How Is Fatty Liver Disease Diagnosed
Because fatty liver disease often has no symptoms, your doctor may be the first one to spot it. Higher levels of liver enzymes that turn up on a blood test for other conditions may raise a red flag. Elevated liver enzymes are a sign your liver is injured. To make a diagnosis, your doctor may order:
- Ultrasound or computed tomography to get a picture of the liver.
- Liver biopsy to determine how far advanced liver disease has progressed.
- FibroScan®, a specialized ultrasound sometimes used instead of a liver biopsy to find out the amount of fat and scar tissue in the liver.
What Are The Treatments For Fatty Liver Disease
Doctors recommend weight loss for nonalcoholic fatty liver. Weight loss can reduce fat in the liver, inflammation, and fibrosis. If your doctor thinks that a certain medicine is the cause of your NAFLD, you should stop taking that medicine. But check with your doctor before stopping the medicine. You may need to get off the medicine gradually, and you might need to switch to another medicine instead.
There are no medicines that have been approved to treat NAFLD. Studies are investigating whether a certain diabetes medicine or Vitamin E can help, but more studies are needed.
The most important part of treating alcohol-related fatty liver disease is to stop drinking alcohol. If you need help doing that, you may want to see a therapist or participate in an alcohol recovery program. There are also medicines that can help, either by reducing your cravings or making you feel sick if you drink alcohol.
Both alcoholic fatty liver disease and one type of nonalcoholic fatty liver disease can lead to cirrhosis. Doctors can treat the health problems caused by cirrhosis with medicines, operations, and other medical procedures. If the cirrhosis leads to liver failure, you may need a liver transplant.
Signs And Symptoms Of Nonalcoholic Fatty Liver Disease
Initially, nonalcoholic fatty liver disease may have no symptoms at all. However, as the condition progresses, it may start to exhibit symptoms. Here are a few signs and symptoms of fatty liver disease:
- Fatigue
- Unexplained weight loss
- Pain in the upper right quadrant of your abdomen
If nonalcoholic liver disease progresses to more serious conditions, it can cause more severe symptoms like ascites, jaundice, muscle wasting, and hepatic encephalopathy.
Keep in mind that fatty liver disease rarely occurs in isolation. Metabolic conditions are significant risk factors for developing fatty liver disease. Metabolic syndrome includes conditions like insulin resistance, type 2 diabetes, elevated triglycerides, and high cholesterol. Fatty liver disease is also correlated with obesity and hypertension.
Read Also: How Do You Get Hepatitis A B C
Clinical Characteristics Of The Study Cohort
We recruited 53 patients with NAFLD and 17 healthy volunteers. However, three patients had histological and clinical features of concomitant autoimmune or cholestatic liver disease. Two control cases showed signs of liver disease and were excluded. Therefore, 50 patients with NAFLD and 15 healthy controls were included in the final analysis.
Patients with NAFLD were classified by a single expert pathologist according to the histological degree of steatosis: 18, 20, and 12 cases had mild , moderate , and severe steatosis, respectively , . Fibrosis staging revealed F0, F1, F2, F3, and F4 fibrosis in 10, 32, 2, 3, and 3 cases. The associations between CAP, 1H-MRS and histology were essentially unaffected by the age of the biopsy .
Clinical characteristics of the study cohort are presented in table 1. Gender distribution did not differ significantly between the three NAFLD subgroups and only slight differences in age were observed. Time span since liver biopsy did not differ significantly. NAFLD cases with mild steatosis had a lower prevalence of hepatocellular inflammation , arterial hypertension , and a trend towards a lower prevalence of diabetes mellitus type 2 compared to patients with more advanced steatosis . Moreover, S2 and S3 patients had a higher frequency of the non-CC PNPLA3 genotype and a trend towards a higher risk profile according to the NAFLD score .
What Questions Should I Ask My Doctor
- Am I taking any medications that could contribute to fatty liver disease?
- How much damage does my liver have?
- How long will it take to reverse the liver damage?
- What is a healthy weight for me?
- Can I talk to a nutritionist or go to classes to learn about healthy eating?
- How can I get treatment for alcohol use disorder?
A note from Cleveland Clinic
Consider fatty liver disease an early warning sign to help you avoid a fatal liver condition, like cirrhosis or liver cancer. Even if you dont have symptoms or any liver function problems at this point, its still important to take steps to stop or reverse fatty liver disease.
Also Check: Ok Google How Do You Get Hepatitis C
Exercise Diet And Prevention Of Hepatic Steatosis
Low levels of habitual physical activity and/or poor fitness are routinely linked to increased NAFLD prevalence.- NAFLD patients are known to have lower amounts of daily physical activity than patients without fatty liver disease. Less physically active individuals also exhibit higher rates of hepatic FFA uptake compared with more active individuals, a factor known to significantly contribute to hepatic steatosis., In addition, a recent study in monozygotic twin pigs found that the more active pig in each pair had 18% greater maximal oxygen uptake and approximately 25% less hepatic fat content than the less active animal. Furthermore, a recent retrospective cross-sectional study suggests that meeting the recommendations for vigorous physical activity is associated with a significant reduction in the odds of hepatic steatosis progressing to NASH and that exceeding the vigorous activity guidelines is associated with decreased odds of having fibrosis. Interestingly, meeting or exceeding the recommendations for moderate intensity activity was not associated with a reduced incidence of NASH or fibrosis. This retrospective analysis points to the potential clinical utility of vigorous, high-intensity exercise training in the management of NASH, but randomized clinical trials are necessary.
Expression Of The Fatty Liver Disease Gene Depends On Environment
Your DNA an abbreviation short for deoxyribonucleic acid is a code that makes you human and determines your individual traits. Some traits, such as eye color, are influenced by just two genes and based on your inherited genes, will remain set in stone for your lifetime.
Other traits, such as personality, are much more complex and described as polygenic traits since they are influenced by a large number of different genes. An individuals personality like introversion or open-mindedness is highly influenced by both genes and the environment. For example, a naturally introverted child may become more extroverted over time in response to positive experiences with family and peers.
The expression of the genes contributing to fatty liver disease is comparable to more complex traits, like personality. Inheriting certain forms of the gene may predispose you to fatty liver disease under certain environmental conditions.
Don’t Miss: What Are The Early Symptoms Of Hepatitis C
Metabolic Syndrome And Fatty Liver Disease
Many researchers now believe that metabolic syndrome a cluster of disorders that increase the risk of diabetes, heart disease and stroke plays an important role in the development of fatty liver.Signs and symptoms of metabolic syndrome include:
- obesity, particularly around the waist
- high blood pressure
- one or more abnormal cholesterol levels high levels of triglycerides, a type of blood fat, or low levels of high-density lipoprotein cholesterol, the good cholesterol
- resistance to insulin, a hormone that helps to regulate the amount of sugar in the blood.
Of these, insulin resistance may be the most important trigger of NASH. Because the condition can remain stable for many years, causing little harm, researchers have proposed that a second hit to the liver, such as a bacterial infection or hormonal abnormality, may lead to cirrhosis.
Molecular Sieves And Desiccants
Apart from distillation, ethanol may be dried by addition of a , such as , , or . The desiccants can be dried and reused. can be used to selectively absorb the water from the 95.6% ethanol solution. Molecular sieves of pore-size 3 , a type of , effectively sequester water molecules while excluding ethanol molecules. Heating the wet sieves drives out the water, allowing regeneration of their dessicant capability.
Also Check: Is Hepatitis B The Same As Hiv
Steatosis And Fibrosis Progression In Hcv
High levels of TNF- have also been observed in human chronic hepatitis C patients. TNF- has been shown to induce IR in experimental animals and cultured cells. Inhibition of tyrosine phosphorylation of IRS 1 and 2 may be one of the mechanisms by which a high level of TNF- causes IR. Administration of an anti-TNF- antibody restores insulin sensitivity. These results provide direct experimental evidence for the contribution of HCV in the development of IR. There are experimental arguments for a direct role of insulin in fibrosis progression in HCV infection.
Epidemiological studies indicating that the state of IR now associated with NASH is also associated with an increased risk of HCC. It is worth mentioning that diabetes increases the risk of chronic liver disease and HCC.
Membranes And Reverse Osmosis
Membranes can also be used to separate ethanol and water. Membrane-based separations are not subject to the limitations of the water-ethanol azeotrope because the separations are not based on vapor-liquid equilibria. Membranes are often used in the so-called hybrid membrane distillation process. This process uses a pre-concentration distillation column as the first separating step. The further separation is then accomplished with a membrane operated either in vapor permeation or pervaporation mode. Vapor permeation uses a vapor membrane feed and pervaporation uses a liquid membrane feed.
You May Like: Treatment To Cure Hepatitis C
Determination Of Glucose Metabolism Levels In Other Organs
The left ventricular myocardial ROI was delineated layer by layer on the tomographic PET/CT fusion images. The SUVmean of 18F-FDG in the entire left ventricular myocardium was automatically calculated by Siemens TrueD software. Because the glucose uptake of the myocardium was affected by a variety of metabolic substrates, the value varied greatly. For subjects with low myocardial uptake as a blood pool, an ROI with double U-shaped lines with about 1cm distance was delineated along the border of the left ventricle on the transaxial PET/CT images . The ROI of the mediastinal blood pool was delineated on the continuous layers of the ascending aorta. In the pancreas, three ROIs with a diameter of 1.0cm were delineated in the pancreatic head, body and tail and used to calculate the SUVmean of the pancreas. The ROI of skeletal muscle was delineated on the upper part of the bilateral femur .
Prevention Of Hepatic Steatosis
A negative by-product of our modern civilization is little need for physical activity and an increased risk of chronic disease, such as heart disease, insulin resistance, type 2 diabetes, and NAFLD. Physical inactivity is one of the causes of these associated metabolic disorders and is an actual known leading cause of death in the United States.-
Recommended Reading: How Does One Get Hepatitis C
Steatosis In Chronic Hepatitis C
In chronic hepatitis C patients, the prevalence of steatosis ranges from 40% to 86% . The majority of patients with steatosis have mild steatosis affecting less than 30% of hepatocytes. Thus, steatosis occurs more frequently in patients with chronic hepatitis C than in the general population of adults in the Western world. Macrovesicular steatosis is found in the periportal region of the liver-different from the centrilobular distribution characteristic of NASH patients. Mild steatosis had been reported in nearly 40% of patients with HCV genotype 4.
Moderate or severe steatosis is significantly less frequent in genotype 4 than 3 chronic hepatitis C patients and similar between genotype 4 and 1. In non-diabetic, overweight patients, moderate or severe steatosis is present in only 10%-15% of genotype 4 or 1 compared with 40% of genotype 3 patients. Thus, hepatic steatosis in genotype 4 is mostly associated with metabolic factors, similar to those in genotype 1.
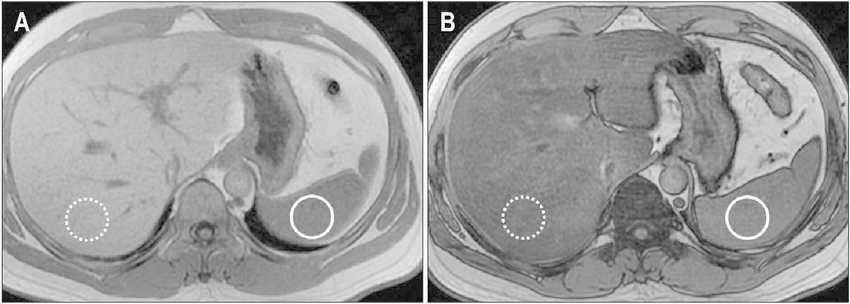
Magnetic Resonance Spectroscopy And Volumetry
MR examinations were performed on a 1.5-T scanner with the patient in supine position. Single-voxel MR spectra were acquired with the integrated body coil using a point-resolved spectroscopy technique and local shimming. Voxels were placed in the right liver lobe trying to avoid bile ducts and larger vessels. Scans were acquired during free breathing with the following sequence parameters: repetition time, TR=3,500 ms, echo time, TE=25 ms, 512 data points, bandwidth, BW=1,000 Hz/pixel, 40 averages, total acquisition time, TA=140 s, and without water suppression.
MR spectra were analyzed with a commercial tool that uses an optimized set of basis functions to determine the relative concentrations of hepatic lipids . Calculated peak areas of water and fat were corrected for T2 relaxation applying previously published literature values and were used to calculate the liver fat content according to the ratio LFC = Sfat/ with Sfat as the sum of the areas under the methyl , methylene and allylic peaks and Swater as the area under the water peak .
You May Like: How Does One Get Hepatitis B And C
Hepatic Steatosis Hepatic Resection And Liver Transplantation
Macrovesicular steatosis is an important criterion defining extended-criteria donor organs. Several studies have reported a poor impact of steatosis on postoperative morbidity and mortality after liver resection. A national analysis of the Scientific Registry of Transplant Recipients demonstrated that macrovesicular steatosis of greater than 30% was an independent predictor of reduced 1-year graft survival. Steatotic livers are particularly vulnerable to ischemia/reperfusion injury, resulting in an increased risk of postoperative morbidity and mortality after liver surgery, including liver transplantation. In a retrospective review of 450 living liver donors who underwent right hepatectomy, a mild degree of hepatic steatosis was associated with higher postoperative peak aspartate and alanine aminotransferase values. Furthermore, biliary complications remain a persistent problem in orthotopic liver transplantation. The presence of macrovesicular steatosis in 20% to 50% of a liver graft emerged as a newly defined risk factor for postoperative biliary complications in 175 adult patients undergoing living donor liver transplantation. Thus, hepatic steatosis poses a challenge after liver resection or transplantation.
What Is Alcoholic Fatty Liver Disease
Alcoholic fatty liver disease is due to heavy alcohol use. Your liver breaks down most of the alcohol you drink, so it can be removed from your body. But the process of breaking it down can generate harmful substances. These substances can damage liver cells, promote inflammation, and weaken your body’s natural defenses. The more alcohol that you drink, the more you damage your liver. Alcoholic fatty liver disease is the earliest stage of alcohol-related liver disease. The next stages are alcoholic hepatitis and cirrhosis.
Read Also: Is Viral Hepatitis C Contagious
Fatty Liver Disease Has A Genetic Component
The likelihood of developing fatty liver disease is influenced in part by genetics. But the heritability of fatty liver is not so simple to determine. Research has shown that there is not just one gene that determines the risk of developing fatty liver disease, but rather an interaction of many genes in your DNA.
Research published in Clinical and Molecular Hepatology describes three genes PNPLA2, GCKR, and TM6SF2 that may influence the likelihood of fat accumulation in the liver. Specific variants of each gene are associated with increased risk of conditions associated with fatty liver disease, such as insulin resistance and type 2 diabetes. Of the three genes, PNPLA3 is the most well-studied gene and directly plays a role in liver metabolic processes. Moreover, a certain variant of the PNPLA3 gene is associated with a higher risk of fatty liver disease progression to NASH, fibrosis, and cirrhosis.
Is Mild Hepatomegaly Serious
Rather than a disease in itself, hepatomegaly is a symptom or complication of other liver conditions, some of them life-threatening. For this reason, hepatomegaly is something to take seriously, as it points to an underlying problem that could be quite serious. Liver disease can develop for years with no overt symptoms at all.
Also Check: Hepatitis B And Rheumatoid Arthritis Treatment
Ultrasound Grade Of Liver Steatosis Is Independently Associated With The Risk Of Metabolic Syndrome
Ivica Grgurevic
1Department of Gastroenterology, Hepatology and Clinical Nutrition, University Hospital Dubrava, University of Zagreb School of Medicine, Zagreb, Croatia
2Department of Emergency Medicine, University Hospital Dubrava, University of Zagreb School of Medicine, Zagreb, Croatia
3Faculty of Pharmacy and Biochemistry, University of Zagreb, Croatia
4Department of Hematology, University Hospital Dubrava, Zagreb, Croatia
5Department of Endocrinology and Clinical Pharmacology, University Hospital Dubrava, University of Zagreb School of Medicine, Zagreb, Croatia
Abstract
1. Introduction
Therefore, the main goals of our study were to assess the prevalence and grade of NAFLD among the cohort of outpatients referred for an US examination and to explore the relationship between the presence and severity of liver steatosis and MS.
2. Patients and Methods
2.1. Study Population
In this study, retrospective analysis was performed over the cohort of consecutive outpatients examined by 3 experienced ultrasonographers in the US Unit of the University Hospital Department of Gastroenterology during a 5-month period.
2.2. US Assessment
2.3. Statistical Analysis
3. Results
3.1. Demographic Characteristics of Study Participants
| Age |
What Are The Forms Of Fatty Liver Disease
There are two main forms of fatty liver disease:
Alcoholic liver disease
Alcoholic fatty liver is the accumulation of fat in the liver as a result of heavy drinking. About 5% of people in the U.S. have this form of liver disease.
Nonalcoholic fatty liver disease
Nonalcoholic fatty liver disease occurs in people who arent heavy drinkers. The condition affects one in three adults and one in 10 children in the United States. Researchers havent found the exact cause of nonalcoholic fatty liver disease. Several factors, such as obesity and diabetes, can increase your risk.
Don’t Miss: What Does Hepatitis B Do
Why Is Fatty Liver Disease Bad
In most cases, fatty liver disease doesnt cause any serious problems or prevent your liver from functioning normally. But for 7% to 30% of people with the condition, fatty liver disease gets worse over time. It progresses through three stages:
Your liver becomes inflamed , which damages its tissue. This stage is called steatohepatitis.
Scar tissue forms where your liver is damaged. This process is called fibrosis.
Extensive scar tissue replaces healthy tissue. At this point, you have cirrhosis of the liver.
Cirrhosis of the liver
Cirrhosis of the liver is a result of severe damage to the liver. The hard scar tissue that replaces healthy liver tissue slows down the livers functioning. Eventually, it can block liver function entirely. Cirrhosis can lead to liver failure and liver cancer.