Who Should Get Tested Or Hepatitis C
-
All Baby-Boomers need to be tested for hepatitis C. These are individuals born between 1945-1965. You need to get tested regardless of risk factors.
-
Persons who ever injected illegal drugs, including those who injected once or twice many years ago
-
Persons who were treated for clotting problems with a blood product made before 1992 when more advanced methods for manufacturing the products were developed
-
Persons who were notified that they received blood from a donor who later tested positive for hepatitis C
-
Persons who received a blood transfusion or solid organ transplant before July 1992 when better testing of blood donors became available
-
Long-term hemodialysis patients
-
Persons who have signs or symptoms of liver disease
-
Healthcare workers after exposures to HCV positive blood on the job
-
Children born to HCV-positive women
-
Homosexual men or women
- New recommendations from the Centers for Disease control state that all “Baby Boomers” get tested, regardless of their HCV risk factors. Baby Boomers were born between 1945-1965. Baby Boomers, as a group, are five times more likely to have HCV. Many have no symptoms, so they need to ask to be tested for HCV-do not assume you will be tested by your physician.
- This video by Dr. Galati outlines some of the Baby Boomer issues related to HCV.
How Can You Reduce Liver Inflammation
It is possible to reduce liver inflammation, and there are a couple of things you can do. The most effective way aside from pharmacological treatment is the change of lifestyle to have a healthy liver.
Dietary changes are the first to be taken into consideration the diet should be based on the food pyramid here are some products you should include:
- Low sugar or sugar-free foods
- Complex carbohydrates in the form of low-processed cereal products, like oatmeal, brown rice, beans, quinoa, and whole-grain bread.
- Vegetables
- Food that is rich in antioxidants like broccoli, pecans, spinach, berries, and artichoke.
- Protein-rich products
Also, avoiding alcohol, drugs, and processed products with a high content of fat or sugar will reduce the inflammation. Therefore, in order to help the liver, the exercise provides the fat loss and helps the liver in its recovery process.
How Can A Person Protect Themselves From Getting Hepatitis C And Other Diseases Spread By Contact With Human Blood
-
Don’t ever shoot drugs. Intranasal is also a risk factor. If you shoot or inhale drugs, stop and get into a treatment program. If you can’t stop, never reuse or share syringes, water, or drug works, and get vaccinated against hepatitis A and hepatitis B.
-
Do not share toothbrushes, razors, or other personal care articles. They might have blood on them.
-
If you are a healthcare worker, always follow routine barrier precautions and safely handle needles and other sharps. Get vaccinated against hepatitis B
-
Consider the health risks if you are thinking about getting a tattoo or body piercing: You can get infected if:
-
the tools that are used have someone else’s blood on them.
-
the artist or piercer doesn’t follow good health practices, such as washing hands and using disposable gloves.
HCV can be spread by sex, but this does not occur very often. If you are having sex, but not with one steady partner:
-
You and your partners can get other diseases spread by having sex .
-
You should use latex condoms correctly and every time. The efficacy of latex condoms in preventing infection with HCV is unknown, but their proper use may reduce transmission.
-
You should get vaccinated against hepatitis B.
Also Check: How Does A Person Get Hepatitis C
Who Should Get Tested For Hepatitis C
The CDC recommends that you get tested at least once no matter what. Definitely get screened if any of these things apply to you:
- You were born between 1945 and 1965.
- You use or inject drugs.
- You have ever injected drugs — even if it was just once or a long time ago.
- Youâre on kidney dialysis.
- You have abnormal alanine aminotransferase levels .
- You had a blood transfusion, blood components, or an organ transplant before July 1992.
- Youâve ever gotten clotting factor concentrates made before 1987.
- You received blood from a donor who later tested positive for hepatitis C virus.
- Youâre a health care worker, first responder, or have another job that exposes you to HCV-infected needles.
- You were born to a mother with HCV.
Additional Tests You Might Need
Once youve been diagnosed with Hepatitis C, your doctor will likely order a number of tests to find out about the health of your liver and decide on a treatment plan thats most appropriate for you.
Hepatitis C genotype
The Hepatitis C genotype refers to a specific strain or type of the Hepatitis C virus. There are six major types of Hepatitis C around the world: genotypes 1, 2, 3, 4, 5 and 6. In the United States, genotypes 1, 2, and 3 are common:
- Genotype 1: Most Americans with Hepatitis C have this type
- Genotype 2: About 10% of Americans with Hepatitis C have this type
- Genotype 3: About 6% of Americans with Hepatitis C have this type
The genotype of Hepatitis C does not change over time, so you only need to get tested once.
Genotype tests are done before a person starts treatment. Hepatitis C treatment works differently for different genotypes, so knowing your genotype helps your doctor choose the best treatment for you.
Testing for Hepatitis A and Hepatitis B
Your doctor may test to see if your body is immune to Hepatitis A and Hepatitis B. If these tests show no prior exposure or protection, he or she will recommend that you be vaccinated against these two viruses to eliminate the chance of becoming infected.
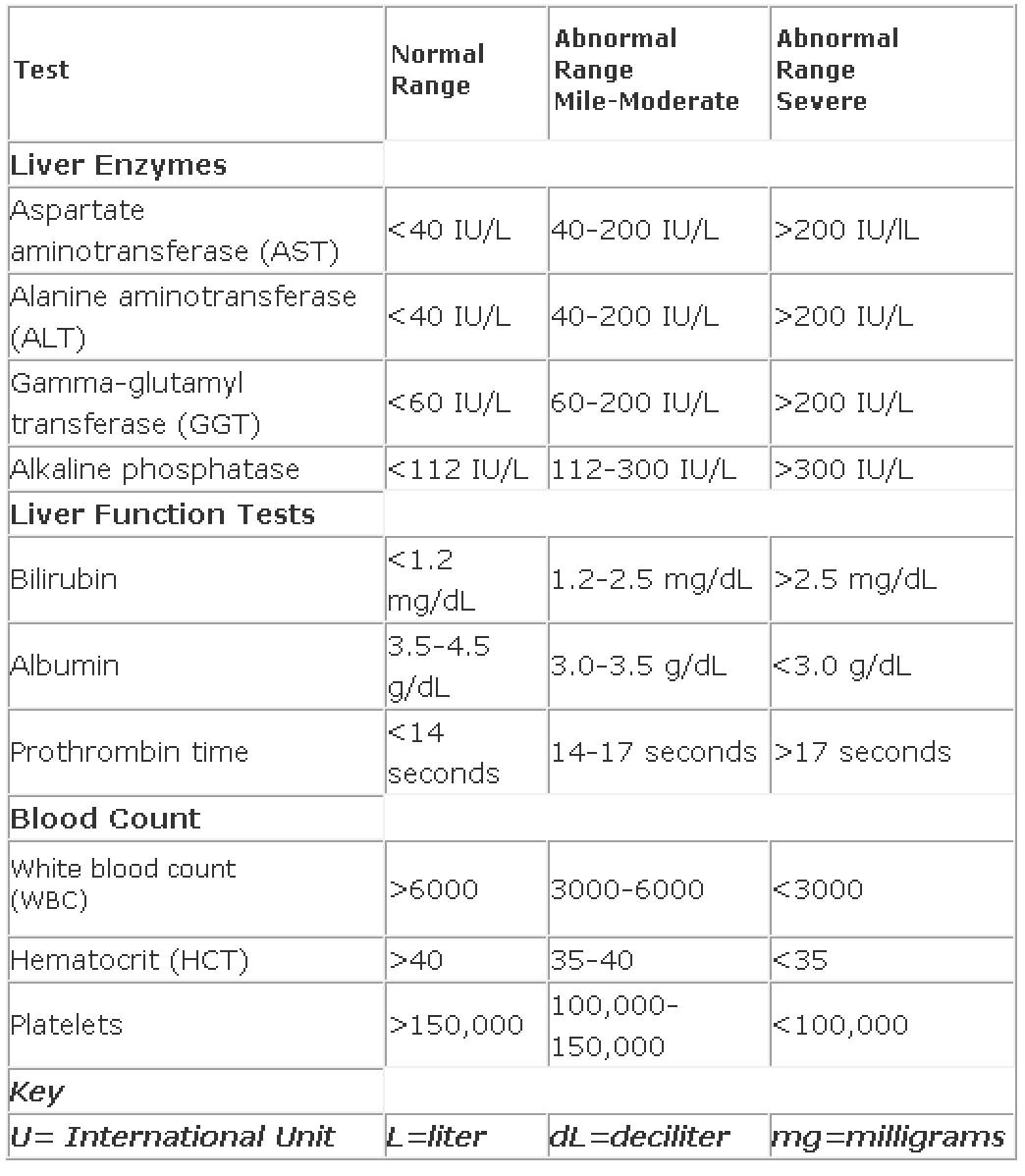
Liver function tests or liver enzymes
- ALT
- AST
Liver function tests also include ALP and total bilirubin, among other things.
Tests to measure liver scarring or fibrosis
- Liver Biopsy
- Elastography
- Serum markers
Imaging tests
Read Also: Should I Get Hepatitis B Vaccine
How To Treat Elevated Liver Enzymes Alt & Ast
Elevated liver enzymes usually are not a life-threatening condition, but high ALT and AST do warrant prompt medical attention. Chronic liver disease and cirrhosis caused more than 39,000 deaths in the United States in 2005, according to the Centers for Disease Control and Prevention, as well as the hospitalization of about 112,000 people1. Elevated ALT and AST indicate damage to your liver caused by disease or infection.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
Fill any prescriptions your doctor has recommended. Corticosteroids and pentoxifylline reduce inflammation of the liver. Ursodeoxycholic acid slows the progression of primary biliary cirrhosis. Antiviral medications reduce liver enzymes elevated by hepatitis C.
Take diuretics as prescribed by your physician. Diuretics remove excess fluid from the body. Your physician might prescribe antibiotics if you have cirrhosis or a liver problem caused by an infection.
Stop drinking alcohol immediately. Alcohol use can cause liver diseases, like cirrhosis and alcoholic hepatitis. Do not drink alcohol after you have recovered.
Lose weight. Obesity, either as the sole cause or in combination with other factors, is quickly becoming a risk factor for the development of cirrhosis, according to the National Digestive Diseases Information Clearinghouse. LabTestsOnline.org shows that cirrhosis elevates AST.
Mildly Elevated Liver Transaminase Levels: Causes And Evaluation
ROBERT C. OH, MD, MPH, Martin Army Community Hospital, Fort Benning, Georgia
THOMAS R. HUSTEAD, MD, Hardin Memorial Health, Elizabethtown, Kentucky
SYED M. ALI, MD, Fort Belvoir Community Hospital, Fort Belvoir, Virginia
MATTHEW W. PANTSARI, MD, Gastroenterology Consultants of Augusta, Augusta, Georgia
Am Fam Physician. 2017 Dec 1 96:709-715.
Patient information: See related handout on elevated liver enzymes, written by the authors of this article.
Mild, asymptomatic elevations of alanine transaminase and aspartate transaminase levels, defined as less than five times the upper limit of normal, are common in primary care. The prevalence of elevated transaminase levels is estimated to be approximately 10%, although less than 5% of these patients have a serious liver disease.1,2 Understanding the epidemiology of each condition that causes asymptomatic elevated transaminase levels can guide the evaluation.36 Elevations greater than five times the upper limit of normal should prompt immediate evaluation6 but are beyond the scope of this article.
WHAT IS NEW ON THIS TOPIC: MILDLY ELEVATED LIVER TRANSAMINASE LEVELS
The NAFLD fibrosis score is a calculator that uses clinical data to predict risk of liver-related complications and death from advanced disease. Clinicians should refer patients with a high NAFLD fibrosis score, increased risk of progression, or coexisting chronic liver disease to a gastroenterologist.
NAFLD = nonalcoholic fatty liver disease.
Don’t Miss: Pro Plan Hepatic Dog Food
What Is Hepatitis C
Hepatitis C is a liver disease caused by the hepatitis C virus , which is found in the blood of persons who have this disease. HCV is spread by contact with the blood of an infected person. Once exposed, 85% of these individuals become chronically infected, with a 15% chance of developing cirrhosis, which is scarring of the liver, over a 25 year time frame.
Can The Liver Repair Itself
Yes, the liver is a unique organ with a special way to regenerate itself from an injury and keeping the liver function. With an astonishing amount of blood running through it every day and a particular set of cells, the liver, to maintain its functions will activate unique mechanisms to keep the balance within the body.
The liver has the ability to repair itself after the removal of a part of the liver or an infection. After the liver injury, the organism activates a mechanism that is asleep under normal circumstances called mitosis, which is basically the replication of the cell.
After this happens, the liver can regenerate itself to its full size, but only the mass, as it does not recover the original shape.
However, if the damage is continuous and incisive, the regeneration mechanism will be exhausted and damaged. It wont have all that it needs to make replicas of the primary cells instead, it will create a scar , which produces more liver damage by inducing rearrangement of the blood circulation within the liver leading to chronic liver injury.
Read Also: Is There A Vaccine Available For Hepatitis B
Stages Of Liver Damage
The hepatitis C virus attacks your liver. Your immune system releases inflammatory substances in response. These substances stimulate your liver to produce fibrous proteins, like collagen to repair the damage. Collagen and other proteins can build up within the liver. This creates scar tissue.
A buildup of scar tissue in your liver is called fibrosis. It can prevent blood from flowing to your liver cells and change the function of your liver. Over time, the liver cells die and the liver no longer functions normally.
The METAVIR score is one method used to measure fibrosis in people with hepatitis C. Scoring is divided into five stages:
- stage 0: no fibrosis
What Are The Essential Functions Of The Liver
The liver is one of the most critical organs within the human body. Its location is in the right upper quadrant of the abdominal cavity and below the trunk it has several primary functions, which includes:
- Detoxification of various metabolites from the body.
- The synthesis of essential proteins.
- The production of digestive enzymes.
- Regulation of red blood cells.
- It has a unique role in metabolism, acting as a deposit for glucose asides from the synthesis of the same.
Therefore, to put all these terms in simple words, the primary liver function is to act as the main filter of the body. Fundamentally, by taking a vast amount of the blood flow from the digestive tract before passing it to the rest of the body.
To understand all the functions that the liver has, we are going to dig a little deeper within it. The liver cells name is Hepatocyte. It has a unique configuration that makes possible the accomplishment of the liver functions.
The liver cells have little bile canaliculi that receive all the bile acids synthesized within the cell. All of these canaliculi disembogue into the bile ducts. Eventually, the final destination is the gallbladder, with the deposit of bile acid, and salts of the body.
Recommended Reading: Is There A Vaccine For Hepatitis C Virus
Measurement Of Plasma Cytokines And Chemokines
Three human cytokine multiplex bead array assay kits utilizing technology licensed by Luminex were purchased from Bio-Rad to measure the following cytokines and chemokines:
-
Measured with Bio–Plex human TH17 15–plex: interleukin-1 beta , IL-4, IL-6, IL-10, IL-17A, IL-17 F, IL-21, IL-22, IL-23, IL-25,IL-31, IL-33, interferon-gamma , soluble CD40 ligand , and tumor necrosis factor alpha
-
Measured with Bio–Plex human cytokine Group I 9–plex: IL-2, IL-8, eotaxin-1 , IFN-, interferon-gamma inducible protein-10 , monocyte chemotactic protein 1 , macrophage inflammatory protein 1 alpha , MIP-1 , and regulated upon activation normal T-cell expressed and presumably secreted
-
Measured with Bio–Plex human cytokine Group II 3–plex: IL-18, TNF-, and TNF-related apoptosis-inducing ligand .
What Tests And Procedures Diagnose The Cause Of Abnormal Levels Of Liver Enzymes
There is a wide variety of tests and procedures that may help diagnose the cause of abnormal levels of liver enzymes. It goes from blood tests to take a portion of the liver and study the tissue and the extension of hepatocellular injury. Of course, a physician may not need all of these tests to diagnose the first and most important procedure is a good clinical history, family history of diseases, and a complete physical examination. However, here is a list of the most common tests.
- Liver Function Test
- Blood test
- Abdominal Ultrasonography
- Liver biopsy
- Computerized tomography
- Surface antibodies and antigens
All of these tests, with the correct use, will give the physician a complete insight into the disease. This enables the doctor to perform an assertive diagnosis, choose the specific treatment for the condition, and avoid any complications.
Also Check: Can You Catch Hepatitis C From Spit
What Medications Cause Abnormal Aminotransferase Levels
A host of medications can cause abnormal liver enzymes levels. Examples include:
- Pain relief medications such as aspirin, acetaminophen , ibuprofen , neproxen , diclofenac , and phenybutazone
- Anti-seizure medications such as phenytoin , valproic acid, carbamazepine , and phenobarbital
- Antibiotics such as the tetracyclines, sulfonamides, isoniazid , sulfamethoxazole, trimethoprim, nitrofurantoin, etc.
- Cholesterol lowering drugs such as the statins and niacin
- Cardiovascular drugs such as amiodarone , hydralazine, quinidine, etc.
- Anti-depressant drugs of the tricyclic type
With drug-induced liver enzyme abnormalities, the enzymes usually normalize weeks to months after stopping the medications.
What Are The Aminotransferases
The aminotransferases catalyze chemical reactions in the cells in which an amino group is transferred from a donor molecule to a recipient molecule. Hence, the names aminotransferases.
Medical terms can sometimes be confusing, as is the case with these enzymes. Another name for aminotransferase is transaminase. The enzyme aspartate aminotransferase is also known as serum glutamic oxaloacetic transaminase and alanine aminotransferase is also known as serum glutamic pyruvic transaminase . To put matters briefly, AST = SGOT and ALT = SGPT.
Also Check: Hepatitis B Vaccine Side Effects
Do Medical Conditions Outside The Liver Occur In Persons With Chronic Hepatitis C
A small percentage of persons with chronic hepatitis C develop medical conditions outside the liver . These conditions are thought to occur due to the body’s natural immune system fighting against itself. Such conditions include: glomerulonephritis associated with kidney disease, essential mixed cryoglobulinemia, and porphyria cutanea tarda-a skin condition.
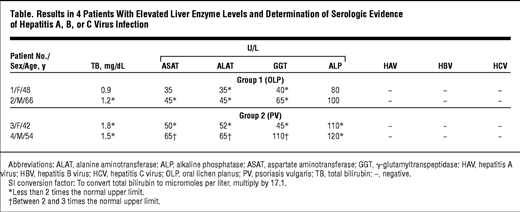
Bivariate Analysis Of Serum Alt Levels In Patients With Hcv Infection
The characteristics of individuals with HCV infection are given in Table . The estimated median duration of HCV infection was 58 mo. Steatosis was present in 22 of the 36 HCV infected patients, of whom 8 had grade 1, 11 grade 2, and 3 grade 3. The histological findings of the study participants are shown in Table . In bivariate correlation analyses, ALT levels correlated with duration of HCV infection ,1), HCV-RNA ,2), and the HAI .3). Among the components of the HAI, ALT concentrations were significantly associated with periportal bridging/necrosis and fibrosis .
You May Like: Hepatitis B Surface Ab Ql Reactive
Do Ast And Alt Tests Results Indicate Liver Function
Yes, both of them are transaminases and are indicatives of the liver function. However, they can also exist in other places within the body. Each one will have different importance in liver disease mainly due to its location.
The Aspartate Aminotransferase is a transaminase that is in the liver. Still, it exists in the heart, muscle, kidneys, brain, and pancreas, lungs, white and red blood cells. This is an essential factor within the diagnosis due to the multiple tissues where it can come from, making it a non-specific test for liver function. Abnormal levels of liver enzyme elevation, predominantly AST over ALT, may be due to Alcohol-related disease, chronic liver diseases, or non-hepatic diseases like thyroid diseases, myopathy, or extreme exercise.
On the other hand, there is the Alanine Aminotransferase . This transaminase exists only in deficient concentrations in other tissues. Therefore, it is primarily in the liver, making it a specific transaminase test for liver diseases. If abnormal levels of ALT are above AST, there are various causes like acute or chronic viral hepatitis, ischemic hepatitis, and autoimmune hepatitis, amongst others.
How Are Healthy People Evaluated For Mild To Moderate Rises In Aminotransferase Levels
Evaluation of healthy patients with abnormal liver enzymes needs to be individualized. A doctor may ask for blood test data from old records for comparison. If no old records are available, the doctor may repeat blood tests in weeks to months to see whether these abnormalities persist. The doctor will search for risk factors for hepatitis B and C including sexual exposures, history of blood transfusions, injectable drug use, and occupational exposure to blood products. A family history of liver disease may raise the possibility of inherited diseases such as hemachromatosis, Wilsons disease, or alpha-1- antitrypsin deficiency.
The pattern of liver enzyme abnormalities can provide useful clues to the cause of the liver disease. For example, the majority of patients with alcoholic liver disease have enzyme levels that are not as high as the levels reached with acute viral hepatitis and the AST tends to be above the ALT. Thus, in alcoholic liver disease, AST is usually under 300 units/liter while the ALT is usually under 100 units/ liter.
If alcohol or medication is responsible for the abnormal liver enzyme levels, stopping alcohol or the medication should bring the enzyme levels to normal or near normal levels in weeks to months. If obesity is suspected as the cause of fatty liver, weight reduction of 5% to 10% should also bring the liver enzyme levels to normal or near normal levels.
Read Also: Can You Get Rid Of Hepatitis B