How Is Fatty Liver Treated And Is It Reversible
Currently, no medications have been approved to treat fatty liver disease. More research is needed to develop and test medications to treat this condition.
In many cases, lifestyle changes can help reverse most stages of fatty liver disease. For example, your doctor might advise you to:
- limit or avoid alcohol
- take steps to lose weight
- make changes to your diet
- avoid medications and supplements that are hard on your liver
If you have AFLD, your doctor will instruct you to completely abstain from alcohol. They may also recommend a detoxification program and counseling if you have alcohol use disorder .
Several viral infections can also damage the liver. To protect your liver health, your doctor may advise you to receive vaccines for hepatitis A and hepatitis B. Depending on your situation, they may also recommend regular screenings for hepatitis C.
Cirrhosis can also cause a variety of complications, including:
- portal hypertension, which is when blood pressure in the portal vein of the liver is too high
- an increased risk of infections
If youve developed complications from cirrhosis, your doctor might recommend additional treatments, such as medications or surgery.
Cirrhosis can also lead to liver failure. If you develop liver failure, you might need a liver transplant.
Lifestyle changes are the first-line treatment for fatty liver disease. Depending on your current condition and lifestyle habits, it might help to:
For example, they might advise you to do the following:
Causes Of Hepatic Steatosis
Steatosis of the liver occurs due to metabolic disorders in diabetes mellitus, obesity, etc. Also, steatosis can be associated with diseases of the digestive system, resulting in impaired absorption of nutrients, as well as malnutrition .
Alcohol and medications have a strong toxic effect on the liver, which can also cause stethatosis.
Fatty liver poisoning is not due to alcohol abuse is called non-alcoholic steatosis, a similar pathology often affects people with excess weight.
Steatosis is most affected by women, people with excess weight, over 45, with type 2 diabetes, and also in the case of hereditary predisposition.
, , , , , , , , ,
Metabolic Syndrome And Fatty Liver Disease
Many researchers now believe that metabolic syndrome a cluster of disorders that increase the risk of diabetes, heart disease and stroke plays an important role in the development of fatty liver.Signs and symptoms of metabolic syndrome include:
- obesity, particularly around the waist
- high blood pressure
- one or more abnormal cholesterol levels high levels of triglycerides, a type of blood fat, or low levels of high-density lipoprotein cholesterol, the good cholesterol
- resistance to insulin, a hormone that helps to regulate the amount of sugar in the blood.
Of these, insulin resistance may be the most important trigger of NASH. Because the condition can remain stable for many years, causing little harm, researchers have proposed that a second hit to the liver, such as a bacterial infection or hormonal abnormality, may lead to cirrhosis.
Recommended Reading: What Is Hepatitis C Antibody Mean
Read Also: Hepatitis C Antibodies In Blood
The Four Stages Of Non
Non-alcoholic Fatty Liver Disease describes a range of conditions caused by too much fat stored in the liver in people who drink little or no alcohol. Healthy liver cells should contain little or no fat. More than 5% fat stored in liver cells is considered too much, and this can result in a fatty liver. 1 in 3 people in the UK is estimated to be affected by NAFLD.
There are four stages of Non-Alcoholic Fatty Liver Disease .
Simple fatty liver or steatosis
Non-alcoholic steatohepatitis
The first stage is referred to as simple fatty liver or steatosis
This occurs when the liver cells start to build-up fat, although there is no inflammation or scarring at this stage. There are often no symptoms in this early stage, so many people are unaware they have a fatty liver. For many people, fatty liver does not develop any further, and with a healthy diet and regular exercise, the excess fat in liver cells can be reduced. It is thought that approximately 20% of people with simple fatty liver, will go on to develop non-alcoholic steatohepatitis or NASH.
The second stage of NAFLD is non-alcoholic steatohepatitis
The third stage of NAFLD is fibrosis
The fourth stage of NAFLD is cirrhosis
Who Will Manage My Care
GPs manage care for earlier stage NAFLD
This can include fatty liver and NASH with mild or moderate fibrosis.
Your liver has little or no long-term damage or scarring and is probably still working well. By eating healthily, doing plenty of physical activity and keeping your weight in a healthy range you have a good chance of repairing any damage and reversing your NAFLD.
Your doctor or nurse will have a conversation with you about your weight, the foods you eat, and how physically active you are. Theyll give you information and help you decide and plan the changes you want to make.
The aim is to build healthy habits that will fit in with your life and help you stay well in the future.
You should have a check-up for NAFLD at least once a year. This should include checks on your risk of developing a condition related to NAFLD.
Your GP can check your:
- weight and body mass index
Every 3 years you should have testing for advanced fibrosis. This is to check that your condition is stable and not getting worse. This is important because there are often no symptoms to tell you or your clinical team that your liver is getting more damaged.
Hospital specialists manage care for later stage NAFLD
This can include NASH with moderate or advanced fibrosis, and cirrhosis.
Your MDT are there to give you any help you need to improve your NAFLD. They can also help you to manage some other medical conditions alongside your NAFLD. Your MDT could include:
Also Check: How Long Can You Live With Hepatitis C
What Are The Stages Of Nafld
There are several stages of NAFLD. Having one stage does not mean you will definitely develop the next one. Treating NAFLD with a healthy diet, physical activity and weight loss can slow or even reverse your NAFLD especially if it is at an earlier stage.
The amount of scarring in your liver is the main sign of how advanced your NAFLD is. Go to the section about fibrosis tests and scores.
- Fatty liver : There is a build-up of fat in your liver but it has not been damaged and there is no scarring. At this point, NAFLD can be fully reversed.
- NASH with mild fibrosis : Fat is causing inflammation and damage in your liver . There is no or very little scarring. Healthy living can undo the damage and reverse your NAFLD.
- NASH with moderate fibrosis : Inflammation and damage have caused some scarring. Your liver is probably still working well and the damage can mostly be repaired.
- NASH with advanced fibrosis : There is a lot of scarring. At this stage it is very important to stop further damage and scarring so your NAFLD doesnt get worse. And it is still possible to repair some damage.
- Cirrhosis : There is so much scarring it changes the shape of your liver. Your liver can keep working and even repair some damage at this point. But if too much of it becomes scarred, your liver may not be able to carry out its job properly.
Cirrhosis can lead to life-threatening conditions including liver cancer and liver failure.
Type 2 Diabetes And Nash
Type 2 diabetes influences the relationship between NAFLD/NASH and cardiovascular disease. According to research, NAFLD was found in 50% of patients with type 2 diabetes who had an otherwise healthy liver. In addition, NAFLD/NASH-related cardiovascular issues are nearly twice as likely in individuals with type 2 diabetes.
NAFLD/NASH and type 2 diabetes share many of the same risk factors: inactivity, obesity, genetics and environmental factors all add to the occurrence of these diseases. In addition, people with type 2 diabetes are at greater risk of advanced fibrosis, which is a major indicator of NASH.
While serious, the good news is that the same measures to help prevent and treat type 2 diabetes eating healthier, exercise, weight management can improve NAFLD and NASH prognosis.
Don’t Miss: How To Get Rid Of Hepatitis B
Symptoms And Treatments For High Iron
Overview of High Iron High iron, a condition known as hemochromatosis, is when the body absorbs too much iron from the foods. The excess iron usually accumulates in the organs, including the liver, heart, and pancreas. When iron stores overtime in these vital organs, it can lead to life-threatening conditions,
Also Check: Hepatitis C How Is It Transmitted
Living With Fatty Liver Disease
If you are living with fatty liver disease, learn as much as you can about your condition and work closely with your medical team. Since many medications can harm your liver, always let all your health care providers know about any medications you are taking. These include OTC drugs, dietary supplements, and vitamins. Other ways to manage fatty liver disease include maintaining a healthy weight, eating a balanced diet, getting regular exercise, and continuing to avoid alcohol.
You May Like: Can You Get Hepatitis From Saliva
Also Check: Hepatitis A Vs B Vs C
Maintain A Healthy Weight
Sticking to a healthy, plant-based diet and getting regular exercise can keep fat from building up in your liver. Thats because the major risk factors for NAFLD are obesity and diabetes, both of which are tied to our weight.
Its estimated that rates of NAFLD may be 90% in obese people and 50% in people with diabetes. Because obesity and diabetes are so prevalent in developed countries, approximately 30% of adults in the developed world have NAFLD. Fortunately, some of this damage appears to be reversible if you take off the extra pounds.
If you are overweight or obese, the American College of Gastroenterology advises that losing 10% of your body weight will have a positive impact on your liver.
Also Check: Hepatic Artery Infusion Survival Rate
What Does Diagnosis Look Like
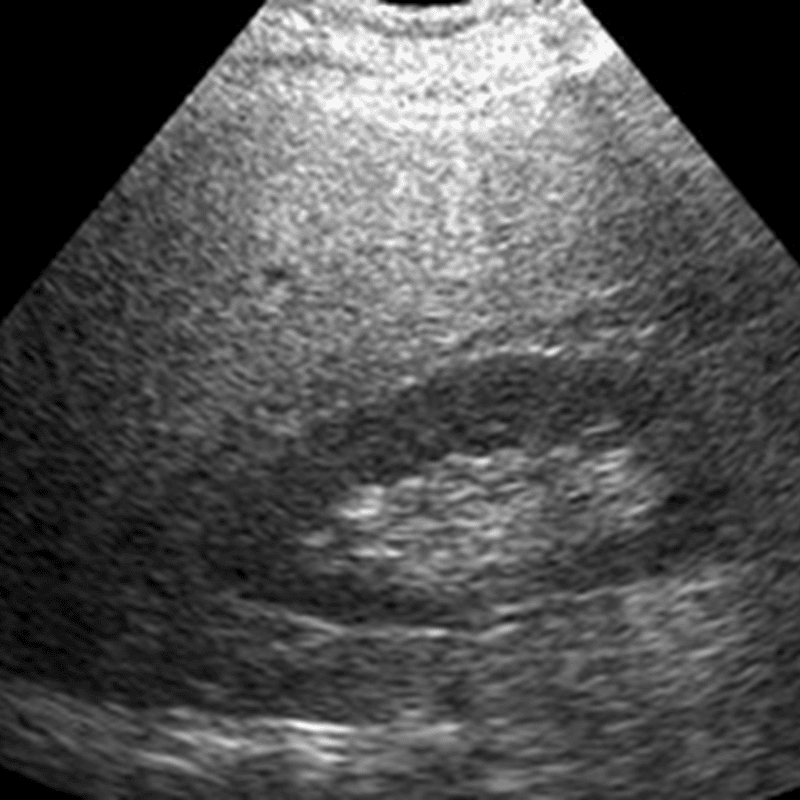
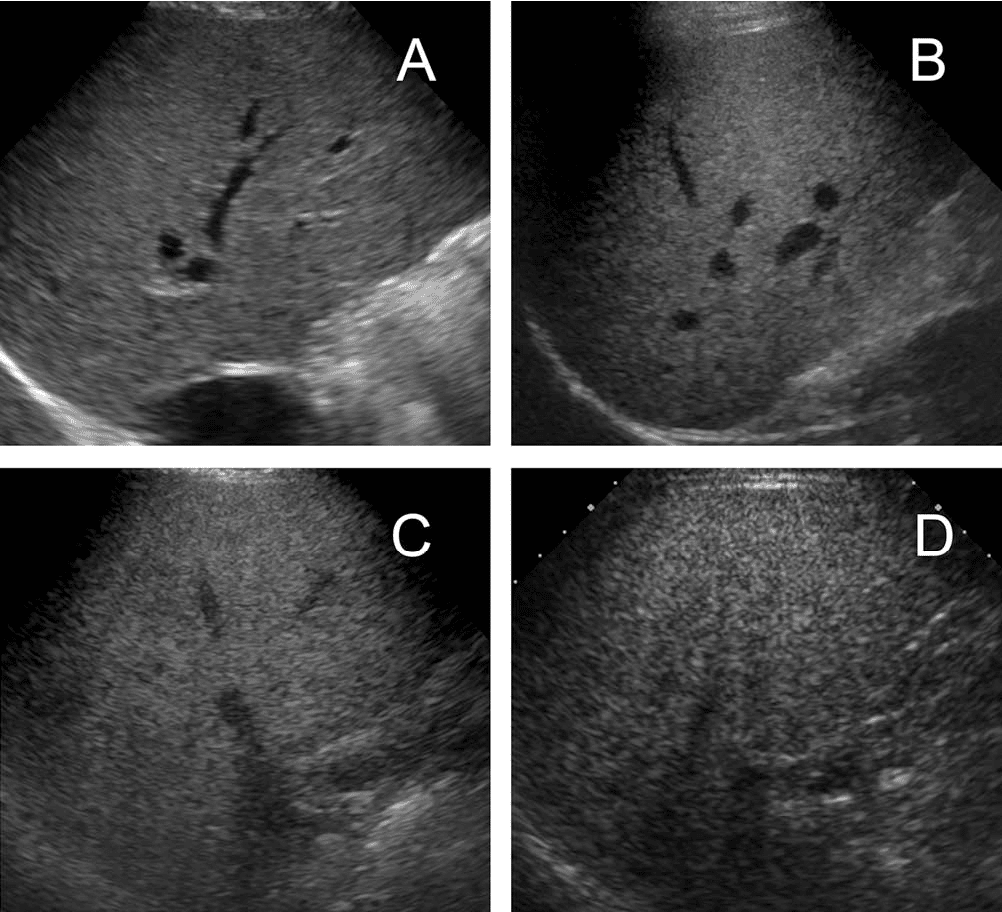
Hepatic steatosis can often be diagnosed by imaging techniques, such as ultrasound, computed tomography scan, or magnetic resonance imaging . All types of medical imaging can reveal diffuse fat content in the liver. This finding may also be described as lower liver attenuation, which means that healthy tissue is interrupted by fatty deposits. Imaging tests are performed by radiology specialists and interpreted by radiologists.
Ultrasound imaging is a type of sonography that is useful for detecting fat within the liver. Ultrasound technology utilizes sound waves to detect variations in structures and composition within body tissues. A higher measure of echogenicity will also accompany fat deposits in the liver parenchyma, which is the part of the liver responsible for carrying out the organs processes. Higher echogenicity means that sound waves more readily bounce off fat tissue and echo back to their source. An MRI might reveal a chemical shift that signifies the presence of fat within the liver.
Another type of imaging is called elastography. Elastography can reveal if soft tissue has hardened, indicating damage. For example, normally functioning liver tissue is soft in texture. Scarred or damaged liver becomes harder in texture.
One of the most definitive ways to detect and diagnose fatty liver disease is through a liver biopsy. A liver biopsy requires taking a tiny sample of your liver and analyzing it for the presence of fat cells, lesions, and other abnormalities.
Read Also: What Is The Cure Of Hepatitis B
What Are The Forms Of Hepatic Steatosis
Hepatic steatosis especially occurs in two forms:
Alcoholic Liver Disease : Excess consumption of alcohol leads to this state where alcoholic fatty liver occurs due to the accumulation of fat. Around 5% of people in the U.S are affected by this form of hepatic steatosis.
Nonalcoholic Fatty Liver Disease : Non-alcoholic individuals are affected by this condition. This can be further classified into the non-alcoholic fatty liver and non-alcoholic steatohepatitis . NAFLD occurs in one in three adults and one in 10 children in the US. The exact cause of this condition is still unknown. Many factors are linked to this condition, like obesity and diabetes, which can, in turn, increase the risk of having NAFLD.
Fatty Liver Disease Symptoms
Now that you know what is fatty liver, its time to take a look at some of the ways you can identify this disease by knowing the common nonalcoholic fatty liver disease symptoms. First, its important to note that it is possible to have non-alcoholic fatty liver disease and exhibit no symptoms. This is actually quite common. When symptoms do occur, there are several possibilities.
Signs of a fatty liver can include:
- A build up of fluid and swelling of the legs and abdomen
- Mental confusion
Read Also: Best Medication For Hepatitis C
Don’t Miss: Where Can I Get A Hepatitis A Shot
Lose Weight If Needed
Losing weight can help you reverse fatty liver disease. When you lose fatty tissue, this also means that you are losing fat from your liver.
To facilitate weight loss, aim to create a calorie deficit, meaning you are burning more energy than you consume. Eating healthy foods, controlling portion sizes, and exercising help encourage weight loss.
Make sure that you follow a balanced diet to lose weight, instead of following extreme diet plans. In addition to losing fat, its essential to also maintain muscle mass.
Alcoholic Steatosis Of The Liver
Alcoholic steatosis of the liver is caused by chronic alcohol intoxication and leads to initial changes in the structure of the liver.
The disease can occur for several reasons, the most common is the abuse of alcohol, while the more and more a person drinks, the faster and heavier the pathological process in the liver.
Such manifestations of steatosis are usually reversible and decline one month after the person stops drinking.
But, despite this, alcoholic steatosis of the liver progresses and leads to serious damage to the body. According to clinical studies, the threat of developing chronic liver diseases is associated with steatosis.
, , , , ,
Don’t Miss: Current Treatment For Hepatitis B
How Is Nafld Treated
Treatment for NAFLD has 2 main aims:
- To stop the condition getting worse, so that it does not lead to liver cancer or liver failure.
- To help your liver repair as much of the damage as possible and reverse your NAFLD.
The main treatment for NAFLD is eating a healthy diet, being more physically active and losing weight. This might seem like very general advice, but these steps all reduce liver fat and inflammation. For example, for people who are overweight, evidence shows losing 5 to 10% of their bodyweight can stop and sometimes even reverse liver damage.
There are currently no medicines to specifically treat NAFLD. But there is a lot of research being done to develop some. You can help by taking part in research. Ask your clinical team about clinical trials in your area or visit the Be Part of Research website.
How your care is managed depends on how serious your NAFLD is and how much scarring there is in your liver.
Ways To Reverse A Fatty Liver
Fatty liver occurs when excess fat accumulates inside liver cells. This means normal, healthy liver tissue becomes partly replaced with fatty tissue. The fat starts to invade the liver, gradually infiltrating the healthy liver areas, so that less and less healthy liver tissue remains. The fatty liver has a yellow greasy appearance and is often enlarged and swollen with fat.
Fatty liver is now recognised as the most common cause of abnormal liver function test results in the USA, UK and Australia. Around one in five people in the general population, in the USA and Australia has a fatty liver. Fatty liver is usually associated with abdominal obesity, insulin resistance and type 2 diabetes. If severe, it can eventually lead to cirrhosis and liver failure.
Read Also: Can Hepatitis C Cause Fatty Liver
Also Check: Colloidal Silver And Hepatitis C
Fibrosis Tests And Scores
It is very important that the amount of scarring in your liver is tested as part of your NAFLD diagnosis. This is the main sign of how advanced your liver disease is.
Fibrosis is the medical term for scarring. It is measured on a scale of 0 to 4. The higher the number, the more fibrosis there is and the more severe it is.
There are 2 main ways to check if youre likely to have advanced fibrosis without doing a biopsy blood tests or a liver scan .
Many doctors use a scoring system that pools results from several routine blood tests. Common fibrosis scoring systems include:
- The Fibrosis -4 score which uses 3 blood tests and your age
- The NAFLD Fibrosis Score which uses 4 blood tests and information about your age, weight and whether you have diabetes
- The Enhanced Liver Fibrosis test which uses a combination of 3 blood tests.
The score doesnt say exactly how much scarring there is in your liver. Your doctor or nurse will interpret the result to decide what to do.
There are 3 possible results:A low risk means advanced fibrosis can be safely ruled out.
This means you dont have later stage NAFLD including cirrhosis. Your GP will continue to manage your care. They should do a fibrosis test every 3 years to check your condition hasnt got worse.
Indeterminate risk means it doesnt say for sure whether you have advanced fibrosis or not.
You should be offered further tests to find out. These could include scans or a liver biopsy.
Prevention And Reversal Of Fatty Liver Disease
There are no medical or surgical treatments for fatty liver, but some steps may help prevent or reverse some of the damage.In general, if you have fatty liver, and in particular if you have NASH, you should:
- lose weight safely. This usually means losing no more than half to one kilogram a week
- lower your triglycerides through diet, medication or both
- control your diabetes, if you have it
- eat a balanced, healthy diet
- increase your physical activity
Also Check: Can You Live A Normal Life With Hepatitis C