Treatment Rates For Chb And Factors Associated With Treatment
Among the patients in the Truven database with CHB diagnosis, we found that 30.66% had received at least 1 prescription for HBV medication at any time during the study period. Given a diagnosis rate of 18.60% for CHB, the estimated treatment rate for all CHB was only 5.70% .
As shown in Table 2, treatment rates were significantly higher in patients with cirrhosis or HCC , significantly higher for those with gastroenterology or infectious disease care compared with those followed up in a primary care clinic only , and significantly higher for those with health maintenance organization insurance compared with preferred provider organization insurance . Notably, we found the highest treatment rates among those with the lowest and highest out-of-pocket medical expense.
Evolution Of Serologic Tests After Infection And Vaccination
To optimally understand and interpret HBV serologic diagnostic tests, it is important to understand how serologic markers evolve over time after initial infection and after receiving hepatitis B vaccine. Following acute HBV infection, the evolution of the pattern of serologic markers depends on the outcome of the host immune response, which typically correlates with the patient’s age. Adults have resolution of HBV infection approximately 90% of the time, whereas 30 to 90% of young children will fail to resolve the infection and thus develop chronic HBV infection. The following discussion will summarize the evolution of key serologic markers during acute HBV infection with recovery, chronic HBV, and post-immunization, with each topic accompanied by corresponding animations from the Centers for Disease Control and Prevention Hepatitis B Serology Training as audio-visual guides to aid in understanding.
Acute Vs Chronic Hepatitis B
A hepatitis B infection can result in either an acute infection or a chronic infection. When a person is first infected with the hepatitis B virus, it is called an “acute infection” . Most healthy adults that are infected do not have any symptoms and are able to get rid of the virus without any problems. Some adults are unable to get rid of the virus after six months and they are diagnosed as having a “chronic infection.” A simple blood test can diagnose an acute or chronic hepatitis B infection.
The risk of developing a chronic hepatitis B infection is directly related to the age at which a person is first exposed to the hepatitis B virus. The younger a person is when they are first infected, the greater the risk of developing a chronic hepatitis B infection:
- More than 90% of infants that are infected will develop a chronic hepatitis B infection
- Up to 50% of young children between 1 and 5 years who are infected will develop a chronic hepatitis B infection
- 5-10% of healthy adults 19 years and older who are infected will develop a chronic hepatitis B infection
The recommendation for hepatitis B vaccination of babies and children is so important because they are at the greatest risk of developing a chronic infection if they are not protected against the hepatitis B virus as soon as possible.
You May Like: Who Needs Hepatitis C Screening
Current Treatment Of Chronic Hepatitis B: Clinical Aspects And Future Directions
- 1The Fourth Affiliated Hospital of Zhejiang University School of Medicine, Jinhua, China
- 2International Institutes of Medicine, Zhejiang University, Jinhua, China
Hepatitis B virus infection is a public health threat worldwide, and there is no direct treatment yet available. In the event of infection, patients may present liver cirrhosis and cancer, which threaten the patients health globally, especially in the Asia-Pacific region and China. In 2019, Chinese hepatopathologists updated the 2015 Guidelines for the Prevention and Treatment of Chronic Hepatitis B as the clinical reference. The other versions formulated by the American Association for the Study of Liver Diseases , European Association for the Study of the Liver , and Asian-Pacific Association for the Study of the Liver also provide clinical guidance. However, there are still some issues that need to be addressed. In the present study, the following aspects will be introduced successively: Who should be treated in the general population according to the guidelines Treatment of specific populations infected with HBV Controversial issues in clinical practice Perspective.
Treatment Of Chronic Hepatitis B In Children
Vaccination against HBV among young Chinese individuals decreased the HBV infection rate. In recent years, several studies reported gradually increasing the horizontal transmission of HBV in early childhood, and family members may be the main source of infection. Interferons and NAs are the potential treatment options according to the age of young people .
You May Like: Blood Test For Hepatitis C Virus
Low Response Rates And Nonresponders
Low vaccination response rates have been associated with obesity, smoking, immunosuppression , and advanced age. Approximately 25-50% of persons who initially do not have a vaccine response will show a response to one additional vaccine dose, and 50-75% of individuals will have a response to a fourth higher dose of Engerix B or Recombivax HB, or a second 3-dose series.
Postvaccine antibody titers do not need to be obtained in routine vaccinations of children or adults. It is recommended that testing for anti-HBs be obtained 4-12 weeks after vaccination in the following groups :
- Immunocompromised patients, including those on hemodialysis, HIV patients, and others
- Infants born to HBsAg-positive mothers
- Healthcare professionals
- Sexual partners of HBsAg-positive patients
Nonresponders, should be revaccinated with another series of 3-dose hepatitis B vaccine. Consider delaying revaccination for several months after initiation of antiretroviral therapy in patients with CD4 counts below 200 cells/mm3 or those with symptomatic HIV disease. The delay in these individuals is an attempt to maximize the antibody response to the vaccine.
Do not defer vaccination in pregnant patients or patients who are unlikely to achieve an increased CD4 count. Individuals at increased risk of severe complications due to HBV infection include those unlikely to achieve CD4 counts of 200 cells/mm3 or above after antiretroviral therapy and HIV-infected pregnant women.
What Are The Types Of Hepatitis B
There are two types of hepatitis B infection: acute and chronic.
Acute
An acute infection happens at the beginning, when you first get infected with hepatitis B. Many people are able to clear it from their bodies and recover. In fact, this is true of about 4 in 5 adults who are infected.
Chronic
If you are not able to clear the infection within six months or longer, you have chronic hepatitis B. It is chronic hepatitis B that leads to inflammation and the serious, and possibly fatal, illnesses of cirrhosis of the liver and liver cancer. Treatment can slow disease progress, reduce the chance of liver cancer and increase your chances of surviving.
You May Like: What Is Hepatic Function Panel
Diagnosed And Undiagnosed Patients With Chb
Of the total number of 511029 privately insured individuals who we estimated should have been diagnosed with CHB , only 95075 had been diagnosed, leaving a total of 415954 remaining undiagnosed.
If using the number of individuals diagnosed with CHB from the sensitivity analysis that only required 1 inpatient or 1 outpatient diagnosis for CHB, the number of those with undiagnosed CHB would be 363861 , giving a rate of undiagnosed CHB of 71.20% . The rate of diagnosed CHB remained low at 28.80% .
How Is Hepatitis B Treated
Your healthcare provider will treat you based on what type of hepatitis B you have, acute or chronic.
Acute hepatitis B infections
If you develop an acute form of the condition, you probably wont need medical treatment. Instead, your doctor will likely suggest that you get plenty of rest, drink lots of fluids and maintain a healthy diet to support your body as it fights off the infection.
Chronic hepatitis B infections
If you have chronic hepatitis B, you might be a candidate for drug therapy. Usually, drug therapy is used only if you have active liver disease. There are seven drugs that are approved by the U.S. Food and Drug Administration to treat hepatitis B. Two are injectable forms of interferon, while the five other antivirals are tablets.
You will need to take these medications every day. They help by slowing the viruss ability to multiply in your system. This helps reduce swelling and liver damage. Youll need to be regularly monitored for early signs of liver damage and liver cancer. Your healthcare provider will want to see you once or twice a year.
Read Also: Hepatitis A Vaccine Cost Cvs
Serological Markers For Hbv Infection
Serological markers for HBV infection consist of HBsAg, anti-HBs, HBeAg, anti-HBe, and anti-HBc IgM and IgG. The identification of serological markers allows: to identify patients with HBV infection to elucidate the natural course of chronic hepatitis B to assess the clinical phases of infection and to monitor antiviral therapy .
HBsAg is the serological hallmark of HBV infection. After an acute exposure to HBV, HBsAg appears in serum within 1 to 10 weeks. Persistence of this marker for more than 6 months implies chronic HBV infection . Several studies have reported the association between transcription activity of cccDNA in the liver and serum HBsAg levels . Differences in the serum HBsAg levels during the different phases of infection indicate the distribution of cccDNA during the respective phases of the disease. The serum HBsAg titers are higher in patients with HBeAg-positive CHB than in HBeAg-negative CHB . Monitoring of quantitative HBsAg levels predicts treatment response to interferon and disease progression in HBeAg-negative CHB patients with normal serum alanine aminotransferase levels .
Immune Tolerant Chronic Hepatitis B
Immune tolerance is a status presenting HBeAg+, high viral replication, and normal ALT. It was put forward as a lack of specific immune response to HBV due to the immature immune system during infancy. No treatment is recommended for such cases in the current guidelines, as it is speculated that patients in the immune tolerance phase have a low risk of progression to liver cirrhosis or cancer . Moreover, ineffective treatment may lead to a low e-antigen seroconversion rate . Patients with immune tolerance are mostly teenagers and readily develop drug resistance because of poor compliance after long-term antiviral treatment .
You May Like: What Lab Test For Hepatitis C
Candidates In The General Population
Antiviral treatment is an effective therapeutic strategy for CHB patients that efficiently suppresses HBV replication, decreases inflammatory necrosis in the liver, reduces the incidence of liver cirrhosis and related complications, and reduces the fatality rate associated with hepatocellular carcinoma and other liver diseases. In the 2019 China guidelines , HBV infection is divided into four phases: immune tolerance, immune clearance, immune control, and immune reactivity, and it is different from the 2015 version . Additionally, the 2019 China guidelines eased the restrictions on indications for antiviral therapy, and reducing the demand for HBV-DNA load. Conversely, the HBV-DNA load is considered for the performance of antiviral therapy in the 2018 guidelines updated by the 2018 AASLD guideline and the 2017 EASL guidelines . For the treatment of HBV infection with normal ALT , antiviral therapy is recommended in patients > 30-years-old with a family history of liver cirrhosis or cancer in the 2019 China guidelines. In another case > 30-years-old without a family history of liver cirrhosis or cancer, a hepatic biopsy was recommended. Although we can refer to many guidelines, there are many patients failed to fulfill the criteria for treatment at follow-up and eventually developed liver fibrosis, cirrhosis, and cancer .
Table 1. Comparison between 2015 and 2019 guidelines.
Table 2. Indications for chronic hepatitis B treatment in 2017 and 2018 guidelines.
Recommended Groups For Routine Hbv Screening
Multiple organizations in the United States recommend performing routine screening for hepatitis B virus infection for persons who are at increased risk of acquiring HBV these organizations include the Centers for Disease Control and Prevention , the U.S. Preventive Services Task Force , the American Association for the Study of Liver Diseases , and the American College of Physicians The USPSTF recommendation was issued in 2014 as a grade B recommendation, meaning clinicians should offer or provide this service in practice. The following list summarizes the groups considered to be at high risk for HBV infection, in whom screening is recommended by the CDC. Certain indications for screening depend on country level HBV prevalence .
Don’t Miss: Are There Cures For Hepatitis
Acute Hepatitis B Infection
An acute hepatitis B infection may last up to six months and infected persons are able to pass the virus to others during this time. A simple blood test can let a person know if the hepatitis B virus is in their blood or if they have successfully gotten rid of the virus. The doctor should periodically test your blood over the six-month period to monitor the health of your liver and check progress towards recovery. In a person who has recovered from an acute hepatitis B infection, a taken six-months after initial diagnosis will show that there is no more hepatitis B virus in your blood.
Being diagnosed with acute hepatitis B can be difficult. As you move through the initial six-month period, there are tips and strategies to help.
Until your health care provider confirms that the blood test shows that there is no more hepatitis B virus in your blood, it is important to protect others from a possible infection.
It is also important to have your sexual partner and family members get tested for hepatitis B. If they have not been infected and have not received the hepatitis B vaccine then they should also start the hepatitis B vaccine series.
Be sure to follow-up with your health care provider for any additional blood tests that are needed to confirm your recovery from an acute infection.
Whats The Outlook For People With Chronic Hep B
The majority of people who have hep B as adults fully recover within 1 to 3 months. Children under the age of 5 are at the highest risk of developing chronic hep B infection.
Medications can help manage chronic hep B, but about 15 to 25 percent of people die prematurely from liver cancer, cirrhosis, or liver failure.
More than half of liver cancers are caused by chronic hep B infection. Taking your medications as prescribed and following your healthcare professionals recommendations can help you minimize your chances of complications.
Also Check: How Dangerous Is Hepatitis B
Understanding Your Test Results
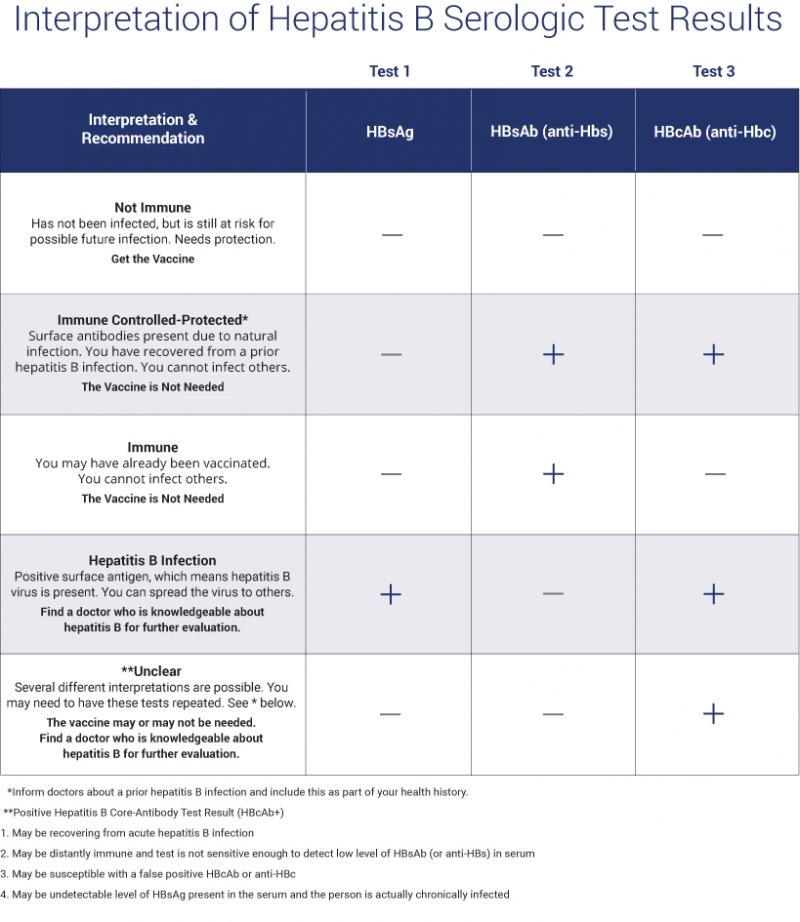
Understanding your hepatitis B blood tests can be confusing. It is important to talk to your health care provider so you understand your test results and your hepatitis B status. Are you infected? Protected? Or at risk? The Hepatitis B Panel of blood tests includes 3 tests and all three results must be known in order to confirm your status.
Below is a chart with the most common explanation of the test results, but unusual test results can occur. Please note that this chart is not intended as medical advice, so be sure to talk to your health care provider for a full explanation and obtain a printed copy of your test results. In some cases, a person could be referred to a liver specialist for further evaluation.
More Detailed Information About Hepatitis B Blood Tests
An acute hepatitis B infection follows a relatively long incubation period – from 60 to 150 days with an average of 90 days. It can take up to six months, however, for a person to get rid of the hepatitis B virus. And it can take up to six months for a hepatitis B blood test to show whether as person has recovered from an acute infection or has become chronically infected .
The following graphic from the U.S. Centers for Disease Control and Prevention represents the typical course of an acute hepatitis B infection from first exposure to recovery.
According to the CDC, a hepatitis B blood test result varies depending on whether the infection is a new acute infection or a chronic infection.
Approaches By Virus Life Cycle Stage
consist of a and sometimes a few stored in a capsule made of , and sometimes covered with a layer . Viruses cannot reproduce on their own and instead propagate by subjugating a host cell to produce copies of themselves, thus producing the next generation.
Researchers working on such “” strategies for developing antivirals have tried to attack viruses at every stage of their life cycles. Some species of mushrooms have been found to contain multiple antiviral chemicals with similar synergistic effects.Compounds isolated from fruiting bodies and filtrates of various mushrooms have broad-spectrum antiviral activities, but successful production and availability of such compounds as frontline antiviral is a long way away. Viral life cycles vary in their precise details depending on the type of virus, but they all share a general pattern:
Before cell entry
This stage of viral replication can be inhibited in two ways:
Uncoating inhibitor
Inhibitors of uncoating have also been investigated.
During viral synthesis
Reverse transcription
Integrase
Transcription
Also Check: How Do You Get Infected With Hepatitis B
Acute Hbv Infection With Recovery
Following acquisition of HBV, the first detectable serologic marker in blood is HBsAg. Detection of HBsAg typically occurs at 4 weeks following infection, with a range of 1 to 9 weeks following infection. Typically, when HBsAg is detectable during acute infection, HBV DNA can also be detected in blood. During early infection, persons may also test positive for HBeAg, which is a marker of infectivity and higher HBV DNA levels. Nearly all persons will test negative for HBsAg and HBV DNA by 15 weeks after the onset of symptoms. With acute HBV infection, IgM anti-HBc is typically detectable at the onset of symptoms and persists for 6 to 9 months following infection. Total anti-HBc, which consists of IgM anti-HBc and IgG anti-HBc, can similarly be detected at the onset of symptoms, but persists indefinitely as a marker of prior infection. During recovery, and after the disappearance of HBsAg, persons who have immunologic control of acute infection will develop antibodies to HBs , which may persist indefinitely or wane over time. It is important to note that following the disappearance of HBsAg and prior to the appearance of anti-HBs, there is a period of time when IgM anti-HBc and total anti-HBc may be the only detectable serologic markers. This period of time is known as the window period.