For Defining The Prognosis Or Inferring The Clinical Features And Behavior Of Aih
Patients with anti-LKM1 reactivity are usually younger than patients with other autoantibody profiles, and patients with anti-SepSecS or with isolated ANA reactivity tend to be older . AIH-2 is usually more aggressive, and acute liver failure is more common in these patients. Patients with AIH-2 exhibited an IgA deficiency more frequently on the other hand, the levels of gamma globulin and IgG are considerably higher in patients with anti-microfilament and anti-SepSecS antibodies than in patients with anti-LKM1 .
Patients with anti-LC1, anti-SepSecS, and anti-F-actin antibodies have a worse prognosis than their counterparts with isolated ANAs in which the response to treatment is much better than in patients with other serological markers . Those who remain reactive to anti-F-actin greater than 1/40 and to ASMA greater than 1/80 after treatment usually have histological activity . Patients with reactivity for anti-SepSecS have relapses more frequently than other patients after treatment withdrawal. However, the prognostic implications ascribed to these antibodies could also be related to anti-Ro52 reactivity due to the almost invariable concomitance of these two types of autoantibodies .
Where Can You Find Asmas
âSmooth muscle antibodies can be found with medical conditions like:â
- Rheumatic disordersâ
The most common target of ASMAs is smooth muscle tissues in the liver, leading to diseases like autoimmune hepatitis and primary biliary cirrhosis.
When diagnosed early, autoimmune hepatitis can be treated by using immunosuppressive drugs. Without treatment, it may lead to liver failure.
Though autoimmune hepatitis can occur in any population, it is more common in women.
What Is A Smooth Muscle Antibody Test
This test looks for smooth muscle antibodies in the blood. A smooth muscle antibody is a type of antibody known as an autoantibody. Normally, your immune system makes antibodies to attack foreign substances like viruses and bacteria. An autoantibody attacks the body’s own cells and tissues by mistake. SMAs attack smooth muscle tissues in the liver and other parts of the body.
If SMAs are found in your blood, it is likely you have autoimmune hepatitis. Autoimmune hepatitis is a disease in which the immune system attacks liver tissues. There are two types of autoimmune hepatitis:
- Type 1, the most common form of the disease. Type 1 affects more women than men. It is also more common in people who also have another autoimmune disorder.
- Type 2, a less common form of the disease. Type 2 mostly affects girls between the ages of 2 and 14.
Autoimmune hepatitis can be managed with medicines that suppress the immune system. Treatment is more effective when the disorder is found early. Without treatment, autoimmune hepatitis can cause serious health problems, including cirrhosis and liver failure.
Other names: anti-smooth muscle antibody, ASMA, actin antibody, ACTA
Recommended Reading: What Does Chronic Hepatitis C Mean
Can I Have More Than One Cause Of Hepatitis
Yes. For instance, autoimmune hepatitis can co-exist with a viral hepatitis, such as hepatitis B or hepatitis C, and can be exacerbated by liver damage caused by alcohol abuse. Since the treatment of hepatitis depends on the cause, it is very important that your healthcare practitioner understand the underlying cause of your condition.
Type 1 Autoimmune Hepatitis
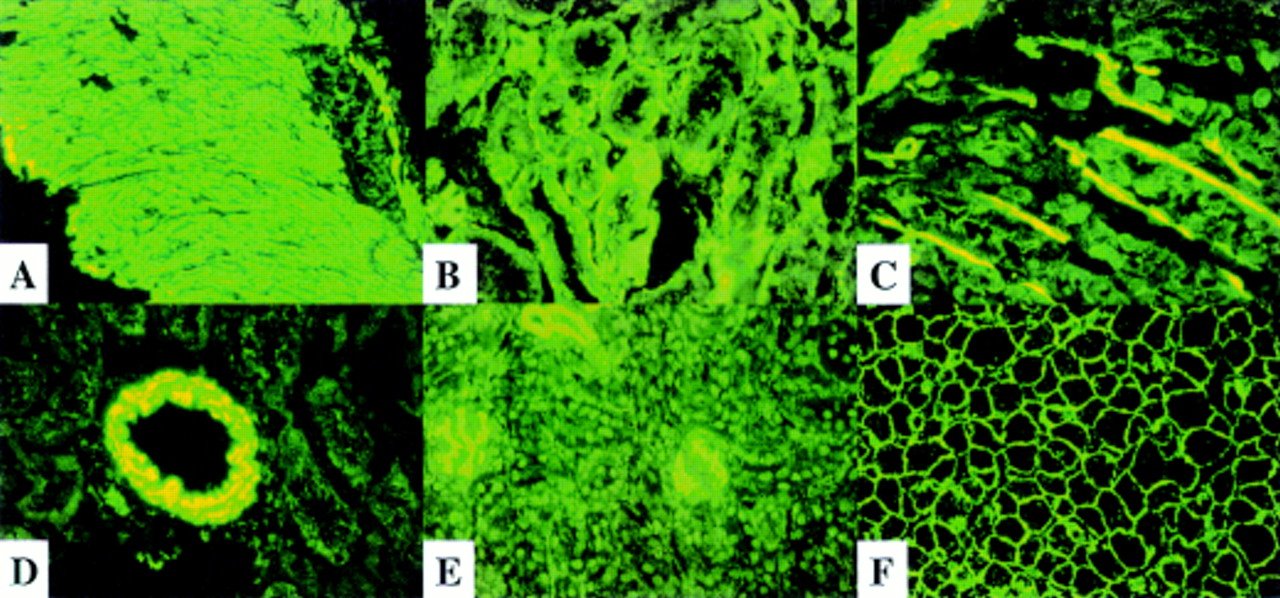
Type 1 AIH is characterized by SMA, ANA, or both .1,7 Antibodies to actin have greater specificity, but less sensitivity, for the diagnosis of AIH than SMA.6 Atypical pANCA are found in as many as 90% of patients with type 1 AIH and typically are absent in type 2 AIH.6,7
Type 1 AIH can occur at any age and in either gender .7 Initial studies that suggested a bimodal age distribution probably reflected referral biases to tertiary medical centers. The disease has been described in infants and probably is underdiagnosed in the elderly.32 Seventy-eight percent of patients are women , and 38% have concurrent extrahepatic immunologic diseases.7 Autoimmune thyroiditis , Graves disease , and ulcerative colitis are the most common associated immune disorders. Rheumatoid arthritis, pernicious anemia, scleroderma, Coombs-positive hemolytic anemia, autoimmune thrombocytopenic purpura, symptomatic cryoglobulinemia, leukocytoclastic vasculitis, nephritis, erythema nodosum, systemic lupus erythematosus, and fibrosing alveolitis also may occur . Cholangiography is warranted to exclude PSC in all patients who have concurrent ulcerative colitis .33
Albert J. Czaja MD, FACP, FACG, AGAF, in, 2012
Read Also: Common Signs Of Hepatitis C
Diagnostic Autoantibodies For Autoimmune Hepatitis
Codified criteria for the diagnosis of autoimmune hepatitis have been developed by the International Autoimmune Hepatitis group.6 The criteria comprise compatible liver histopathology including interphase hepatitis, elevated serum IgG, liver autoantibodies, elevated serum transaminases and negative serology for viral hepatitis. Interphase hepatitis is characterised by lymphocytic infiltration with or without plasma cells with associated hepatocyte cell death at parenchymal-connective tissue junctions around portal tracts.
What Does A Positive Smooth Muscle Antibody Test Mean
Normally, very little to no ASMAs are found in your blood.
If your blood test shows a high amount of ASMAs, you may have autoimmune hepatitis. It means that your immune system is attacking healthy cells in your liver using autoantibodies.
âYour doctor will order a biopsy to confirm the diagnosis of autoimmune hepatitis.
Also Check: Hepatitis C What Does It Do
Serological Markers And Liver Histopathology
Serum autoantibodies, including antinuclear antibody , smooth muscle antibody and antimitochondrial antibody were tested using indirect immunofluorescence with the standard methods , and sera were considered to be positive when they produced a reaction at a dilution of 1:100. Immunoglobulin assay were taken with the mothod of immunological turbidimetry . The normalized levels of IgG, IgM and IgA were respectively 7.23-16.6 g/L, 0.63-2.77 g/L and 0.69-3.82 g/L.
Biochemical profiles, including alanine transarninase , aspartate aminotransferase , total bilirubin , gamma glutamyl transferase and alkaline phosphatase were measured using standard laboratory procedure. The normalized levels of ALT, AST, TBil, GGT and ALP were respectively < 40 U/L, < 40 U/L, < 17.1 umol/L, 7-32 U/L, and 40-150 U/L.
Liver biopsy was performed in some cases for definite diagnosis, and biopsy specimens were examined in the Pathology Department.
When To Start Treatment
Treatment should be started in patients with significant disease, characterized by at least one of the following: AST or ALT > 10 times the upper limit of normal AST or ALT > 5 times the upper limit of normal and IgG > 2 times the upper limit of normal bridging necrosis or multiacinar necrosis on histology. Although uncommon, the presence of incapacitating symptoms has also been proposed as an indication of treatment regardless of laboratory values.
In asymptomatic patients with AST, ALT, and gamma globulins/IgG elevations that do not meet the criteria above, the benefit of treatment is less clear. The course of the disease in such patients has not been well established and there is little data to support treatment. Thus in asymptomatic patients with only mild laboratory and histological changes, the decision to start treatment should be individualized and the risks of therapy taken into account. Often treatment in this situation can be postponed and liver tests followed closely. Such patients should always be referred to a hepatologist or gastroenterologist for decision regarding therapy.
Asymptomatic patients with inactive disease on liver biopsy or burned out cirrhosis do not benefit from treatment.
Read Also: If You Have Hepatitis C Can You Donate Plasma
Genetics And Predisposing Factors
Autoimmune hepatitis is thought to result from an environmental trigger in a genetically predisposed individual, leading to loss of tolerance of T lymphocytes with subsequent hepatocyte attack.
It is a polygenic disease and does not follow a Mendelian distribution. Therefore there is no need to screen family members of patients with AIH. There is a strong genetic association with the alleles of the major histocompatibility complex class II. The presence of human leukocyte antigen genes HLA DRB1*03 and HLA DRB1*04 predisposes to AIH type 1 and affect the disease course and response to treatment. Individuals who are positive for HLA DRB1*03 are younger, respond less favorably to corticosteroid therapy, and progress more often to liver failure. On the other hand, the presence of HLA DRB1*04 is associated with higher rates of concomitant autoimmune disorders.
Autoimmune hepatitis can also be associated with autoimmune polyendocrinopathy candidiasis ectodermal dystrophy syndrome, an autosomal recessive disease characterized by hypoparathyroidism, adrenal insufficiency, and chronic mucocutaneous candidiasis. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy is the only AIH-associated disease that follows a Mendelian pattern of inheritance and genetic counseling should be offered for patients and family members.
Table 1: Drugs Associated With Drug-Induced Autoimmune-Like Hepatitis
| Association |
|---|
Autoantibodies And Hepatitis C Virus
Circulating autoantibodies are often detected in patients with chronic HCV infection. Antinuclear antibodies , rheumatoid factor , and antismooth muscle antibodies are the most frequently found, while other autoantibodies are infrequent . ANA have been detected in 589 out of 3169 unselected HCV patients included in 16 studies , although the geographic prevalence varied significantly . Yee et al. reported a threefold higher prevalence of ANA in HCV females compared with males, with no correlation between ANA and the response to antiviral therapy, while Stroffolini et al. found no correlation between nonorgan-specific autoantibodies and the main HCV-related epidemiological, biochemical, and histological features, or the response to antiviral treatment. This suggests that the presence of ANA or NOSA in HCV patients should not be considered a contraindication for antiviral treatment. Combined antiviral treatment is safe and effective in NOSA-positive HCV patients, with a similar prevalence of long-term response between NOSA-positive and NOSA-negative patients .
Table 9.1. Metaanalysis of the Main Studies Analyzing Prevalence of Autoantibodies in Unselected Series of Patients With Chronic Hepatitis C Virus Infection
| Autoantibodies |
|---|
Anthony J. Demetris, … Eizaburo Sasatomi, in, 2015
Recommended Reading: Difference Between Hepatitis A And B
What Are The Risks
The ASMA test carries minimal risk. There may be a small amount of bruising at the needle site. Applying pressure on the puncture site for several minutes after the healthcare professional removes the needle can minimize bruising.
Some people have a potential risk of continued bleeding after the professional has removed the needle. Tell the test administrator if youre taking blood thinners or have problems with bleeding or clotting.
In rare cases after youve given a blood sample, inflammation of the vein may occur. This condition is known as phlebitis. To treat it, apply a warm compress several times a day.
In very rare cases, having blood drawn may result in:
- excessive bleeding
- a hematoma, which is an accumulation of blood under the skin
- an infection at the needle site
What Is Being Tested
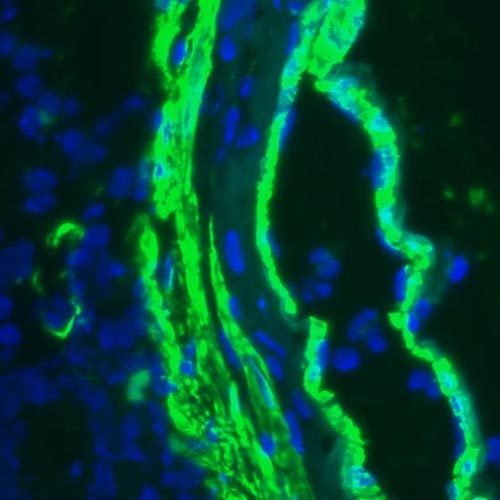
Smooth muscle antibodies are autoantibodies, proteins produced by the bodys immune system that recognize and attack its own actin, a protein found in smooth muscle and other tissues, especially the liver. This test detects and measures the amount of SMA in the blood.
The production of smooth muscle or actin antibodies is strongly associated with autoimmune hepatitis. It may also sometimes be seen in other forms of liver disease, such as primary biliary cholangitis , but usually at lower antibody titers.
Autoimmune hepatitis occurs when the immune system attacks the bodys liver cells. It presents as an acute or chronic inflammation of the liver that is not due to another cause, such as a viral infection, exposure to a drug or toxin, a hereditary disorder, or alcohol abuse. It can lead to liver cirrhosis and, in some cases, to liver failure. Autoimmune hepatitis can affect anyone at any age, but about 80% of patients are women. In the United States, more than 70% of people with this disorder will have SMA or actin antibodies, either alone or along with antinuclear antibodies .
Also Check: How Is Hepatitis C Causes
Reflections On Autoantibody Testing And Conclusion
Indirect immunofluorescence is an old technique requiring expertise and patience that may not be ideal for the modern laboratory. Yet, for the moment, it is here to stay.
Following this report and the fact that members of the American College of Rheumatology were made aware of other inaccurate results for ANA testing, the College set up a Task Force to evaluate the extent of the problem and to recommend solutions. The Task Force reviewed the relevant literature and concluded that solid phase immunoassays may not be appropriate for replacing IIF as a screening test for the detection of ANA . The key recommendations of the Task Force were that, first, IIF ANA test should remain the gold standard for ANA testing and, second, that hospital and commercial laboratories using bead-based multiplex platforms or other solid phase assays for detecting ANA must provide data that their assay has the same or improved sensitivity and specificity as IIF ANA.
Differential Diagnosis And Variant Syndromes
The term AMA-negative PBC or autoimmune cholangitis has been applied to cases that are clinically, histologically, and biochemically compatible with PBC except for the lack of identifiable AMAs serum ANA and antismooth muscle antibodies may be present in high titers. More sensitive testing using cloned mitochondrial antigens such as a triple hybrid recombinant molecule may identify AMA in some patients previously thought to be seronegative.150 In retrospective studies, no significant differences between patients with PBC and these AMA-negative patients have been described,151-154 although a prospective study describing 20 patients with autoimmune cholangitis reported that these patients have higher serum levels of aspartate aminotransferase and bilirubin and lower serum IgM than do patients with classic PBC.155 Although data are largely lacking, it is thought that the response to ursodeoxycholic acid therapy in these patients is the same156 as for those who test positive for AMA.
Distinction of PBC from sarcoidosis with destruction of bile ducts by granulomas may be difficult. The granulomas of sarcoidosis tend to be better formed and more numerous than those of PBC.157 The lack of AMA positivity and the presence of pulmonary involvement also favor a diagnosis of hepatic sarcoidosis.
Kenneth E. Sherman MD, PhD, in, 2010
Don’t Miss: What Is Hepatitis B And C
Serological Markers For Autoimmune Hepatitis
As previously discussed, AIH is divided into two types: AIH-1 and AIH-2. ANA and anti-SMA are associated with AIH-1, whereas anti-LKM-1 and anti-LC-1 antibodies are the hallmarks of AIH-2. These autoantibodies can be detected by IIF testing: ANA on HEp-2 cells and the other autoantibodies on rodent triple tissue . When these markers are absent, it is useful to test for autoantibodies to anti-SLA and anti-neutrophil cytoplasmic antigens . All these antibodies are included in the International Autoimmune Hepatitis Group diagnostic scoring system .
Although ANA can be present in 5080% of AIH-1 patients , they are not disease-specific, since they may also be detected in connective tissues diseases, as well as in non-ALD . ANA in AIH are directed against a variety of antigens, including histones, chromatin, double- and single-stranded DNA, centromere, laminin, small nuclear-ribonucleoproteins, cyclin A, and other not yet identified nuclear antigens. The most frequent encountered patterns are homogeneous and speckled.
P. Brito-Zerón, … M. Ramos-Casals, in, 2017
Looking For Reference Ranges
You may be able to find your test results on your laboratorys website or patient portal. However, you are currently at Testing.com. You may have been directed here by your labs website in order to provide you with background information about the test you had performed. You will need to return to your labs website or portal, or contact your healthcare practitioner in order to obtain your test results.
Testing.com is an award-winning patient education website offering information on laboratory tests. The content on the site, which has been reviewed by laboratory scientists and other medical professionals, provides general explanations of what results might mean for each test listed on the site, such as what a high or low value might suggest to your healthcare practitioner about your health or medical condition.
The reference ranges for your tests can be found on your laboratory report. They are typically found to the right of your results.
If you do not have your lab report, consult your healthcare provider or the laboratory that performed the test to obtain the reference range.
For more information, please read the article Reference Ranges and What They Mean.
Read Also: What Type Of Virus Is Hepatitis C
For The Diagnosis And Classification Of Aih
In accordance with the classical criteria for the diagnosis of AIH, the importance of autoantibody testing is diluted among 12 parameters . Only adult patients with autoantibody reactivity greater than 1/80 for the classical markers, such as anti-smooth muscle antibodies , anti-nuclear antibodies , and anti-liver/kidney microsome type 1 antibodies, score three points. When these markers are absent, other secondary antibodies, such as anti-soluble liver/pancreas antigen and liver cytosol type 1 , should be tested. It is possible to reach a definite diagnosis of AIH without any autoantibody reactivity, and this occurs in approximately 510% of all AIH cases.
Further, a simplified scoring system was proposed based on only four parameters: absence of viral hepatitis antibodies, increased IgG levels, typical histological features, and reactivity for liver autoantibodies . As stated in the interpretation of these simplified criteria, it is impossible to have a definite diagnosis without any reactivity for autoantibodies, and we know this is not true.
Table 1. Main autoantibody markers of AIH with their corresponding target antigens, techniques of detection, and AIH clinical features .
Predictive Value Of Diagnostic Autoantibodies For Asymptomatic Autoimmune Liver Diseasess
Autoantibodies in asymptomatic subjects may precede overt autoimmune disease by many years. This is certainly the case for autoantibodies associated with asymptomatic PBC patients followed up for 19 years.62 Liver biopsies of asymptomatic subjects with mitochondria antibody and normal liver function has shown the histological hallmarks of PBC.63 Autoantibodies to F-actin-specific smooth muscle antibody may also be found in asymptomatic subjects with normal liver function.64 A 12-year follow-up has reported the rare occurrence of development of overt autoimmune hepatitis in asymptomatic subjects with F-actin antibody and normal liver function.65
You May Like: Can You Get Hepatitis C From Kissing
What Does The Test Result Mean
A significant increase in the blood titer of SMA or actin antibody and/or ANA is usually due to autoimmune hepatitis type 1. A small increase in SMA or actin antibody may be present in up to 50% of patients with primary biliary cholangitis . The SMA autoantibody may also be found in other conditions, such as infectious mononucleosis, hepatitis C, and some cancers.
A negative SMA or actin antibody test and an increased titer of LKM1 may indicate autoimmune hepatitis type 2. Type 2 is uncommon in the United States.
If the SMA or actin antibody test and other antibody tests are negative, then symptoms and liver injury may be due to causes other than autoimmune hepatitis.