections declined by 95 percent in the United States. The number of reported cases of hepatitis A fell to 1,239 in 2014, the lowest yearly number of cases reported since the disease could be tracked.1 However, the number of reported cases increased to 3,366 in 2017, almost 3 times higher, mostly due to outbreaks among people who use drugs and people experiencing homelessness.1 Early reports suggest that the numbers of cases and outbreaks of hepatitis A increased further during 2018 and continue at these higher rates in 2019.2
Hepatitis A is more common in developing countries where sanitation is poor and access to clean water is limited. Hepatitis A is more common in parts of Africa, Asia, Central and South America, and Eastern Europe than it is in the United States.
Who Is At Risk Of Hepatitis A
Anyone can get hepatitis A if they have not beenvaccinated. In the U.S., you are at a higher risk if you:
- Use illegal drugs, whether injected or not
- Live with someone who has hepatitis A
- Have bleeding problems and take clotting factors
- Have oral-anal sexual contact with someone who has hepatitis A
- Travel to areas that have high rates of hepatitis A
Travel to Africa, Asia, Eastern Europe,or Central and South America,including Mexico, increases the riskof getting hepatitis A.
You May Like: How Do You Get Hepatitis B
How Is Hepatitis A Diagnosed And Treated
A doctor can determine if a person has Hepatitis A by discussing his or her symptoms and taking a blood sample. To treat Hepatitis A, doctors usually recommend rest, adequate nutrition, fluids, and medical monitoring. Some people will need to be hospitalized. It can take a few months before people begin to feel better.
How Is It Spread
Hepatitis A is spread when a person ingests fecal mattereven in microscopic amountsfrom contact with objects, food, or drinks contaminated by feces or stool from an infected person.
Hepatitis B is primarily spread when blood, semen, or certain other body fluids- even in microscopic amounts from a person infected with the hepatitis B virus enters the body of someone who is not infected. The hepatitis B virus can also be transmitted from:
- Birth to an infected mother
- Sex with an infected person
- Sharing equipment that has been contaminated with blood from an infected person, such as needles, syringes, and even medical equipment, such as glucose monitors
- Sharing personal items such as toothbrushes or razors
- Poor infection control has resulted in outbreaks in health care facilities
Hepatitis C is spread when blood from a person infected with the Hepatitis C virus even in microscopic amounts enters the body of someone who is not infected. The hepatitis C virus can also be transmitted from:
- Sharing equipment that has been contaminated with blood from an infected person, such as needles and syringes
- Receiving a blood transfusion or organ transplant before 1992
- Poor infection control has resulted in outbreaks in health care facilities
- Birth to an infected mother
Also Check: How Common Is Hepatitis C
How Can You Prevent Hepatitis A
There is a vaccine, made from an inactivateddeadvirus to prevent hepatitis A. If you are not sure you have had the vaccine, you can ask your doctor to test you to see if you have been vaccinated.
You can also practice good hand washing hygiene. Make sure you use soap and warm water to wash your hands for at least 15 to 30 seconds after you use the toilet, change diapers, and before and after touching food.
If you are traveling in another country, especially a developing country, drink only bottled water and use only bottled water to brush your teeth, wash your produce, and freeze for ice cubes.
Common Symptoms Of Hepatitis
If you are living with a chronic form of hepatitis, like hepatitis B and C, you may not show symptoms until the damage affects liver function. By contrast, people with acute hepatitis may present with symptoms shortly after contracting a hepatitis virus.
Common symptoms of infectious hepatitis include:
It is crucial to understand what is causing hepatitis in order to treat it correctly. Doctors will progress through a series of tests to accurately diagnose your condition.
Also Check: Hepatitis B Surface Antibody Positive
How Do People Get Hepatitis A
Hepatitis A virus is found in the stool of people with HAV infection. It enters the body through the mouth after someone handles something contaminated with HAV, or eats or drinks something contaminated with HAV.
People usually get hepatitis A by having close contact with a person who is infected, from food or drinks prepared by someone who is infected, or by eating shellfish harvested from sewage-contaminated water. After the virus enters the body, there is an incubation period lasting 2 to 7 weeks until illness begins.
Can Hepatitis A Be Prevented
Yes. The hepatitis A vaccine is recommended for all children over 1 year old. The vaccine is given at 12 months of age, followed by a second dose at least 6 months later. Having many young kids vaccinated against HAV can limit the spread of the disease in a community.
The vaccine can be given as early as 6 months of age to babies who will travel to a place where hepatitis A is common .
The vaccine also is recommended for older kids, teens, and adults who have never gotten it.
The best way to prevent hepatitis A and many other infections is to wash hands well and often. This is especially important after using the toilet and before eating or preparing food.
Don’t Miss: How Do You Get Hepatitis A
What Are The Symptoms And Signs Of Viral Hepatitis
The period of time between exposure to hepatitis and the onset of the illness is called the incubation period. The incubation period varies depending on the specific hepatitis virus. Hepatitis A virus has an incubation period of about 15 to 45 days Hepatitis B virus from 45 to 160 days, and Hepatitis C virus from about 2 weeks to 6 months.
Many patients infected with HAV, HBV, and HCV have few or no symptoms of illness. For those who do develop symptoms of viral hepatitis, the most common are flu-like symptoms including:
Who Is At Risk Of Getting Hepatitis A

Hepatitis A is usually spread from person to person, making it highly contagious. However, certain factors can increase your risk of contracting it, including:
- living in an area where hepatitis A is common, including most countries with low sanitation standards or a lack of safe water
- injecting or using illegal drugs
- living in the same household as someone who is hepatitis A-positive
- having sexual activity with someone who is hepatitis A-positive
- being HIV-positive
Don’t Miss: How Do You Catch Hepatitis B And C
What Is The Treatment For Viral Hepatitis
Treatment of acute viral hepatitis and chronic viral hepatitis are different. Treatment of acute viral hepatitis involves resting, relieving symptoms, and maintaining an adequate intake of fluids. Treatment of chronic viral hepatitis involves medications to eradicate the virus and taking measures to prevent further liver damage.
Acute hepatitis
In patients with acute viral hepatitis, the initial treatment consists of relieving the symptoms of nausea, vomiting, and abdominal pain . Careful attention should be given to medications or compounds, which can have adverse effects in patients with abnormal liver function . Only those medications that are considered necessary should be administered since the impaired liver is not able to eliminate drugs normally, and drugs may accumulate in the blood and reach toxic levels. Moreover, sedatives and “tranquilizers” are avoided because they may accentuate the effects of liver failure on the brain and cause lethargy and coma. The patient must abstain from drinking alcohol since alcohol is toxic to the liver. It occasionally is necessary to provide intravenous fluids to prevent dehydration caused by vomiting. Patients with severe nausea and/or vomiting may need to be hospitalized for treatment and intravenous fluids.
Chronic hepatitis
Medications for chronic hepatitis C infection include:
- oral daclatasvir
Medications for chronic hepatitis B infection include:
- oral entecavir
- oral tenofovir
Fulminant hepatitis