What Is Hepatitis C
Hepatitis C is an inflammation of the liver caused by a specific virus called the hepatitis C virus . The word “hepatitis” is derived from two Latin segments: “hepat” refers to the liver, and “itis” meaning inflammation. The term “hepatitis” is not specific for a particular cause of the inflammation, as hepatitis can be caused by reactions to medications, toxic drugs, poisons, alcohol, allergic reactions, autoimmune diseases and a variety of viruses. The most common viruses that specifically cause hepatitis include
- hepatitis B virus, and
- hepatitis C virus.
Other hepatitis viruses also exist and cause a small number of infections. Additionally, other viruses can cause hepatitis even though they are not specifically “hepatitis viruses.” These most commonly include Epstein Barr Virus , the cause of mononucleosis, and cytomegalovirus , which causes a variety of illnesses in different parts of the body, especially in patients whose immune function is depressed due to steroids, chemotherapy for cancer, and HIV/AIDS.
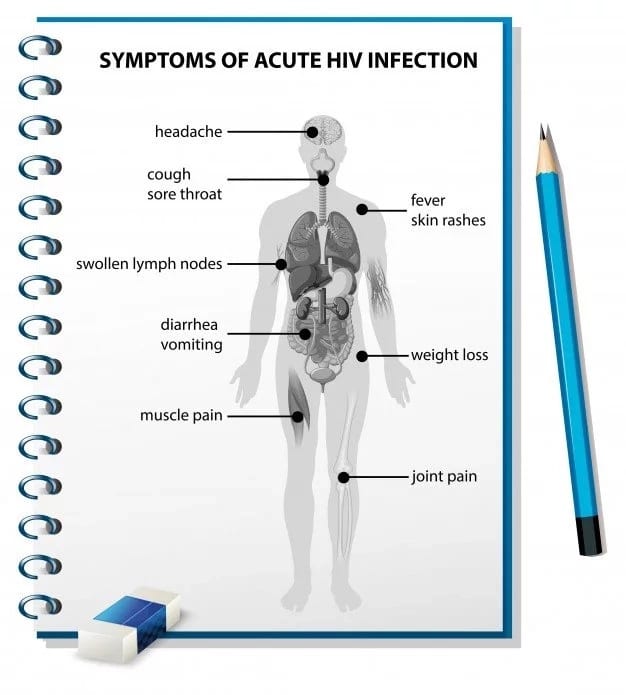
There are two stages of hepatitis C. The acute phase occurs soon after infection. Most people have no symptoms at this stage. Roughly 75% – 85% of individuals infected go on to develop a chronic infection. At this second, chronic stage, there may be no symptoms for years or decades. Eventually, if left untreated, most people with chronic hepatitis C will become symptomatic with progressive liver disease.
- Generalized abdominal pain
Can I Drink Alcohol Once In A While If I Have Hepatitis C
Alcohol can clearly contribute to worsening liver disease. You must discuss with your health care provider if any amount of alcohol is safe for you.
Alcohol can cause inflammation and scarring in the liver. If you have any underlying liver condition, such as hepatitis C or hepatitis B or damage from long-term alcohol use, your liver will be more sensitive to alcohol. When you have hepatitis C virus, alcohol on top of the hepatitis C can cause the inflammation and scarring to be worse, and overall damage to the liver may happen much faster when you drink alcohol.
Here is some helpful information about alcohol and hepatitis:
Who Should Get Tested
You should consider getting tested for hepatitis C if you’re worried you could have been infected or you fall into one of the groups at an increased risk of being infected.
- Hepatitis C often has no symptoms, so you may still be infected if you feel healthy.
- The following groups of people are at an increased risk of hepatitis C:
- ex-drug users and current drug users, particularly users of injected drugs
- people who received blood transfusions before September 1991
- recipients of organ or tissue transplants before 1992
- people who have lived or had medical treatment in an area where hepatitis C is common high risk areas include North Africa, the Middle East and Central and East Asia
- babies and children whose mothers have hepatitis C
- anyone accidentally exposed to the virus, such as health workers
- people who have received a tattoo or piercing where equipment may not have been properly sterilised
- sexual partners of people with hepatitis C
If you continue to engage in high-risk activities, such as injecting drugs frequently, regular testing may be recommended. Your doctor will be able to advise you about this.
Read Also: Different Types Of Hepatitis C
Do I Have The Symptoms Of Hepatitis C
Hep C usually shows up first in routine bloodwork since many people have no symptoms at all. In fact, because hep C can remain dormant for so longit takes 10 to 40 years to progress from mild disease to cirrhosis, liver failure or liver cancerthe Centers for Disease Control and Prevention is now recommending a one-time screening blood test for anyone born between 1945 and 1965 since this population is more at risk of having received a tainted blood transfusion.
In the meantime, it’s crucial to know what the symptoms of hepatitis c cirrhosis are. They include:
Taking action quickly if you have any of these symptoms is crucial. The liver, which is the second-largest organ has a big job, or rather jobs, including producing most of the protein we need, breaking down nutrients from food to produce energy, preventing nutrient shortages by storing certain vitamins, minerals and sugar, producing bile, which helps digest fat and absorb vitamins A, D, E and K, and fighting infection by removing bacteria from the blood.
Blood Donations Before September 1991

Since September 1991, all blood donated in the UK is checked for the hepatitis C virus.
There’s a small chance you may have been infected with hepatitis C if:
- you received a blood transfusion or blood products before September 1991
- you received an organ transplant before 1992
Before 1992 donated organs were not routinely screened for hepatitis C and there is a very small risk a donated organ from someone with hepatitis C could spread the infection.
There are blood tests to check for hepatitis C infection
Also Check: Low Protein Diet For Hepatic Encephalopathy
I I Have Liver Disease Or Cirrhosis Of The Liver Will This Make Me More At Risk With Covid
If you have cirrhosis of the liver there is no evidence that you have a higher chance of catching COVID.
Having cirrhosis of the liver can increase the risk of severe illness if you have COVID.
If you have elevated liver enzymes or abnormal liver function test as a result of liver disease, you may also be at risk of severe illness if you have COVID.
For these reasons, its best to take all necessary precautions to keep yourself safe from COVID by following government and medical recommendations.
Everyone with cirrhosis should see their liver specialist regularly. Call and speak to your specialist about what is best for your health.
How Common Is Hepatitis C
There are approximately 30,000 new cases of acute hepatitis C every year in the United States as estimated by the CDC. In 2015, it was estimated that approximately 3.5 million Americans were infected with hepatitis C.
On a global scale, the prevalence of hepatitis C is greatest in Central and East Asia, North Africa, and the Middle East. In 2016, it was estimated that 177 million people worldwide had antibodies to hepatitis C virus.
- exposure to other people who do or might have hepatitis C.
Recommended Reading: Can You Cure Hepatitis B
Is It Safe To Take Aspirin Or Tylenol If I Have Hepatitis C
Tylenol is an over-the-counter pain killer. It can be harmful in high doses. If you have hepatitis or liver disease, then you can take Tylenol, but no more than 2,000 mg total over 24 hours. In general, this could be one 500 mg tablet every 6 hours, at the most. Acetaminophen is also included as an ingredient in some opiate medications and in some over-the-counter cold/flu medications, so please be aware of the dose of acetaminophen you may be taking from some combination medicines.
Aspirin, ibuprofen , naproxen , and other nonsteroidal anti-inflammatory drugs , can be harmful if you have cirrhosis. They are safe in hepatitis patients who do not have cirrhosis. But, if a patient has cirrhosis, then NSAIDs cannot be taken at all. If you are not sure, always check with your provider.
How Is Hepatitis C Infection Prevented
Unfortunately, there is no vaccine to prevent hepatitis C. To reduce your risk of getting hepatitis C:
- Injection drug use is the most common way people get hepatitis C. Avoid injecting drugs to reduce your risk. If you do inject drugs, use sterile injection equipment. Avoid reusing or sharing.
- Avoid sharing personal care items that might have blood on them
- If you are a health care or public safety worker, follow universal blood/body fluid precautions and safely handle needles and other sharps
- Consider the risks if you are thinking about tattooing, body piercing, or acupuncture are the instruments properly sterilized?
- If youre having sex with more than one partner, use latex condoms correctly and every time to prevent the spread of sexually transmitted diseases, including hepatitis C.
Recommended Reading: Can You Get Hepatitis C Twice
What Is The Life Expectancy Of Someone With Hep C
People with hepatitis C can live many years after diagnosis, but the range varies. A 2014 study showed that patients infected with hepatitis C virus died on average 15 years sooner than people who did not have the illness. With hepatitis C, the liver becomes seriously damaged due to inflammation.
What makes hep C worse?
Raw oysters or shellfish. They can have bacteria that give you serious infections that are more severe if you have hep C. Fatty, sugary foods. They can stress your liver or lead to fat deposits in it.
I Have Hep C Do I Need Extra Protection Against Covid
No. You can protect yourself against COVID in the same ways as everyone else. We all need be careful to stop the spread of COVID, for our own health and for the health of our communities.
You should take extra care to protect yourself from COVID if you: have an additional health condition are over 70 are over 50 and Aboriginal have a weakened immune system.
Follow Government advice on keeping safe and stopping the spread of COVID
Don’t Miss: How Do They Test For Hepatitis
How Is Hepatitis B Diagnosed
There are three main ways to diagnose HBV infection. They include:
- Blood tests: Tests of the blood serum shows how your bodys immune system is responding to the virus. A blood test can also tell you if you are immune to HBV.
- Abdominal ultrasound: An ultrasound uses sound waves to show the size and shape of your liver and how well the blood flows through it.
- Liver biopsy: A small sample of your liver tissue is removed though a tiny incision and sent to a lab for analysis.
The blood test that is used to diagnose hepatitis B is not a test that you get routinely during a medical visit. Often, people whove become infected first learn they have hepatitis B when they go to donate blood. Blood donations are routinely scanned for the infection.
The virus can be detected within 30 to 60 days of infection. About 70% of adults with hepatitis B develop symptoms, which tend to appear an average of 90 days after initial exposure to the virus.
How Do You Get Hepatitis C
Hepatitis C is only contracted through contact with another person who is infected with the hepatitis C virus . It is not acquired through contact with animals or insects.
Hepatitis C is present primarily in the blood, and to a lesser degree in specific other body fluids, of an infected person. Today, it is passed most commonly through the sharing of used needles by injection drug users. Prior to 1990, it was commonly passed through blood transfusions. However, since 1990, all donated blood is tested for hepatitis C virus, so it is extremely rare for hepatitis C to be acquired through a blood transfusion.
Transmission of hepatitis C occasionally occurs in healthcare settings, such as hospitals and clinics, when established infection control protocols are not followed. Health care professionals who do not follow these protocols can become infected if they sustain a needle stick from a patient who carries hepatitis C virus.
While uncommon, one mode of transmission is through organ transplantation when the donated organ comes from a person who carries the hepatitis C virus. The use of HCV-positive organs is currently reserved for the most serious cases requiring transplantation.
How Does Hepatitis C Spread?
Tattooing and body piercing have been documented to transmit the hepatitis C virus when recommended sterilization and infection control procedures are not followed.
Also Check: What Are The Signs Of Hepatitis C In Females
Are There Supplements That Are Bad For My Liver
Taking too many vitamin and mineral supplements may do more harm than good to a damaged liver.
What Laboratory Tests Diagnose Hepatitis C
Laboratory blood tests will be done to evaluate the patient’s liver function and to look for hepatitis C antibodies . If these tests indicate that the person has hepatitis C, a hepatitis C “viral load” test will be done. This looks for genetic material from the hepatitis C virus and measures the quantity of hepatitis C virus that is circulating in the patient’s blood. This is helpful in determining if treatment is appropriate and to monitor the success of the treatment .
Individuals who had hepatitis C in the past and cleared the virus on their own will have a positive HCV antibody test, but there will be no hepatitis C virus genetic material in the blood. If a person is immunosuppressed due to an immunological condition, cancer chemotherapy, immunotherapy or HIV/AIDS, the test results may be different and need to be evaluated accordingly.
You May Like: How Do You Get Hepatitis From Food
What Foods Should I Avoid
Everyone should avoid eating a lot of fat, cholesterol, salt and processed sugar, even if their liver is healthy. In addition, those with HCV should limit or avoid alcohol. Drinking alcohol will speed up liver damage.
Eating properly can help decrease some of the symptoms of Hepatitis C, like feeling tired and sick. Drink lots of water for general health benefits. HCV is not a digestive disease diet will not affect the disease. Your provider may put you on a special diet if you have advanced liver disease.
What Causes Hepatitis C
Hepatitis C is caused by infection with the hepatitis C virus. The virus is spread from person to person through contact with blood. People who use intravenous drugs can get hepatitis C when they share needles with someone who has the virus. Health care workers can be exposed to hepatitis C. They can become infected if they are accidentally stuck with a needle that was used on an infected patient. You are also at a higher risk if you got a blood transfusion or an organ transplant before 1992.
Hepatitis C cant be spread unless a person has direct contact with infected blood. This means a person who has hepatitis C cannot pass the virus to others through casual contact such as:
- using public toilets
- touching doorknobs
Also Check: Can I Donate Plasma If I Had Hepatitis B
New Jersey Senior Care News
Hepatitis C is the number one cause for liver transplants. It is five times more prevalent in the United States than HIV/AIDS and kills about 10,000 Americans annually.
It puts patients at risk for cirrhosis of the liver as well as liver cancer. It can be a relatively silent disease, as many people have no symptoms for years after contracting the virus. In many cases, these are people who are in their 50s and 60s, who often learn of their illness through a routine blood test and are shocked to hear they have the disease.
Primary risk factors for Hepatitis C include use of intravenous drugs , promiscuous sex, blood transfusions, and exposure to tainted blood.
The good news is that recent advances in treatment have dramatically improved the success rate in eradicating the Hepatitis C virus from 50% to 80%. The old standard of care has taken a major leap forward by adding directly acting antiviral agents called DAAs. The new medication, called Incivek, is given for 12 weeks with the old treatment , with the old treatment then continued for 36 more weeks. Incivek, which received FDA earlier this year, is taken in pill form.
What Are The Recommendations For Follow
Anti-viral agents or immune globulin should not be used for postexposure prophylaxis.
For the source, baseline testing for anti-HCV.
For the person exposed to an HCV-positive source, baseline and follow-up testing including baseline testing for anti-HCV and ALT activity and follow-up testing for anti-HCV and ALT activity.
Recommended Reading: Is Hepatitis C Contagious Sexually
What Other Tests Diagnose Hepatitis C
Once the diagnosis of hepatitis C is established, other tests may be done to determine whether the patient has developed liver fibrosis or scarring . This can be done with a needle biopsy of the liver, and examining the biopsied liver tissue under the microscope. Liver biopsy is less commonly done today because noninvasive tests are more readily available, more easily accomplished and less costly.
Liver imaging can evaluate fibrosis using ultrasound and MRI scans. Additionally, calculations using a variety of blood tests also can predict the degree of inflammation and fibrosis present. Genotype testing will typically be done to determine what subtype of hepatitis C the patient has, as this will impact what drugs are used for treatment.
Testing for other infections including HIV, hepatitis A, and hepatitis B is typically done to determine if the patient might have other conditions that could impact patient’s treatment and prognosis.
With the newest forms of antiviral treatment, the most common types of chronic hepatitis C can be cured in most individuals.
How Is Hepatitis B Treated
Your healthcare provider will treat you based on what type of hepatitis B you have, acute or chronic.
Acute hepatitis B infections
If you develop an acute form of the condition, you probably wont need medical treatment. Instead, your doctor will likely suggest that you get plenty of rest, drink lots of fluids and maintain a healthy diet to support your body as it fights off the infection.
Chronic hepatitis B infections
If you have chronic hepatitis B, you might be a candidate for drug therapy. Usually, drug therapy is used only if you have active liver disease. There are seven drugs that are approved by the U.S. Food and Drug Administration to treat hepatitis B. Two are injectable forms of interferon, while the five other antivirals are tablets.
You will need to take these medications every day. They help by slowing the viruss ability to multiply in your system. This helps reduce swelling and liver damage. Youll need to be regularly monitored for early signs of liver damage and liver cancer. Your healthcare provider will want to see you once or twice a year.
Don’t Miss: Hepatitis B Vaccine For Newborns