Reversibility Of Hepatic Encephalopathy
Classically, hepatic encephalopathy was regarded as a reversible condition. Patients appeared to improve with either drug therapy or liver transplantation. However, a recent study assessed cirrhotic patients who had apparently recovered from an episode of overt hepatic encephalopathy. After careful psychometric testing, it was discovered that these clinically improved patients had residual cognitive impairment compared with cirrhotic patients with either minimal hepatic encephalopathy or no encephalopathy.
In 2009, Sotil et al evaluated 39 patients who had undergone liver transplantation about 1.5 years before the study. The 25 patients who had hepatic encephalopathy prior to transplantation, on the whole, performed worse on psychometric testing than the 14 patients with no history of overt encephalopathy prior to transplantation.
In 2011, Garcia-Martinez et al assessed the cognitive function in 52 patients who had undergone liver transplantation. Global cognitive function after transplantation was worse in patients with a history of alcohol-induced cirrhosis, patients with diabetes, and patients with a history of hepatic encephalopathy prior to transplantation. Furthermore, the brain volume after transplantation was smaller in patients with a history of hepatic encephalopathy prior to transplantation than in patients with no overt encephalopathy. These are provocative findings that require additional investigation.
Clinical Scales For Grading He
A number of scales have been devised for the diagnosis of HE the first of its kind was proposed by Parsonsmith and colleagues in 1957. For patients with moderate to severe HE, the Glasgow Coma scale can also be employed.
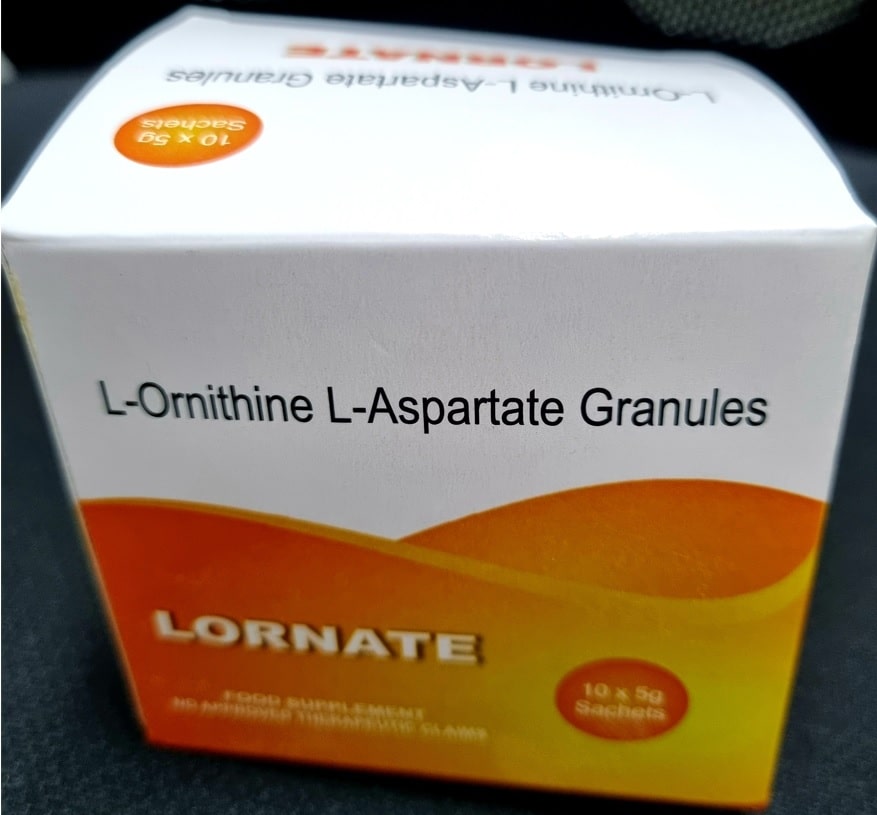
Table 1: West-Haven Criteria for Hepatic Encephalopathy
| Stage | |
|---|---|
| Normal examination if impaired psychomotor testing, consider MHE | |
| 1 | Impaired addition or subtraction mild asterixis or tremor |
| 2 |
MHE, minimal hepatic encephalopathy.
The West-Haven Classification Table
Stage 0. MHE . Lack of detectable changes in personality or behavior. Minimal changes in memory, concentration, intellectual function, and coordination. Asterixis is absent.
Stage 1. Trivial lack of awareness. Shortened attention span. Impaired addition or subtraction. Hypersomnia, insomnia, or inversion of sleep pattern. Euphoria, depression, or irritability. Mild confusion. Slowing of ability to perform mental tasks. Asterixis can be detected.
Stage 2. Lethargy or apathy. Minimal disorientation. Inappropriate behavior. Slurred speech. Obvious asterixis. Drowsiness, lethargy, gross deficits in ability to perform mental tasks, obvious personality changes, inappropriate behavior, and intermittent disorientation, usually regarding time.
Stage 3. Somnolent but can be aroused, unable to perform mental tasks, gross disorientation about time and place, marked confusion, amnesia, occasional fits of rage, present but incomprehensible speech.
Treatments To Increase Ammonia Clearance
Zinc. Low zinc concentrations are common in patients with cirrhosis of the liver, particularly those with HE. Even in patients who are not zinc deficient. Patients with fulminant hepatic failure and subacute hepatic failure have also been shown to have low serum zinc levels. Zinc deficiency also leads to alteration of neurotransmitters like GABA and norepinephrine. Zinc supplementation has been tried in HE. It may have a role in mild chronic HE, though further trials are necessary.
Unequivocal evidence of benefit of oral zinc therapy for treatment of acute HE is lacking. Zinc sulfate and zinc acetate have been used at a dose of 600 mg orally every day in clinical trials. HE improved in two studies there was no improvement in mental function in two other studies. However, an interesting study from Japan in 2010 showed zinc supplementation significantly improved patients’ quality of life, as it improved the physical component scale but not the mental component scale. Zinc supplementation also significantly decreased HE grade and blood ammonia levels and improved Child-Pugh score and neuropsychological tests compared with standard therapy. Interestingly this study showed as well administration of zinc in combination with L-carnosine showed to enhance intestinal barrier and improve zinc plasma levels.
Some examples for probiotics available in USA that contains same species that showed some effect for HE include :
| Drug |
|---|
You May Like: Can Hepatitis Cause Mental Illness
Provision Of Supportive Care
Standard supportive care is required for all hospitalized patients with HE. Patient safety and frequent bedside monitoring of mental status are crucial. This can require additional personnel and, in the case of comatose patients, admission to the intensive care unit, endotracheal intubation, or both. Although temporary restriction of dietary protein may be necessary, patients with HE should avoid prolonged periods of fasting. Although the restriction of dietary protein at the time of acute HE can be part of therapy, protracted nitrogen restriction can lead to malnutrition. Appropriate enteral nutrition, by mouth or nasogastric feeding tube, should be administered as soon as feasible.
Intravenous Administration To Cirrhotic Patients
In a double-blind, randomized, placebo-controlled, cross-over clinical trial, 10 cirrhotic patients with HE and hyperammonemia were studied on four separate days with an interval of 25 days between single infusions of a range of doses of LOLA. After an overnight fast, the patients consumed a liquid protein formula of 0.25 g/kg at 9 a.m. and 0.50 g/kg at 1 p.m. Blood was drawn for analysis of ammonia and amino acids immediately before and every 2 h after infusion. Doses of LOLA were 0 g , 5 g, 20 g, and 40 g starting at 9 a.m. and continuing for 8 h. The dose of LOLA was selected randomly .
Following continuous infusion of placebo , concentrations of l-ornithine and l-aspartate remained stable for the entire 8-h period. Following LOLA 5 g , the concentration of l-ornithine increased to 132±13 mol/L and 148±10 mol/L while that of l-aspartate increased to a near steady state level . Continuous administration of 2.5 g/h LOLA increased the level of l-ornithine and l-aspartate 4-fold whereas 5 g/h LOLA led to a 10-fold increase of l-ornithine and a 20-fold increase of l-aspartate above basal placebo levels .
Fig. 1
Recommended Reading: Antiviral Medication For Hepatitis B
Oxidative And Nitrosative Stress
Enhanced production of reactive nitrogen species and reactive oxygen species occurs in cultured astrocytes that are exposed to ammonia, inflammatory cytokines, hyponatremia or benzodiazepines. It’s suggested that glutamine formed in the cytoplasm enters the mitochondrial matrix and is cleaved to release ammonia while still inside the mitochondria. Evidence indicating a close association and interplay between astrocyte swelling and ROS is now growing.
Treatments To Improve Sleep Disturbances
Sleep disturbances are more common in patients with cirrhosis than in control subjects. Whether or not this relates to hepatic encephalopathy is unclear. A trial compared the histamine H1 blocker hydroxyzine with placebo in patients with cirrhosis and minimal hepatic encephalopathy. Sleep efficiency and the patients’ subjective quality of sleep improved in patients receiving hydroxyzine at bedtime. However, there was no accompanying improvement in cognition, as measured by neurophysiologic tests. The authors urged caution when prescribing hydroxyzine, on account of the risk of worsening encephalopathy in some patients.
Read Also: Hiv Hepatitis B And C Test
Identification And Removal Of Precipitating Factors
When there is obvious worsening of HE , a vigorous search to identify and eliminate a precipitating factor or factors should be instituted.
In most cases of cirrhosis with acute or chronic HE, a precipitating factor is found, such as the following:
GI hemorrhage. Exploration requires stool analysis and/or placement of a nasogastric tube.
Infections. This factor requires culture of all appropriate body fluids blood, urine, ascites, and pleural fluid when present. Spontaneous bacterial peritonitis and pneumonia may present with HE.
Use of psychoactive medication. This factor may require a urine screen for benzodiazepines, narcotics, and other sedatives.
Constipation. Noncompliance with lactulose doses at home.
Renal and electrolyte disturbances. These include renal failure, metabolic alkalosis, hypokalemia, dehydration, and diuretic effects.
Acute deterioration of liver function in cirrhosis. HE in cirrhosis seldom reflects the acute impact of liver failure. Exceptions include the presence of superimposed alcoholic hepatitis, the development of an acute circulatory disturbance , and the impairment of liver function seen after surgery in cirrhosis.
TIPS. Precipitating events should also be sought with the development of encephalopathy after placement of TIPS for control of portal hypertension.
Spontaneous encephalopathy should raise the suspicion of an abnormal collateral circulation imaging of the abdomen should be performed looking for spontaneous splenorenal shunt.
Can Not Be Said Yes
Evaluation of efficacy of ornithine aspartate in reducing serum levels of ammonia and increasing neuropsychiatry status in HE has been studied during at least the last 3 decades. However, few double-blind, randomized, placebo-controlled clinical trials were able to detect such effect. Reduction of ammonia and improvement of encephalopathy clinical status, measured by psychometric tests ) or mental status through the clinical scoring of encephalopathy has been the form of evaluating drug efficacy. Tolerance and the appearance of adverse effects shown by the patients have also been subject to evaluation in most of these studies. Generally, the studies selected here showed that LOLA was able to reduce hyperammonemia in patients with
You May Like: Hepatitis A And B Shots
Ccrct = Cochrane Collaboration Register Of Controlled Trial
Evaluation of the methodological quality of the studies was finished by using JADAD et al. scale, composed by three items, quantifying the probability of bias related to the trial according to the description of randomization, masking, withdrawals and drop outs. Scores vary from 1 to 5 studies that present scores 1 or 2 are considered as showing low quality and studies that present scores 3 to 5 are considered as showing high quality.
A Critical Analysis Of Studies Assessing L
INTRODUCTION
Change in the brain function is a characteristic complication of acute or chronic liver failure. In addition to the traditional presentation, as frank hepatic encephalopathy , a subclinical manifestation form is currently known, where the patient has a normal neurological status, but manifests motor and cognitive deficits detected only by specific tests. Minimum hepatic encephalopathy is an entity of unquestionable clinical importance due to the high prevalence, occurring in up to 84% of cirrhotic patients. Furthermore, MHE may potentially evolve to frank HE in about 56% in 3 years negatively interfering in the survival of these individuals. This survival is not bigger than 20% in 5 years, following the identification of the clinically manifested disease. In spite of a silent course, studies have shown that daily activities and quality of life of cirrhotic individuals with MHE are compromised. Use of lactulose in the treatment MHE was related to improvement in the detection tests of the disease, in addition to the impact in the quality of life of these individuals however, its routine usage in the clinical practice is questionable and more prospective, randomizes trials are necessary.1
Criteria for consideration of studies in this review Type of studies The review has included all the randomized controlled double-blind clinical trials performed
Recommended Reading: What Kind Of Doctors Treat Hepatitis C
Treatments To Decrease Intestinal Ammonia Production
Diet
In the late 19th century, it was recognized that the feeding of a high-protein diet to dogs that had undergone portosystemic shunt surgery could produce symptoms of abnormal coordination and stupor in the treated animals.
In the 20th century, low-protein diets were routinely recommended for patients with cirrhosis, in the hope of decreasing intestinal ammonia production and in preventing exacerbations of hepatic encephalopathy. An obvious consequence was the worsening of preexisting protein-energy malnutrition. Protein restriction may be appropriate in some patients immediately following a severe flare of symptoms . However, protein restriction is rarely justified in patients with cirrhosis and persistent hepatic encephalopathy. Indeed, malnutrition is a more serious clinical problem than hepatic encephalopathy for many of these patients.
Diets containing vegetable proteins appear to be better tolerated than diets rich in animal proteins, especially proteins derived from red meats. This may be because of increased content of dietary fiber, a natural cathartic, and decreased levels of aromatic amino acids. Aromatic amino acids, as precursors of the false neurotransmitters tyramine and octopamine, are thought to inhibit dopaminergic neurotransmission and worsen hepatic encephalopathy.
Cathartics
In subsequent years, multiple randomized trials have reinvestigated the efficacy of lactulose.
Antibiotics
Assessment Of Study Quality
The methodological quality of the included studies was assessed using the Jadad scale, a three item checklist assessing randomisation, blinding and withdrawals, with a maximum score of 5. Two reviewers independently assessed the methodological quality of the included studies, with disagreements resolved through discussion.
Don’t Miss: Booster Dose Of Hepatitis B Vaccine
Systematic Reviews And Meta
Results of several systematic reviews and/or meta-analyses on the effects of LOLA in the treatment of HE in cirrhosis have been published in the last two decades. These analyses had a range of objectives and were focused on various subtypes of HE in cirrhosis, oral versus intravenous formulations of LOLA, and differences in experimental design. Extraction of the optimal amount of information and insights regarding the efficacy of LOLA from these analyses requires that they be critically reviewed. The first study published in abstract form , based upon the findings of five double-blind, placebo-controlled RCTs in 246 patients with cirrhosis assessed the efficacy of intravenous infusions of LOLA in terms of improvement of mental state, number connection test-A scores and hyperammonemia. LOLA treatment resulted in a 3.22-fold greater chance of being free from overt hepatic encephalopathy after 7 days of therapy compared to placebo. Treatment also led to significant reduction of post-prandial ammonia during this time.
In a systematic review and meta-analysis of 15 RCTs and 1023 patients published in abstract form, treatment of patients with cirrhosis with LOLA resulted in benefit in the subgroup of patients with acute episodes or chronic HE but not in those with MHE .
Assessment Of The Need For Long
Patients with cirrhosis are at risk of developing new episodes of encephalopathy. Several factors need to be considered:
Diet and Nutrition
Low-protein diets are often erroneously recommended for patients with cirrhosis, in hopes of decreasing intestinal ammonia production and of preventing exacerbations of HE. An obvious consequence was the worsening of preexisting protein-energy malnutrition. Protein restriction may be appropriate in some patients immediately following a severe flare of symptoms . However, protein restriction is rarely justified in patients with cirrhosis and persistent HE. Indeed, malnutrition is a more serious clinical problem than HE for many of these patients.
It is the infrequent patient who is intolerant of a diet high in protein. Most patients with mild chronic HE tolerate more than 60 to 80 g of protein per day.
Diets containing vegetable proteins appear to be better tolerated than diets rich in animal protein. This may be because of increased content of dietary fiber, a natural cathartic, and decreased levels of AAA. AAA, as precursors for the false neurotransmitters tyramine and octopamine, are thought to inhibit dopaminergic neurotransmission and worsen HE. Ingestion of red meat protein should be discouraged.
Control of Potential Precipitating Factors
Higher Likelihood of Recurrent Encephalopathy
Patient Education
Assessment of the Need for Liver Transplantation
Hepatic Encephalopathy and Fitness to Drive
Specific Measures
You May Like: Is There Medicine For Hepatitis B
Laboratory Abnormalities In Hepatic Encephalopathy
An elevated blood ammonia level is the classic laboratory abnormality reported in patients with hepatic encephalopathy. This finding may aid in correctly diagnosing patients with cirrhosis who present with altered mental status. However, serial ammonia measurements are inferior to clinical assessment in gauging improvement or deterioration in a patient under therapy for hepatic encephalopathy. Checking the ammonia level in a patient with cirrhosis who does not have hepatic encephalopathy has no utility. Only arterial or free venous blood specimens must be assayed when checking the ammonia level. Blood drawn from an extremity to which a tourniquet has been applied may provide a falsely elevated ammonia level when analyzed.
Classic EEG changes associated with hepatic encephalopathy are high-amplitude low-frequency waves and triphasic waves. However, these findings are not specific for hepatic encephalopathy. When seizure activity must be ruled out, an EEG may be helpful in the initial workup of a patient with cirrhosis and altered mental status.
Visual evoked responses also demonstrate classic patterns associated with hepatic encephalopathy. However, this test is not in common clinical use.
V 46 No3 Jul/set 2009
Arq Gastroenterol
Sorez PC, Oliveira AC, Padovan J, Parise ER, Ferraz MB. A critical analysis of studies assessing L-ornithine-L-aspartate in hepatic encephalopathy treatment
RESULTS
Search results A total of 271 references was identified by electronic search in MEDLINE , PubMed and Cochrane Collaboration Register of Controlled Trials . No paper was found in LILACS and SciELO database. Fifty nine duplicate references and 145 references considered as irrelevant after reading the abstracts were excluded. From the remaining 67 references, 63 were excluded, 16 reviews, 1 letter to the editor, 7 abstracts , 1 presentation in congress, 14 other study design, 17 in another language and 7 clinical trials that have not met our inclusion criteria . Remaining references are four randomized, controlled clinical trials that met the inclusion criteria. Figure 1 shows the results from the search and Figure 2 describes the included studies.
You May Like: How To Treat Hepatitis A
Single Dose Kinetics In Healthy Humans
Intravenous administration LOLA 5 g in 250 mL 0.9% sodium chloride were administered intravenously to 10 healthy, fasting subjects over 30 min and blood levels of l-ornithine were measured at the end of infusion and hourly up to 24 h after infusion. A biphasic pattern was observed with a fast distribution phase and a slower terminal elimination phase . Peak levels of l-ornithine 30 min after the beginning of the infusion were nearly 10 times basal levels that fell to normal within 7 h. The median area under the curve for l-ornithine was 1.390 mmol/h/L .
Oral administration LOLA 5 g in 250 mL water were consumed by 10 healthy, fasting subjects and blood levels determined at the same intervals as the intravenous infusions . l-ornithine peaked within 3060 min to levels five times greater than basal concentrations and returned to baseline within 7 h. The median AUC for l-ornithine was 1.143 mmol/h/L. Bioavailability was 82.2±28% after IV or oral administration .
History Signs And Symptoms
Patients with HE usually have advanced chronic liver disease and thus have many of the physical and laboratory stigmata associated with severe hepatic dysfunction.
| The history may reveal a precipitating cause. These include: |
|---|
| Hypovolemia |
| Infection |
| Rarely, hepatocellular carcinoma and/or vascular occlusion |
Disturbance in the diurnal sleep pattern is common, and typically precedes overt neurologic signs. More advanced neurologic features include bradykinesia, asterixis . Hyperactive deep tendon reflexes are common seizures and hallucinations and transient decerebrate posturing may also be seen occasionally.
Read Also: How To Know If I Have Hepatitis