What Are The Symptoms Of Hepatitis C
During the acute phase most persons have no symptoms or might experience a mild illness. Symptoms of acute HCV infection, when present, may include:
- Jaundice
- Dark-colored urine, light-colored stools
- Diarrhea
- Fever
During the chronic phase hepatitis C usually progresses silently, with no symptoms at all during the first 10-20 years. Signs of severe liver scarring may include:
- Ascites
- Star-shaped vein pattern developing on the swollen belly
- Jaundice
- Itching
- Easy bruising and bleeding
Because symptoms of hepatitis C are usually absent, persons with risk for HCV infection should be tested. The blood test for hepatitis C infection is called the hepatitis C antibody test. People who have hepatitis C infection will show positive antibodies on this test. In many cases, it is necessary to confirm a positive hepatitis C antibody test with a more specific test, such as a test for HCV virus RNA.
If you think you have hepatitis C or have risk for hepatitis C, you should contact your doctor. The Communicable Disease Control Unit may be able to help answer your questions.
Identification Of Hepatitis C Virus
Identification of the novel virus was now a high priority. All the traditional techniques for virus hunting were put to use but, in spite of this, the virus eluded isolation for over a decade. Michael Houghton, working for the pharmaceutical firm Chiron, undertook the arduous work needed to isolate the genetic sequence of the virus. Houghton and his co-workers created a collection of DNA fragments from nucleic acids found in the blood of an infected chimpanzee. The majority of these fragments came from the genome of the chimpanzee itself, but the researchers predicted that some would be derived from the unknown virus. On the assumption that antibodies against the virus would be present in blood taken from hepatitis patients, the investigators used patient sera to identify cloned viral DNA fragments encoding viral proteins. Following a comprehensive search, one positive clone was found. Further work showed that this clone was derived from a novel RNA virus belonging to the Flavivirus family and it was named Hepatitis C virus. The presence of antibodies in chronic hepatitis patients strongly implicated this virus as the missing agent.
George Emil Paladewas the first Romanian to receive the Nobel Prize for Medicine in 1974 for his discoveries concerning the structural and functional organization of the cell. When Palade got the award, he was working at the School of Medicine of the Yale University. He got the award together with Albert Claude and Christian de Duve.
Late 1970s: Exploring A Non
Soon after the identification of HAV, US researchers, including Harvey Alter at the NIH, noticed the screening of donors for HBV prior to transfusions did not eliminate post-transfusion hepatitis cases. They also showed that these cases also did not Hav. a Hav. infection, meaning the post-transfusion cases had an unidentified cause.
There was some urgency to discover what was causing these post-transfusion cases given it was leading to chronic disease and cirrhosis much more often than HBV infection.
This new form of chronic hepatitis was named non-A, non-B hepatitis as it continued to elude scientists, including Alter, working on discovering the infectious agent causing it.
You May Like: Hepatitis C Signal To Cut Off
How Does Hcv Cause Disease
HCV travels through a persons bloodstream to the liver, where it binds to host receptors on the surface of hepatocytes, or liver cells. Once the virus has entered the cells, it replicates rapidly according to some estimates, HCV could potentially make trillions of copies of itself in a day. When the immune system detects these infected cells, it launches a response to destroy them that slows viral production but at the cost of significant inflammation. Left untreated over months or years, this inflammation can quietly lead to the formation of scar tissue in the liver, which gradually degrades the livers ability to filter and detoxify the blood. Scientists are still trying to disentangle how much of the harm from hepatitis C is caused by the immune response against the virus rather than the virus itself.
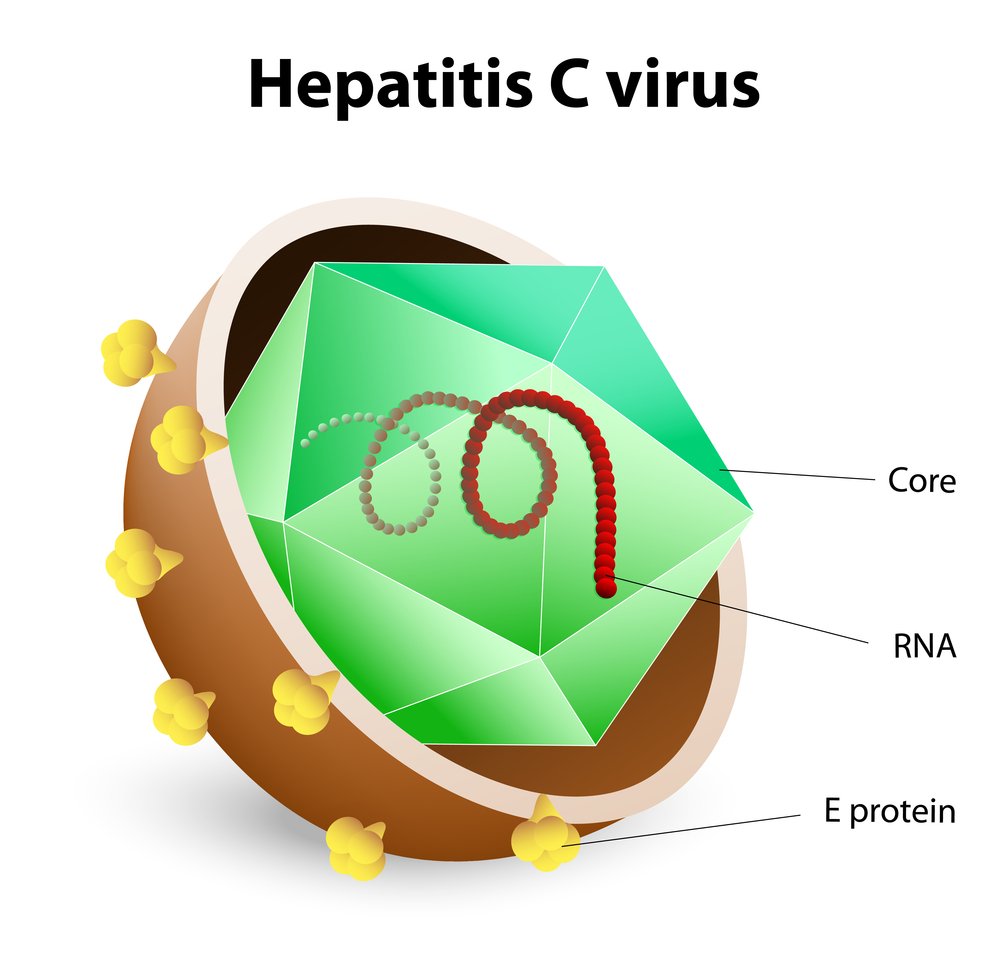
About The Hepatitis C Virus
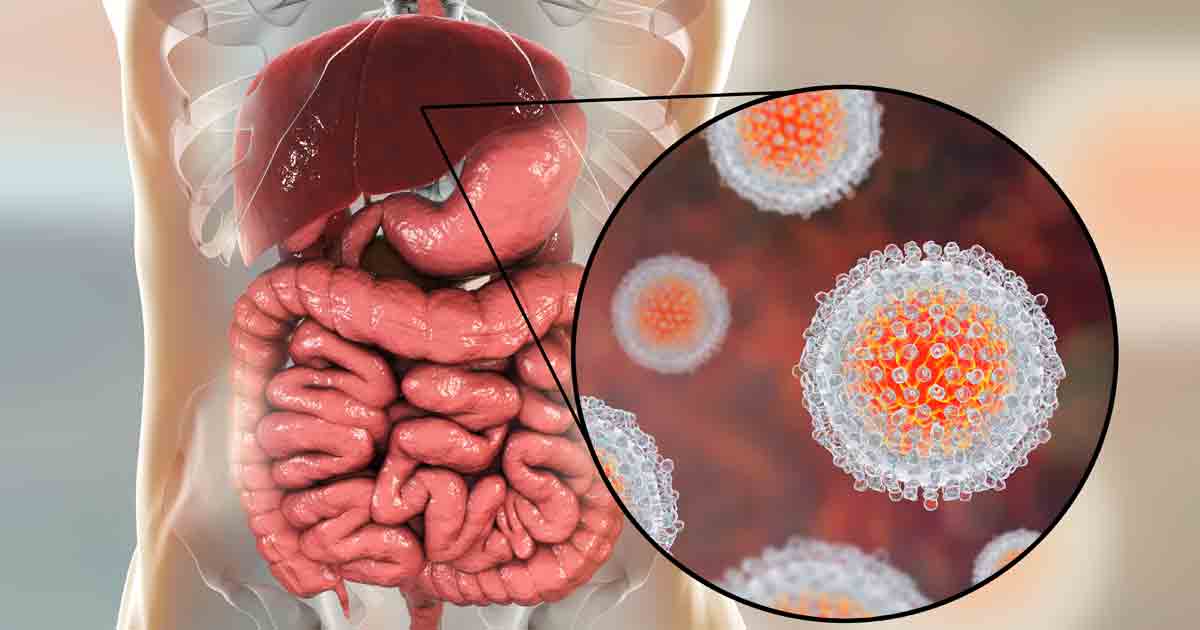
Hepatitis C is a blood-borne virus that predominantly infects the cells of the liver. This can result in inflammation and significant damage to the liver. It can also affect the livers ability to perform its essential functions. Although it has always been regarded as a liver disease – hepatitis means inflammation of the liver – recent research has shown that the hepatitis C virus affects a number of other areas of the body. These can include the digestive system, the lymphatic system, the immune system and the brain.
Hepatitis C was first discovered in the 1980s when it became apparent that there was a new virus causing liver damage. Before being properly identified in 1989 it was originally known as non-A non-B hepatitis. In 1991 a screening process was developed making it possible to detect HCV in blood samples. As a relatively new disease there are still many aspects of hepatitis C which are yet to be fully understood.
There are an estimated 150 million people worldwide chronically infected with hepatitis C. The level of infection, known as prevalence, varies widely from country to country. In some countries, such as Egypt, it is as high as15%. In the United States it is believed to be 1% and in the UK it is believed to be around 0.5%. The virus can only be transmitted by infected blood.
Recommended Reading: What Is Hepatitis C Virus Infection
Discovery Of Hepatitis C Snags Nobel Prize In Medicine
Harvey J. Alter, Michael Houghton and Charles M. Rice share the award for identifying the virus behind the blood-borne liver disease
This years Nobel Prize in Physiology or Medicine was awarded for the discovery of the hepatitis C virus, which causes severe liver disease and chronically infects more than 70 million people worldwide. The prize was jointly awarded to American researchers Harvey J. Alter and Charles M. Rice and British-born scientist Michael Houghton.
Three hepatitis viruses are known to infect the liver: Hepatitis A is transmitted by water or contaminated food, and it causes a short-term infection that is typically resolved within weeks. Hepatitis B and C are transmitted by contaminated blood, and they cause chronic infections that can silently attack the liver for decades. This damage can lead to cirrhosis or liver cancer, which are sometimes only treatable through liver transplants. As a result of hepatitis Cs discovery and blood-screening programs, the virus has been nearly eliminated, and most cases are treatable.
Sheahan speaks similarly highly of Rice. Hes just a special person, Sheahan says. Ive had two mentors, . Theyre both really smart. But these are famous people who are actually good at being humans.
Last years prize was awarded to scientists William Kaelin, Jr., Peter Ratcliffe and Gregg Semenza for the discovery of how cells sense oxygen.
Innovating Against A Silent Killer
Imagine taking an injection and a pill that made you feel every day worse than you ever felt from the infection that was being treated. Alexea Gaffney-Adams, MD, infectious disease specialist
Hepatitis C is dubbed the silent killer as it typically progresses without symptoms, often leaving patients unaware they are infected until their condition is very serious. HCV damages the liver slowly over many years, often moving from inflammation to scarring to permanent, irreversible scarring .
Once a patient has cirrhosis, the liver is unable to heal itself, and this condition can rarely be reversed. For those with end-stage liver disease, treatment is more focused on preventing further damage in an effort to avoid complications, including liver cancer, liver transplantation, and premature death. Hepatitis C has also been associated with other serious conditions, including diabetes, kidney disease, and depression.
In 1987, scientists working at Chiron Corporation, later acquired by Novartis, partnered with the CDC. Using a novel molecular cloning approach, they officially identified and named the virus hepatitis C in 1989.
Interferon was the first, and for a time, the only treatment for hepatitis C. An interferon is a protein produced by the bodys immune system in response to an infection. Side effects were debilitating, and many patients dropped out of what was a very long course of treatment. It was also a largely ineffective treatment.
Don’t Miss: How Many Types Of Hepatitis C Are There
Virologists Who Discovered Hepatitis C Win Medicine Nobel
You can also search for this author in PubMed
Harvey Alter, Charles Rice and Michael Houghton won the 2020 Nobel prize in medicine for their research on the hepatitis C virus.Credit: NIH History Office, John Abbott/The Rockefeller University, Richard Siemens/University of Alberta
A trio of scientists who identified and characterized the virus responsible for many cases of hepatitis and liver disease hepatitis C are the recipients of the 2020 Nobel Prize in Physiology or Medicine.
The winners are Harvey Alter at the US National Institutes of Health in Bethesda, Maryland Michael Houghton, now at the University of Alberta in Edmonton, Canada and Charles Rice, now at the Rockefeller University in New York City. Their work on the hepatitis C virus paved the way for effective treatments for the infection that are now available.
The World Health Organization estimates that 71 million people worldwide are chronically infected with hepatitis C, which causes nearly 400,000 deaths per year, mostly from cirrhosis and liver cancer.
The prize is well deserved, says Ellie Barnes, who studies liver medicine and immunology at the University of Oxford, UK. It stands out as an emblem of great science, she says. Weve got to a point where we can cure most people who are infected. The prizewinners will share an award of 10 million kronor .
Enormous Impacts Of The Hcv Discovery
The breakthrough in HCV discovery has had enormous impacts from two main perspectives: elimination of post-transfusion HCV infection and advent of antivirals against HCV.
In addition to Houghton’s magnificent works, a highly sensitive assay for the detection of HCV in blood transfusion has been developed. This led to a dramatic decline in the risk of post-transfusion HCV infection in the 90s. Since then, transfusion-transmitted HCV infection has been effectively prevented in most countries, ensuring the safety of blood transfuison on a global scale.
”A cure is possible,” Rice said. With this belief, he was continuously dedicated to his work in exploring the structure and function of HCV NS5A protein, now an important target against HCV. Since the first introduction of direct-acting antivirals in 2011, the standard of care for HCV treatment has grown from DAA plus peginterferon/ribavirin therapy to interferon-free DAA therapy. Eventually, the advent of DAA boosted the sustained virologic response rates to 95%â99%, which was a huge advancement as compared to interferon-based therapies .- Following the implementation of DAA treatment, the incidence of HCV-related hepatocellular carcinoma in the Veterans Health Administration reduced by 29.6% from 2015 to 2018.
Don’t Miss: What Is A Hepatic Diet
Harvey J Alter: Demonstrating The Existence Of ”non
In the 1970s, the advent of hepatitis B surface antigen blood test markedly reduced the incidence of post-transfusion hepatitis. However, Harvey J. Alter noticed and reported a skeptical phenomenon: the occurrence of transfusion-associated hepatitis in 22 patients that was unrelated to both hepatitis A and B viruses. As more multiply transfused cases were diagnosed with hepatitis, but none of them were related to the known viruses, Alter proposed the plausible existence of the ”non-A, non-B” hepatitis virus.
To further strengthen the hypothesis, Alter and his colleagues demonstrated the transmissible nature of the serum derived from NANBH patients by injecting it into chimpanzees, a species that is susceptible to both hepatitis A and B viruses. Alter’s dedicated work successfully drew attention to this transmissible virus-like agent that caused NANBH.
Egyptian Model An Eye Opener For The Middle To Low Income Countries
In the middle and low income countries the Egyptian model is the best strategy for combating HCV. Egypt was regarded as one of the countries with the highest prevalence till 2015 according to WHO report. This was the outcome of mass treatment with unsterilized syringes for schistosomiasis during 1960s to 1980s, which has represented the largest ever iatrogenic spread of blood borne infection in the history. After this mammoth burden with an estimated 10% seroprevalence, the agreement of Gilead Sciences, than Bristol-Meyers-Squibb and Ministry of Health, brings down cost of Sofosbuvir and Daclatasvir and making local brands in much cheaper cost. Then with continuous efforts of opening up of health care provision, treatment centres and web based appointment system, Egypt is regarded as being on the right path as per latest estimates from local and international audits. Egyptian model is not only cost efficient but also easily acquirable. Egypt is the only low- and middle-income country, among nine of countries which are on the track of WHO 2030 elimination program.
Don’t Miss: How Is Hepatitis C Caused
How Can I Prevent Passing On The Virus To Others
If you have a current hepatitis C infection you should:
- Not share any injecting equipment such as needles, syringes, etc.
- Not donate blood or carry a donor card.
- Not share razors, toothbrushes or anything else that may possibly be contaminated with blood.
- Use condoms when having sex. The risk of passing on HCV during sex is small but risk is reduced even further by using condoms.
- Advise anybody with whom you have had sex or shared needles to have tests as well, to check they do not have HCV.
There is currently no vaccine available to protect against hepatitis C.
Virus Discovery And Contribution Of Laureates
The discovery of hepatitis C virus can be traced back to the mid-1970s, when laureate Harvey J. Alter was the Chief of the Infectious Disease Section in the Department of Transfusion Medicine at the National Institutes of Health, which is the apex US agency for public health research.
Alterâs team demonstrated that the hepatitis that occurs after blood transfusion is not caused by hepatitis A or B virus.
Research on identifying the cause was stalled for a decade, but in 1987, laureate Michael Houghton, along with virologists Qui-Lim Choo and George Kuo made a landmark discovery. In collaboration with virologist Daniel W. Bradley of the Centers for Disease Control and Prevention in the US, the team managed to identify the hepatitis C virus and develop a diagnostic test.
Alter then confirmed the presence of viruses in other specimens in 1988.
Houghton, Choo and Kuo then worked for Chiron Corporation, a US biotechnology company. A patent battle ensued with CDC, which was subsequently dropped after Chiron paid $1.9 million to CDC and over $300,000 to Bradley.
The same year, Charles M. Rice, then a researcher at Washington University, identified a part of the HCV genome that was responsible for viral replication. He genetically engineered a modified HCV and by testing on chimpanzees, was able to prove that HCV solely causes hepatitis through transfusion.
You May Like: Ways To Contract Hepatitis C
Why Was Hcv So Difficult To Isolate And Identify
One difficulty was the danger hepatitis C posed to researchers, who had to exercise great care when working with it. Also, because hepatitis C was initially known only as a human disease, researchers did not have an animal model to run experiments on. Eventually, it was found that chimpanzees could also be infected. But a more enduring problem was that the virus was present in such tiny concentrations in the blood of patients despite being highly infectious that traditional immunological methods of finding and identifying the virus were ineffective.
S 1980s: Interferon Emerges As A Treatment
With HBV and Hav. being identified and scientists continuing to search for the non-A, non-B hepatitis virus, other researchers got to work on finding treatments for hepatitis.
Studies showed that HBV patients responded well to interferon, a cytokine produced by the immune system against viral infections.
As a result, researchers at NIH did a pilot study of interferon against non-A, non-B hepatitis the results were dramatic with 50% of patients showing no signs of liver infection in decade long follow ups. Interferon was approved for non-A, non-B hepatitis in 1984.
Recommended Reading: What Does It Mean To Have Hepatitis C Antibodies
Hepatitis A Global Threat To Human Health
Liver inflammation, or hepatitis, a combination of the Greek words for liver and inflammation, is mainly caused by viral infections, although alcohol abuse, environmental toxins and autoimmune disease are also important causes. In the 1940s, it became clear that there are two main types of infectious hepatitis. The first, named hepatitis A, is transmitted by polluted water or food and generally has little long-term impact on the patient. The second type is transmitted through blood and bodily fluids and represents a much more serious threat since it can lead to a chronic condition, with the development of cirrhosis and liver cancer . This form of hepatitis is insidious, as otherwise healthy individuals can be silently infected for many years before serious complications arise. Blood-borne hepatitis is associated with significant morbidity and mortality, and causes more than a million deaths per year world-wide, thus making it a global health concern on a scale comparable to HIV-infection and tuberculosis.
Figure 1 There are two main forms of hepatitis. One form is an acute disease caused by Hepatitis A virus that is transmitted by contaminated water or food. The other form is caused by Hepatitis B virus or Hepatitis C virus . This form of blood-borne hepatitis is often a chronic disease that may progress to cirrhosis and hepatocellular carcinoma.
The University Of Chiron
Houghton launched his hunt for the virus in 1982, at a biotechnology company called the Chiron Corporation in Emeryville, California. The firm had been nicknamed the University of Chiron for its academic pedigree and its reputation for pursuing cutting-edge science.
At the time, blood transfusions tainted with HCV were infecting 160 people in the United States each day. Left untreated, the virus can damage the liver and cause liver cancer. Today, despite the availability of blood-screening methods and treatments, the World Health Organization estimates that 71 million people around the world are still infected with HCV.
These were the days before the widespread use of the polymerase chain reaction , which provides an easy way to amplify DNA. The idea of sequencing a novel virus within weeks of its emergence as happened for the SARS-CoV-2 coronavirus earlier this year was unthinkable. Houghton began screening for viral nucleic acids using samples from infected and uninfected chimpanzees supplied by Daniel Bradley at the US Centers for Disease Control and Prevention in Atlanta, Georgia.
Don’t Miss: How Do They Treat Hepatitis C